Medical condition
| Febrile seizure | |
|---|---|
| Other names | Fever fit, febrile convulsion |
 | |
| An analog medical thermometer showing a temperature of 38.8 °C or 101.8 °F | |
| Specialty | Emergency medicine, neurology |
| Symptoms | Tonic-clonic seizure |
| Usual onset | Ages of 6 months to 5 years |
| Duration | Typically less than 5 minutes |
| Types | Simple, complex |
| Causes | High body temperature |
| Risk factors | Family history |
| Differential diagnosis | Meningitis, metabolic disorders |
| Treatment | Supportive care |
| Medication | Benzodiazepines (rarely needed) |
| Prognosis | Good |
| Frequency | ~5% of children |
A febrile seizure, also known as a fever fit or febrile convulsion, is a seizure associated with a high body temperature but without any serious underlying health issue. They most commonly occur in children between the ages of 6 months and 5 years. Most seizures are less than five minutes in duration, and the child is completely back to normal within an hour of the event. There are two types: simple febrile seizures and complex febrile seizures. Simple febrile seizures involve an otherwise healthy child who has at most one tonic-clonic seizure lasting less than 15 minutes in a 24-hour period. Complex febrile seizures have focal symptoms, last longer than 15 minutes, or occur more than once within 24 hours. About 80% are classified as simple febrile seizures.
Febrile seizures are triggered by fever, typically due to a viral infection. They may run in families. The underlying mechanism is not fully known, but it is thought to involve genetics, environmental factors, brain immaturity, and inflammatory mediators. The diagnosis involves verifying that there is not an infection of the brain, there are no metabolic problems, and there have not been prior seizures that have occurred without a fever. Blood testing, imaging of the brain, or an electroencephalogram (EEG) is typically not needed. Examination to determine the source of the fever is recommended. In otherwise healthy-looking children a lumbar puncture is not necessarily required.
Neither anti-seizure medication nor anti-fever medication are recommended in an effort to prevent further simple febrile seizures. In the few cases that last greater than 5 minutes, a benzodiazepine such as lorazepam or midazolam may be used. Efforts to rapidly cool during a seizure is not recommended.
Febrile seizures affect 2–10% of children. They are more common in boys than girls. After a single febrile seizure there is an approximately 35% chance of having another one during childhood. Outcomes are generally excellent with similar academic achievements to other children and no change in the risk of death for those with simple seizures. There is tentative evidence that affected children have a slightly increased risk of epilepsy at 2% compared to the general population.
Signs and symptoms
Signs and symptoms depend on if the febrile seizure is simple versus complex. In general, the child's temperature is greater than 38 °C (100.4 °F), although most have a fever of 39 °C (102.2 °F) or higher. Most febrile seizures will occur during the first 24 hours of developing a fever. Signs of typical seizure activity include loss of consciousness, opened eyes which may be deviated or appear to be looking towards one direction, irregular breathing, increased secretions or foaming at the mouth, and the child may look pale or blue (cyanotic). They may become incontinent (wet or soil themselves) and may also vomit.
Types
There are two types of febrile seizures: simple and complex. Febrile status epilepticus is a subtype of complex febrile seizures that lasts for longer than 30 minutes. It can occur in up to 5% of febrile seizure cases.
| Simple | Complex | |
|---|---|---|
| Characteristics | Generalized tonic clonic movements (stiffening and shaking of arms and legs) | Focal movements (usually affecting a single limb or side of the body) |
| Duration | <15 minutes (with most lasting <5 minutes) | >15 minutes |
| Postictal state | None or short period of drowsiness | Longer period of drowsiness; may experience Todd's paralysis |
| Recurrence | No recurrence in the first 24 hours | May recur in the first 24 hours |
Causes
| Type | OMIM | Gene |
|---|---|---|
| FEB3A | 604403 | SCN1A |
| FEB3B | 604403 | SCN9A |
| FEB4 | 604352 | GPR98 |
| FEB8 | 611277 | GABRG2 |
Febrile seizures are due to fevers, usually those greater than 38 °C (100.4 °F). The cause of the fevers is often a viral illness. The likelihood of a febrile seizure is related to how high the temperature reaches. Some feel that the rate of increase is not important while others feel the rate of increase is a risk factor. This latter position has not been proven.
In children, illnesses that often cause a fever include middle ear infections and viral upper respiratory infections. Other infections associated with febrile seizures include Shigellosis, Salmonellosis, and Roseola. Although the exact mechanism is unknown, it is speculated that these infections may affect the brain directly or via a neurotoxin leading to seizures.
There is a small chance of a febrile seizure after certain vaccines. The risk is only slightly increased for a few days after receiving one of the implicated vaccines during the time when the child is likely to develop a fever as a natural immune response. Implicated vaccines include:
- measles/mumps/rubella/varicella
- combined diphtheria/tetanus/acellular pertussis/polio/Haemophilus influenzae type b
- diphtheria-tetanus-whole-cell pertussis, which is not used in North America anymore
- some versions of the pneumococcal vaccine
- some types of inactivated influenza vaccine
It was previously thought that febrile seizures were more likely to occur with the combined MMRV vaccine, but recent studies have found there to be no significant increase. Overall, febrile seizures triggered by vaccines are uncommon. Children who have a genetic predisposition towards febrile seizures are more likely to have one after vaccination.
The seizures occur, by definition, without an intracranial infection or metabolic problems. They run in families with reported family history in approximately 33% of people. Several genetic associations have been identified, including GEFS+ and Dravet Syndrome. Possible modes of inheritance for genetic predisposition to febrile seizures include autosomal dominance with reduced penetrance and polygenic multifactorial inheritance. An association with iron deficiency has also been reported, particularly in the developing world.
Mechanism
The exact underlying mechanism of febrile seizures is still unknown, but it is thought to be multi-factorial involving genetic and environmental factors. Speculation includes immaturity of the central nervous system at younger ages, making the brain more vulnerable to the effects of fever. The increased activity of neurons during rapid brain development, may help explain why children, particularly younger than age 3, are prone to febrile seizures, with occurrences decreasing after age 5. Other proposed mechanisms include the interactions of inflammatory mediators, particularly cytokines, which are released during a fever, causing elevated temperatures in the brain, which may somehow lead to a seizure. Specific cytokines implicated include elevated CSF IL-1β and serum IL-6.
Diagnosis
The diagnosis is made by eliminating more serious causes of seizure and fever: in particular, meningitis and encephalitis. However, in children who are immunized against pneumococcal and Haemophilus influenzae, the risk of bacterial meningitis is low. If a child has recovered and is acting normally, bacterial meningitis is very unlikely, making further procedures such as a lumbar puncture unnecessary.
Diagnosis involves gathering a detailed history including the value of highest temperature recorded, timing of seizure and fever, seizure characteristics, time to return to baseline, vaccination history, illness exposures, family history, etc.; and performing a physical exam that looks for signs of infection including meningitis and neurological status. Blood tests, imaging of the brain and an electroencephalogram are generally not needed. However, for complex febrile seizures, EEG and imaging with an MRI of the brain may be helpful.
Lumbar puncture is recommended if there are obvious signs and symptoms of meningitis or if there is high clinical suspicion. However, lumbar puncture is an option that may be considered in children younger than 12 months of age since signs and symptoms of meningitis may be atypical, if the child does not return to baseline, or if the child lacks immunization against Haemophilus influenzae and pneumococcal or vaccination status is unknown.
Differential diagnosis includes other causes of seizures such as CNS infections (i.e. meningitis, encephalitis), metabolic disturbances (i.e. electrolyte imbalances), CNS trauma, drug use and/or withdrawal, genetic conditions (i.e. GEFS+), FIRES, shivering, febrile delirium, febrile myoclonus, breath holding spells, and convulsive syncope. However, febrile seizures are still the most likely cause of convulsions in children under the age of 5 years old.
Prevention
There is no benefit from the use of phenytoin, valproate, ibuprofen, diclofenac, acetaminophen, pyridoxine, or zinc sulfate. There is no evidence to support administering fever reducing medications such as acetaminophen at the time of a febrile seizure or to prevent the rate of recurrence. Rapid cooling methods such as an ice bath or a cold bath should be avoided as a method to lower the child's temperature, especially during a febrile seizure.
There is a decrease of recurrent febrile seizures with intermittent diazepam and phenobarbital but there is a high rate of adverse effects. They are thus not recommended as an effort to prevent further seizures.
Treatment
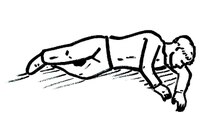
If a child is having a febrile seizure, the following recommendations are made for caregivers:
- Note the start time of the seizure. If the seizure lasts longer than 5 minutes, call an ambulance. Medication to stop seizure, such as rectal diazepam or intranasal midazolam may be used. The child should be taken immediately to the nearest medical facility for further diagnosis and treatment.
- Gradually place the child on a protected surface such as the floor or ground to prevent accidental injury. Do not restrain or hold a child during a convulsion.
- Position the child on his or her side or stomach to prevent choking. When possible, gently remove any objects from the child's mouth. Nothing should ever be placed in the child's mouth during a convulsion. These objects can obstruct the child's airway and make breathing difficult.
- Seek immediate medical attention if this is the child's first febrile seizure and take the child to the doctor once the seizure has ended to check for the cause of the fever. This is especially urgent if the child shows symptoms of stiff neck, extreme lethargy, or abundant vomiting, which may be signs of meningitis, an infection over the brain surface.
In those with a single seizure lasting greater than 5 minutes or two consecutive seizures lasting greater than 5 minutes in which the person has not returned to their baseline mental status, defined as status epilepticus, intravenous lorazepam, rectal diazepam, or intranasal midazolam is recommended. Anti-seizure medication are used in status epilepticus in an effort to prevent complications such as injury to the hippocampus or temporal lobe epilepsy.
Secondary causes of a seizure should be addressed if present. Questions that may be asked of the caregivers who witnessed the seizure include the length of the seizure, the timing of the day, loss of consciousness, loss of bowel or urinary continence, a period of altered level of consciousness or confusion once the seizure stopped, movement of the eyes to a specific side, recent infections, recent medication usage including antibiotics or fever reducer medications, family history of febrile and afebrile seizures, vaccination and travel history.
Vital signs should be monitored in the emergency department along with observation for 6 hours. Evaluation for the cause of fever should be performed including signs of an infection such as a bulging tympanic membrane (otitis media), red pharynx, enlarged tonsils, enlarged cervical lymph nodes (streptococcal pharyngitis or infectious mononucleosis), and a widespread rash. CNS infections such as meningitis, encephalitis and brain abscesses should be ruled out, along with electrolyte abnormalities.
Prognosis
Long term outcomes are generally good with little risk of neurological problems or epilepsy. Those who have one febrile seizure have an approximately 30- 40% chance of having another one in the next two years, with the risk being greater in those who are younger.
Simple febrile seizures do not tend to recur frequently (children tend to outgrow them) and do not make the development of adult epilepsy significantly more likely (about 3–5%) compared with the general public (1%). Children with febrile convulsions are more likely to have a febrile seizure in the future if they were young at their first seizure (less than 18 months old), have a family history of a febrile convulsions in first-degree relatives (a parent or sibling), have a short time between the onset of fever and the seizure, had a low degree of fever before their seizure, or have a seizure history of abnormal neurological signs or developmental delay. Similarly, the prognosis after a complex febrile seizure is excellent, although an increased risk of death has been shown for complex febrile seizures, partly related to underlying conditions.
Epidemiology
Febrile seizures happen between the ages of 6 months and 5 years. The peak age for a febrile seizure is 18 months, with the most common age range being 12–30 months of age. They affect between 2-5% of children. They are more common in boys than girls. Febrile seizures can occur in any ethnic group, although there have been higher rates in Guamanians (14%), Japanese (6-9%) and Indians (5-10%).
References
- ^ Graves RC, Oehler K, Tingle LE (January 2012). "Febrile seizures: risks, evaluation, and prognosis". American Family Physician. 85 (2): 149–53. PMID 22335215.
- ^ Gupta A (February 2016). "Febrile Seizures". Continuum (Minneapolis, Minn.). 22 (1 Epilepsy): 51–9. doi:10.1212/CON.0000000000000274. PMID 26844730. S2CID 33033538.
- ^ Xixis KL, Keenaghan M (2019), "Febrile Seizure", StatPearls, StatPearls Publishing, PMID 28846243, retrieved 13 January 2020
- ^ "Symptoms of febrile seizures". www.nhs.uk. 1 October 2012. Archived from the original on 6 October 2014. Retrieved 13 October 2014.
- ^ Roddy SM, McBride MC (2017). "Chapter 327: Seizure Disorders". In McInerny TK (ed.). American Academy of Pediatrics Textbook of Pediatric Care (2nd ed.). : American Academy of Pediatrics. ISBN 978-1-61002-047-3. OCLC 952123506.
- ^ Leung AK, Hon KL, Leung TN (2018). "Febrile seizures: an overview". Drugs in Context. 7: 212536. doi:10.7573/dic.212536. PMC 6052913. PMID 30038660.
- ^ Patel N, Ram D, Swiderska N, Mewasingh LD, Newton RW, Offringa M (August 2015). "Febrile seizures". BMJ. 351: h4240. doi:10.1136/bmj.h4240. PMID 26286537. S2CID 35218071.
- ^ Kwon A, Kwak BO, Kim K, Ha J, Kim SJ, Bae SH, Son JS, Kim SN, Lee R (2018). "Cytokine levels in febrile seizure patients: A systematic review and meta-analysis". Seizure. 59: 5–10. doi:10.1016/j.seizure.2018.04.023. PMID 29727742.
- ^ Offringa M, Newton R, Nevitt SJ, Vraka K (16 June 2021). "Prophylactic drug management for febrile seizures in children". The Cochrane Database of Systematic Reviews. 2021 (6): CD003031. doi:10.1002/14651858.CD003031.pub4. ISSN 1469-493X. PMC 8207248. PMID 34131913.
- Prasad P (2013). Pocket Pediatrics: The Massachusetts General Hospital for Children Handbook of Pediatrics. Lippincott Williams & Wilkins. p. 419. ISBN 9781469830094. Archived from the original on 6 September 2017.
- ^ "Febrile Seizures". familydoctor.org. Retrieved 24 January 2020.
- ^ Ronald M. Perkin, ed. (2008). Pediatric hospital medicine : textbook of inpatient management (2nd ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 266. ISBN 9780781770323. Archived from the original on 6 September 2017.
- Ahmad S, Marsh ED (September 2010). "Febrile status epilepticus: current state of clinical and basic research". Seminars in Pediatric Neurology. 17 (3): 150–4. doi:10.1016/j.spen.2010.06.004. PMID 20727483.
- ^ Subcommittee on Febrile Seizures (1 February 2011). "Febrile Seizures: Guideline for the Neurodiagnostic Evaluation of the Child With a Simple Febrile Seizure". Pediatrics. 127 (2): 389–394. doi:10.1542/peds.2010-3318. ISSN 0031-4005. PMID 21285335.
- ^ Nakayama J, Arinami T (August 2006). "Molecular genetics of febrile seizures". Epilepsy Research. 70 (Suppl 1): S190-8. doi:10.1016/j.eplepsyres.2005.11.023. PMID 16887333. S2CID 34951349.
- Greenberg DA, Aminoff MJ, Simon RP (2012). "12". Clinical neurology (8th ed.). New York: McGraw-Hill Medical. ISBN 978-0071759052.
- ^ Engel J (2008). Epilepsy: a comprehensive textbook (2nd ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 661. ISBN 9780781757775. Archived from the original on 6 September 2017.
- ^ Monfries N, Goldman RD (February 2017). "Prophylactic antipyretics for prevention of febrile seizures following vaccination". Canadian Family Physician. 63 (2): 128–130. PMC 5395384. PMID 28209678.
- ^ Ma SJ, Xiong YQ, Jiang LN, Chen Q (2015). "Risk of febrile seizure after measles–mumps–rubella–varicella vaccine: A systematic review and meta-analysis". Vaccine. 33 (31): 3636–3649. doi:10.1016/j.vaccine.2015.06.009. PMID 26073015.
- ^ Whelan H, Harmelink M, Chou E, Sallowm D, Khan N, Patil R, Sannagowdara K, Kim JH, Chen WL, Khalil S, Bajic I (2017). "Complex febrile seizures—A systematic review". Disease-a-Month. 63 (1): 5–23. doi:10.1016/j.disamonth.2016.12.001. PMID 28089358.
- King D, King A (October 2014). "Question 2: Should children who have a febrile seizure be screened for iron deficiency?". Archives of Disease in Childhood. 99 (10): 960–4. doi:10.1136/archdischild-2014-306689. PMID 25217390. S2CID 43130862.
- Kwak BO, Kim K, Kim SN, Lee R (November 2017). "Relationship between iron deficiency anemia and febrile seizures in children: A systematic review and meta-analysis". Seizure. 52: 27–34. doi:10.1016/j.seizure.2017.09.009. PMID 28957722.
- Shah PB, James S, Elayaraja S (9 April 2020). "EEG for children with complex febrile seizures". The Cochrane Database of Systematic Reviews. 2020 (4): CD009196. doi:10.1002/14651858.CD009196.pub5. ISSN 1469-493X. PMC 7142325. PMID 32270497.
- Wilmshurst JM, Gaillard WD, Vinayan KP, Tsuchida TN, Plouin P, Van Bogaert P, Carrizosa J, Elia M, Craiu D, Jovic NJ, Nordli D (August 2015). "Summary of recommendations for the management of infantile seizures: Task Force Report for the ILAE Commission of Pediatrics". Epilepsia. 56 (8): 1185–1197. doi:10.1111/epi.13057. ISSN 1528-1167. PMID 26122601. S2CID 13707556.
- ^ "Febrile Seizures Fact Sheet. National Institute of Neurological Disorders and Stroke". www.ninds.nih.gov. Archived from the original on 28 July 2017. Retrieved 9 August 2017.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- Seinfeld S, Goodkin HP, Shinnar S (March 2016). "Status Epilepticus". Cold Spring Harbor Perspectives in Medicine. 6 (3): a022830. doi:10.1101/cshperspect.a022830. PMC 4772080. PMID 26931807.
- Shinnar S, Glauser TA (January 2002). "Febrile seizures". Journal of Child Neurology. 17 (Suppl 1): S44-52. doi:10.1177/08830738020170010601. PMID 11918463. S2CID 11876657.
- Vestergaard M, Pedersen MG, Ostergaard JR, Pedersen CB, Olsen J, Christensen J (August 2008). "Death in children with febrile seizures: a population-based cohort study". Lancet. 372 (9637): 457–63. doi:10.1016/S0140-6736(08)61198-8. PMID 18692714. S2CID 17305241.
- ^ Cerisola A, Chaibún E, Rosas M, Cibils L (2018). "". Medicina. 78 (Suppl 2): 18–24. PMID 30199360.
- Waruiru C, Appleton R (August 2004). "Febrile seizures: an update". Archives of Disease in Childhood. 89 (8): 751–6. doi:10.1136/adc.2003.028449. PMC 1720014. PMID 15269077.
- Patterson JL, Carapetian SA, Hageman JR, Kelley KR (December 2013). "Febrile seizures". Pediatric Annals. 42 (12): 249–54. doi:10.3928/00904481-20131122-09. PMID 24295158.
External links
| Classification | D |
|---|---|
| External resources |
| Seizures and epilepsy | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Basics | |||||||||
| Management |
| ||||||||
| Personal issues | |||||||||
| Seizure types |
| ||||||||
| Related disorders | |||||||||
| Organizations | |||||||||