| Revision as of 08:24, 17 February 2014 editDougsim (talk | contribs)Extended confirmed users8,815 edits →Calibration standards: table of quantities added← Previous edit | Revision as of 19:36, 25 February 2014 edit undoDougsim (talk | contribs)Extended confirmed users8,815 edits →Measures of Dose: units correctedNext edit → | ||
| Line 34: | Line 34: | ||
| ] | ] | ||
| ] | ] | ||
| There are a number of different measures of radiation dose, including ] (D) measured in ] (Gy), ] (H) measured in ]s (Sv), ] ( |
There are a number of different measures of radiation dose, including ] (''D'') measured in ] (Gy), ] (''H'') measured in ]s (Sv), ] (''E'') (also measured in sieverts) and ] (K) measured in grays, along with ] (DAP) and dose length product (DLP). Each measure is often simply described as ‘dose’, which can lead to confusion. Non-] units are still used, particularly in the USA, where dose is often reported in ] and dose equivalent in ]. By definition, 1 Gy = 100 rad and 1 Sv = 100 rem. | ||
| The fundamental measure of the biological effect of ionising radiation is the absorbed dose (D), which is defined as the mean energy imparted (dE) per unit mass (dm) of material (D = dE/dm)<ref name="Measurements 2011">International Commission on Radiation Units and Measurements (ICRU).Options for Characterizing Energy Deposition. Journal of the ICRU Vol 11 No 2 (2011) Report 86</ref> The SI unit of absorbed dose is the gray (Gy) defined as one joule per kilogram. Absorbed dose, as a point measurement, is suitable for describing localised (i.e. partial organ) exposures such as tumour dose in radiotherapy. It may be used to estimate stochastic risk provided the amount and type of tissue involved is stated. Localised diagnostic dose levels are typically in the 0-50 mGy range. At a dose of 1 milligray (mGy) of photon radiation, each cell nucleus is crossed by an average of 1 liberated electron track.<ref>Feinendegen LE. The cell dose concept; potential application in radiation protection. 1990 Phys. Med. Biol. 35 597</ref> | The fundamental measure of the biological effect of ionising radiation is the absorbed dose (''D''), which is defined as the mean energy imparted (dE) per unit mass (dm) of material (D = dE/dm)<ref name="Measurements 2011">International Commission on Radiation Units and Measurements (ICRU).Options for Characterizing Energy Deposition. Journal of the ICRU Vol 11 No 2 (2011) Report 86</ref> The SI unit of absorbed dose is the gray (Gy) defined as one joule per kilogram. Absorbed dose, as a point measurement, is suitable for describing localised (i.e. partial organ) exposures such as tumour dose in radiotherapy. It may be used to estimate stochastic risk provided the amount and type of tissue involved is stated. Localised diagnostic dose levels are typically in the 0-50 mGy range. At a dose of 1 milligray (mGy) of photon radiation, each cell nucleus is crossed by an average of 1 liberated electron track.<ref>Feinendegen LE. The cell dose concept; potential application in radiation protection. 1990 Phys. Med. Biol. 35 597</ref> | ||
| ===Equivalent Dose=== | ===Equivalent Dose=== | ||
| The absorbed dose required to produce a certain biological endpoint varies between different types of radiation, such as ], ] or ]. This is taken into account by the equivalent dose (H), which is defined as the mean dose to organ T by radiation type R (D<sub>T,R</sub>), multiplied by a weighting factor |
The absorbed dose required to produce a certain biological endpoint varies between different types of radiation, such as ], ] or ]. This is taken into account by the equivalent dose (H), which is defined as the mean dose to organ T by radiation type R (D<sub>T,R</sub>), multiplied by a weighting factor ''W''<sub>R</sub> designed to takes into account varying ] (RBE) of the radiation type,<ref name="Measurements 2011"/> i.e. for the same absorbed dose in Gy, alpha particles are 20 times as biologically potent as X or gamma rays. Note that the earlier measure of ‘dose equivalent’ is not organ averaged. Equivalent dose is primarily designed for estimation of stochastic risks from radiation exposures. Stochastic effects, which include cancer and hereditary effects are probabilistic in nature, theoretically resulting from mutation to a single cell. As dose is averaged over the whole organ; equivalent dose is rarely suitable for evaluation of acute radiation effects or tumour dose in radiotherapy. In the case of estimation of stochastic effects, assuming a ], this averaging out should make no difference as the total energy imparted remains the same. | ||
| {| class="wikitable" | {| class="wikitable" | ||
| Line 60: | Line 60: | ||
| ===Effective dose=== | ===Effective dose=== | ||
| It is difficult to compare the stochastic risk from localised exposures of different parts of the body (e.g. a chest x-ray compared to a CT scan of the head), or to compare exposures of the same body part but with different exposure patterns (e.g. a cardiac CT scan with a cardiac nuclear medicine scan). One way to avoid this problem is to simply average out a localised dose over the whole body. The problem of this approach is that the stochastic risk of cancer induction varies from one tissue to another. The effective dose (E) is designed to account for this variation by the application of specific weighting factors for each tissue (W<sub>T</sub>). Effective dose provides the equivalent whole body dose that gives the same risk as the localised exposure. It is defined as the sum of equivalent doses to each organ (H<sub>T</sub>), each multiplied by its respective tissue weighting factor ( |
It is difficult to compare the stochastic risk from localised exposures of different parts of the body (e.g. a chest x-ray compared to a CT scan of the head), or to compare exposures of the same body part but with different exposure patterns (e.g. a cardiac CT scan with a cardiac nuclear medicine scan). One way to avoid this problem is to simply average out a localised dose over the whole body. The problem of this approach is that the stochastic risk of cancer induction varies from one tissue to another. The effective dose (E) is designed to account for this variation by the application of specific weighting factors for each tissue (''W''<sub>T</sub>). Effective dose provides the equivalent whole body dose that gives the same risk as the localised exposure. It is defined as the sum of equivalent doses to each organ (''H''<sub>T</sub>), each multiplied by its respective tissue weighting factor (''W''<sub>T</sub>). | ||
| Weighting factors are calculated by the International Commission for Radiological Protection (ICRP), based on the risk of cancer induction for each organ and adjusted for associated lethality, quality of life and years of life lost. Organs that are remote from the site of irradiation will only receive a small equivalent dose (mainly due to scattering) and therefore contribute little to the effective dose, even if the weighting factor for that organ is high. Effective dose is used to estimate stochastic risks for typical examinations for a ‘reference’ person. It is not suitable for estimating stochastic risk for individual exposures to individual patients and should never be used to assess acute radiation effects. | Weighting factors are calculated by the International Commission for Radiological Protection (ICRP), based on the risk of cancer induction for each organ and adjusted for associated lethality, quality of life and years of life lost. Organs that are remote from the site of irradiation will only receive a small equivalent dose (mainly due to scattering) and therefore contribute little to the effective dose, even if the weighting factor for that organ is high. Effective dose is used to estimate stochastic risks for typical examinations for a ‘reference’ person. It is not suitable for estimating stochastic risk for individual exposures to individual patients and should never be used to assess acute radiation effects. | ||
Revision as of 19:36, 25 February 2014
| It has been suggested that Radiation Exposure Monitoring be merged into this article. (Discuss) Proposed since November 2012. |
Radiation dosimetry is the measurement and calculation of the radiation dose received by matter and tissue resulting from the exposure to indirect and direct ionizing radiation. It is a scientific sub-specialty in the fields of health physics and medical physics that is focused on the calculation and analysis of internal and external dose. Internal dose is calculated from a variety of physiological techniques, whilst external dose is measured with a dosimeter or inferred from other radiation instruments.
Dosimetry is used extensively for radiation protection and is routinely applied to occupational radiation workers, where a radiation dose is expected, but regulatory levels must not be exceeded. It is also used where radiation is unexpected, such as in the aftermath of the Three Mile Island, Chernobyl or Fukishima radiological release incidents, where the public dose is measured and calculated from a variety of indicators such as ambient measurements of radiation and radioactive contamination.
Other significant areas are medical dosimetry, where the required treatment dose and any collateral dose is monitored, and in environmental dosimetry, such as radon monitoring in buildings.
In all cases the information is used to calculate any likely detrimental health effects.
Measuring dose
External dose
There are several ways of measuring doses from ionizing radiation. People in occupational contact with radioactive substances or who may be exposed to radiation routinely carry personal dosimeters. These are specifically designed to record and indicate the dose received. Traditionally these were badges containing photographic film (film badge dosimeter), which would be chemically developed following exposure to indicate the total dose received. Film badges have now been largely replaced with other devices such as the TLD badge which uses Thermoluminescent dosimetry or optically stimulated luminescence (OSL) badges.
A number of electronic devices known as Electronic Personal Dosimeters (EPDs) have come into general use using semiconductor detection and programmable processor technology. These are worn as badges, but can give an indication of instantaneous dose rate and an audible and visual alarm if a dose rate or a total integrated dose is exceeded. A good deal of information can be made immediately available to the wearer of the recorded dose and current dose rate via a local display. They can be used as the main stand-alone dosimeter, or as a supplement to such as a TLD badge. These devices are particularly useful for real-time monitoring of dose where a high dose rate is expected which will time-limit the wearer's exposure.
The ICRP states that if a personal dosimeter is worn on a position on the body representative of its exposure, assuming whole-body exposure, the value of ambient dose equivalent H(10) is sufficient to provide an effective dose value suitable for radiological protection.
In certain circumstances dose can be inferred from readings taken by fixed instrumentation in an area in which the person concerned has been working. This would generally only be used if personal dosimetry had not been issued, or a personal dosimeter has been damaged or lost. Such calculations would take a pessimistic view of the likely received dose.
Internal Dose
Internal dosimetry is used to evaluate the radiation dose of the intake of radionuclides into the human body.
Medical dosimetry
Main article: Treatment planningMedical dosimetry is the calculation of absorbed dose and optimization of dose delivery in radiation therapy. It is often performed by a professional medical dosimetrist with specialized training in the field. In order to plan the delivery of radiation therapy, the radiation produced by the sources is usually characterized with percentage depth dose curves and dose profiles measured by medical physicists.
Environmental dosimetry
Envronmental Dosimetry is used where it is likely that the environment will generate a significant radiation dose. An example of this is radon monitoring. Radon is a radioactive gas generated by the decay of uranium, which is present in varying amounts in the earth's crust. Certain geographic areas, due to the underlying geology, continually generate radon which permeates it's way to the earth's surface. In some cases the dose can be significant in buildings where the gas can accumulate. A number of specialised dosimetry techniques are used to evaluate the dose that a building's occupants may receive.
Measures of Dose
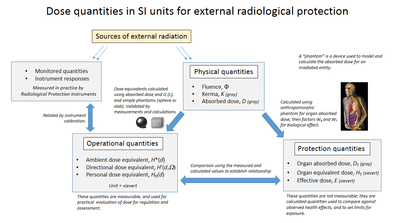

There are a number of different measures of radiation dose, including absorbed dose (D) measured in grays (Gy), Equivalent dose (H) measured in sieverts (Sv), Effective dose (E) (also measured in sieverts) and Kerma (K) measured in grays, along with dose area product (DAP) and dose length product (DLP). Each measure is often simply described as ‘dose’, which can lead to confusion. Non-SI units are still used, particularly in the USA, where dose is often reported in rads and dose equivalent in rems. By definition, 1 Gy = 100 rad and 1 Sv = 100 rem.
The fundamental measure of the biological effect of ionising radiation is the absorbed dose (D), which is defined as the mean energy imparted (dE) per unit mass (dm) of material (D = dE/dm) The SI unit of absorbed dose is the gray (Gy) defined as one joule per kilogram. Absorbed dose, as a point measurement, is suitable for describing localised (i.e. partial organ) exposures such as tumour dose in radiotherapy. It may be used to estimate stochastic risk provided the amount and type of tissue involved is stated. Localised diagnostic dose levels are typically in the 0-50 mGy range. At a dose of 1 milligray (mGy) of photon radiation, each cell nucleus is crossed by an average of 1 liberated electron track.
Equivalent Dose
The absorbed dose required to produce a certain biological endpoint varies between different types of radiation, such as photons, neutrons or alpha particles. This is taken into account by the equivalent dose (H), which is defined as the mean dose to organ T by radiation type R (DT,R), multiplied by a weighting factor WR designed to takes into account varying biological effectiveness (RBE) of the radiation type, i.e. for the same absorbed dose in Gy, alpha particles are 20 times as biologically potent as X or gamma rays. Note that the earlier measure of ‘dose equivalent’ is not organ averaged. Equivalent dose is primarily designed for estimation of stochastic risks from radiation exposures. Stochastic effects, which include cancer and hereditary effects are probabilistic in nature, theoretically resulting from mutation to a single cell. As dose is averaged over the whole organ; equivalent dose is rarely suitable for evaluation of acute radiation effects or tumour dose in radiotherapy. In the case of estimation of stochastic effects, assuming a linear dose response, this averaging out should make no difference as the total energy imparted remains the same.
| Radiation | Energy | WR (formerly Q) |
|---|---|---|
| x-rays, gamma rays, beta rays, muons |
1 | |
| neutrons | < 1 MeV | 2.5 + 18.2·e |
| 1 MeV - 50 MeV | 5.0 + 17.0·e | |
| > 50 MeV | 2.5 + 3.25·e | |
| protons, charged pions | 2 | |
| alpha rays, Nuclear fission products, heavy nuclei |
20 |
Effective dose
It is difficult to compare the stochastic risk from localised exposures of different parts of the body (e.g. a chest x-ray compared to a CT scan of the head), or to compare exposures of the same body part but with different exposure patterns (e.g. a cardiac CT scan with a cardiac nuclear medicine scan). One way to avoid this problem is to simply average out a localised dose over the whole body. The problem of this approach is that the stochastic risk of cancer induction varies from one tissue to another. The effective dose (E) is designed to account for this variation by the application of specific weighting factors for each tissue (WT). Effective dose provides the equivalent whole body dose that gives the same risk as the localised exposure. It is defined as the sum of equivalent doses to each organ (HT), each multiplied by its respective tissue weighting factor (WT).
Weighting factors are calculated by the International Commission for Radiological Protection (ICRP), based on the risk of cancer induction for each organ and adjusted for associated lethality, quality of life and years of life lost. Organs that are remote from the site of irradiation will only receive a small equivalent dose (mainly due to scattering) and therefore contribute little to the effective dose, even if the weighting factor for that organ is high. Effective dose is used to estimate stochastic risks for typical examinations for a ‘reference’ person. It is not suitable for estimating stochastic risk for individual exposures to individual patients and should never be used to assess acute radiation effects.
| Organs | Tissue weighting factors | ||
|---|---|---|---|
| ICRP30(I36) 1979 |
ICRP60(I3) 1991 |
ICRP103(I6) 2008 | |
| Gonads | 0.25 | 0.20 | 0.08 |
| Red Bone Marrow | 0.12 | 0.12 | 0.12 |
| Colon | - | 0.12 | 0.12 |
| Lung | 0.12 | 0.12 | 0.12 |
| Stomach | - | 0.12 | 0.12 |
| Breasts | 0.15 | 0.05 | 0.12 |
| Bladder | - | 0.05 | 0.04 |
| Liver | - | 0.05 | 0.04 |
| Oesophagus | - | 0.05 | 0.04 |
| Thyroid | 0.03 | 0.05 | 0.04 |
| Skin | - | 0.01 | 0.01 |
| Bone surface | 0.03 | 0.01 | 0.01 |
| Salivary glands | - | - | 0.01 |
| Brain | - | - | 0.01 |
| Remainder of body | 0.30 | 0.05 | 0.12 |
Dose versus activity
Radiation dose refers to the amount of energy deposited in matter and/or biological effects of radiation, and should not be confused with the unit of radioactive activity (becquerel, Bq). Exposure to a radioactive source will give a dose which is dependent on the activity, duration of exposure, energy of the radiation emitted, distance from the source and shielding. The equivalent dose is then dependent upon the weighting factors above. Dose is a measure of deposited dose, and therefore can never go down—removal of a radioactive source can only reduce the rate of increase of absorbed dose, never the total absorbed dose.
The worldwide average background dose for a human being is about 3.5 mSv per year , mostly from cosmic radiation and natural isotopes in the earth. The largest single source of radiation exposure to the general public is naturally-occurring radon gas, which comprises approximately 55% of the annual background dose. It is estimated that radon is responsible for 10% of lung cancers in the United States.
Calibration standards
Because the human body is approximately 70% water and has an overall density close to 1 g/cm, dose measurement is usually calculated and calibrated as dose to water.
National standards laboratories such as the NPL provide calibration factors for ionization chambers and other measurement devices to convert from the instrument's readout to absorbed dose. The standards laboratories operate a Primary Standard, which is normally calibrated by absolute calorimetry, the warming of substances when they absorb energy. A user sends their Secondary Standard to the laboratory, where it is exposed to a known amount of radiation (derived from the Primary Standard) and a factor is issued to convert the instrument's reading to that dose. The user may then use their Secondary Standard to derive calibration factors for other instruments they use, which then become tertiary standards, or field instruments.
The NPL in the UK operates a graphite-calorimeter for absolute photon dosimetry. Graphite is used instead of water as its specific heat capacity is one-sixth that of water and therefore the temperature rises in graphite are 6 times more than the equivalent in water and measurements are more accurate. Significant problems exist in insulating the graphite from the laboratory in order to measure the tiny temperature changes. A lethal dose of radiation to a human is approximately 10–20 Gy. This is 10-20 joules per kilogram. A 1 cm piece of graphite weighing 2 grams would therefore absorb around 20–40 mJ. With a specific heat capacity of around 700 J·kg·K, this equates to a temperature rise of just 20 mK.
Dosimeters in radiotherapy (linear particle accelerator in external beam therapy) are routinely calibrated using ionization chambers or the new and more accurate diode technology.
Radiation-related quantities
The following table shows radiation quantities in SI and non-SI units.
| Quantity | Name | Symbol | Unit | Year | System |
|---|---|---|---|---|---|
| Exposure (X) | röntgen | R | esu / 0.001293 g of air | 1928 | non-SI |
| Absorbed dose (D) | erg•g | 1950 | non-SI | ||
| rad | rad | 100 erg•g | 1953 | non-SI | |
| gray | Gy | J•kg | 1974 | SI | |
| Activity (A) | curie | c | 3.7 × 10 s | 1953 | non-SI |
| becquerel | Bq | s | 1974 | SI | |
| Dose equivalent (H) | röntgen equivalent man | rem | 100 erg•g | 1971 | non-SI |
| sievert | Sv | J•kg | 1977 | SI | |
| Fluence (Φ) | (reciprocal area) | cm or m | 1962 | SI (m) |
Although the United States Nuclear Regulatory Commission permits the use of the units curie, rad, and rem alongside SI units, the European Union European units of measurement directives required that their use for "public health ... purposes" be phased out by 31 December 1985.
Radiation exposure monitoring
Records of legal dosimetry results are usually kept for a set period of time, depending upon the legal requirements of the nation in which they are used.
medical radiation exposure monitoring is the practice of collecting dose information from radiology equipment and using the data to help identify opportunities to reduce unnecessary dose in medical situations.
See also
- Computational human phantom
- Dosimeter
- Health physics
- Health effects of radon
- Radiation dose reconstruction
References
- ICRP pub 103 para 138
- ^ International Commission on Radiation Units and Measurements (ICRU).Options for Characterizing Energy Deposition. Journal of the ICRU Vol 11 No 2 (2011) Report 86
- Feinendegen LE. The cell dose concept; potential application in radiation protection. 1990 Phys. Med. Biol. 35 597
- "The 2007 Recommendations of the International Commission on Radiological Protection". Annals of the ICRP. ICRP publication 103. 37 (2–4). 2007. ISBN 978-0-7020-3048-2. Retrieved 17 May 2012.
- UNSCEAR-2008 Annex A page 40, table A1, retrieved 2011-7-20
- 10 CFR 20.1004. US Nuclear Regulatory Commission. 2009.
- The Council of the European Communities (1979-12-21). "Council Directive 80/181/EEC of 20 December 1979 on the approximation of the laws of the Member States relating to Unit of measurement and on the repeal of Directive 71/354/EEC". Retrieved 19 May 2012.
External links
- Eurados - The European radiation dosimetry group
- Nucleonica Wiki on Dosimetry & Shielding
- Nucleonica website
- The Karlsruhe Nuclide Chart
- Tim Stephens and Keith Pantridge, 'Dosimetry, Personal Monitoring Film' (a short article on Dosimetry from the point of view of its relation to photography, in Philosophy of Photography, volume 2, number 2, 2011, pp. 153–158.)