
The effects of climate change on human health are profound because they increase heat-related illnesses and deaths, respiratory diseases, and the spread of infectious diseases. There is widespread agreement among researchers, health professionals and organizations that climate change is the biggest global health threat of the 21st century.
Rising temperatures and changes in weather patterns are increasing the severity of heat waves, extreme weather and other causes of illness, injury or death. Heat waves and extreme weather events have a big impact on health both directly and indirectly. When people are exposed to higher temperatures for longer time periods they might experience heat illness and heat-related death.
In addition to direct impacts, climate change and extreme weather events cause changes in the biosphere. Climate change will impact where infectious diseases are able to spread in the future. Many infectious diseases will spread to new geographic areas where people have not previously been exposed to them. Certain diseases that are carried and spread by living hosts such as mosquitoes and ticks (known as vectors) may become more common in some regions. Affected diseases include dengue fever and malaria. Contracting waterborne diseases such as diarrhoeal disease will also be more likely.
Changes in climate can cause decreasing yields for some crops and regions, resulting in higher food prices, less available food, and undernutrition. Climate change can also reduce access to clean and safe water supply. Extreme weather and its health impact can also threaten the livelihoods and economic stability of people. These factors together can lead to increasing poverty, human migration, violent conflict, and mental health issues.
Climate change affects human health at all ages, from infancy through adolescence, adulthood and old age. Factors such as age, gender and socioeconomic status influence to what extent these effects become wide-spread risks to human health. Some groups are more vulnerable than others to the health effects of climate change. These include children, the elderly, outdoor workers and disadvantaged people.
Overview of health effects and pathways
The effects of climate change on human health can be grouped into direct and indirect effects. Extreme weather, including increased storms, floods, droughts, heat waves and wildfires can directly cause injury, illness, or death. The indirect impact of climate change happens through changes in the environment that alter the Earth's natural systems on a large-scale. These include worsening water quality, air pollution, reduced food availability, and faster spread of disease-carrying insects.
Both direct and indirect health effects and their impact vary across the world and between different groups of people according to age, gender, mobility and other factors. For example, differences in health service provision or economic development will result in different health risks and outcomes for people in different regions, with less developed countries facing greater health risks. In many places, the combination of lower socioeconomic status and gender roles result in increased health risks to women and girls as a result of climate change, compared to those faced by men and boys (although the converse may apply in other instances).
The various health effects that are related to climate change include cardiovascular diseases, respiratory diseases, infectious diseases, undernutrition, mental illness, allergies, injuries and poisoning.
The provision of health care can also be impacted by the collapse of health systems and damage to infrastructure due to climate-induced events such as flooding. Therefore, building health systems that are climate resilient is a priority.
Health risks from extreme weather and climate events
Further information: Effects_of_climate_change § Weather, and Extreme weatherClimate change is increasing the frequency and intensity of some extreme weather events. Extreme heat and cold events are the most likely to increase and worsen followed by more frequent heavy rain or snow and increases in the intensity of droughts.
Extreme weather events, such as floods, hurricanes, heatwaves, droughts and wildfires can result in injuries, death and the spread of infectious diseases. For example, local epidemics can occur due to loss of infrastructure, such as hospitals and sanitation services, but also because of climate changes creating a more suitable weather for disease-carrying organisms.
Heat
Further information: Heat illnessSince the 1970s, temperature on the surface of Earth has become warmer each decade. This increase happened faster than in any other 50-year period over at least the last 2000 years. Compared to the second half of the 19th century, temperature in the 21st century show a warming of 1.09 °C.
Extreme heat is a direct threat to health, especially for people over 65 years, children, people living in cities and those who have already existing health conditions. Rising global temperatures impact the health and wellbeing of people in multiple ways. In the last few decades, people all over the world have become more vulnerable to heat and experienced an increasing number of life-threatening heatwave events. Extreme heat has negative effects on mental health as well, raising the risk of mental health-related hospitalisations and suicidality.
Physical exercise is beneficial for reducing the risk the many illnesses and for mental health. At the same time the number of hours per day when the temperature is dangerously high for outdoor exercise has been increasing. The rising heat also impacts people's ability to work and the number of hours when it is not safe to work outdoors (construction, agriculture, etc.) has also increased.
It is estimated that between 1960 and 1990, climate change has put over 600 million people (9% of the global population) outside the human climate niche which is the average temperature range in which people have been able to thrive in the past 6,000 years. Unless greenhouse gas emissions are reduced, regions inhabited by a third of the human population could become as hot as the hottest parts of the Sahara within 50 years. The projected annual average temperature of above 29 °C for these regions would be outside the biologically suitable temperature range for humans.
Heat-related health effects for vulnerable people
Further information: Effects of climate change § Heatwaves, and Heat illness
Exposure to extreme heat poses an acute health hazard, especially for people deemed as vulnerable. Vulnerable people with regard to heat illnesses include people with low incomes, minority groups, women (in particular pregnant women), children, older adults (over 65 years old), people with chronic diseases, disabilities and multiple long-term health conditions. Other people at risk include those living in urban environments (due to the urban heat island effect), outdoor workers and people who take certain prescription drugs.
Climate change increases the frequency and severity of heatwaves and thus heat stress for people. Human responses to heat stress can include heat stroke and overheating (hyperthermia). Extreme heat is also linked to acute kidney injury, low quality sleep, and complications with pregnancy.Furthermore, it may cause the deterioration of pre-existing cardiovascular and respiratory disease. Adverse pregnancy outcomes due to high ambient temperatures include for example low birth weight and pre-term birth.Heat waves have also resulted in epidemics of chronic kidney disease (CKD). Prolonged heat exposure, physical exertion, and dehydration are sufficient factors for the development of CKD.
The human body requires evaporation of sweat to cool down and prevent overheating, even with a low activity level. With excessive heat and humidity human bodies would no longer be able to adequately cool the skin. A wet-bulb temperature of 35 °C is regarded as the limit for humans (called the "physiological threshold for human adaptability" to heat and humidity). As of 2020, only two weather stations had recorded 35 °C wet-bulb temperatures, and only very briefly, but the frequency and duration of these events is expected to rise with ongoing climate change. Global warming above 1.5 degrees risks making parts of the tropics uninhabitable because the threshold for the wet bulb temperature may be passed. A wet-bulb temperature of 31 degrees is already considered dangerous, even for young and healthy people. This threshold is not uniform for all and depend on many factors including environmental factors, activity and age. If the global temperature will rise by 3 degrees (the most likely scenario without reducing the use of fossil fuels), temperatures will exceed this limit at large areas in Pakistan, India, China, sub-Saharan Africa, United States, Australia, and South America.
People with cognitive health issues (e.g. depression, dementia, Parkinson's disease) are more at risk when faced with high temperatures and ought to be extra careful as cognitive performance has been shown to be differentially affected by heat. People with diabetes and those who are overweight, have sleep deprivation, or have cardiovascular/cerebrovascular conditions should avoid too much heat exposure.
The risk of dying from chronic lung disease during a heat wave has been estimated at 1.8–8.2% higher compared to average summer temperatures. An 8% increase in hospitalization rate for people with chronic obstructive pulmonary disease (COPD) has been estimated for every 1 °C increase in temperatures above 29 °C.
In urban areas
Further information: Urban heat island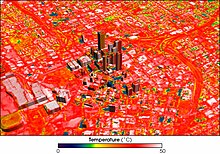
The effects of heatwaves tend to be more pronounced in urban areas because they are typically warmer than surrounding rural areas due to the urban heat island effect. This results from the way many cities are built. For example, they often have extensive areas of asphalt, reduced greenery along with many large heat-retaining buildings that physically block cooling breezes and ventilation. Lack of water features are another cause.
Extreme heat exposure in cities with a wet bulb globe temperature above 30 °C tripled between 1983 and 2016. It increased by about 50% when the population growth in these cities is not taken into account.
Cities are often on the front-line of climate change due to their densely concentrated populations, the urban heat island effect, their frequent proximity to coasts and waterways, and reliance on ageing physical infrastructure networks.
Heat-related mortality
Health experts warn that "exposure to extreme heat increases the risk of death from cardiovascular, cerebrovascular, and respiratory conditions and all-cause mortality. Heat-related deaths in people older than 65 years reached a record high of an estimated 345 000 deaths in 2019". More than 70,000 Europeans died as a result of the 2003 European heat wave. Also more than 2,000 people died in Karachi, Pakistan in June 2015 due to a severe heat wave with temperatures as high as 49 °C (120 °F).
Due to climate change temperatures rose in Europe and heat mortality increased. From 2003–12 to 2013–22 alone, it increased by 17 deaths per 100,000 people, while women are more vulnerable than men.
Increasing access to indoor cooling (air conditioning) will help prevent heat-related mortality but current air conditioning technology is generally unsustainable as it contributes to greenhouse gas emissions, air pollution, peak electricity demand, and urban heat islands.
Mortality due to heat waves could be reduced if buildings were better designed to modify the internal climate, or if the occupants were better educated about the issues, so they can take action on time. Heatwave early warning and response systems are important elements of heat action plans.
Reduced labour capacity
Heat exposure can affect people's ability to work. The annual Countdown Report by The Lancet investigated change in labour capacity as an indicator. It found that during 2021, high temperature reduced global potential labour hours by 470 billion – a 37% increase compared to the average annual loss that occurred during the 1990s. Occupational heat exposure especially affects laborers in the agricultural sector of developing countries. In those countries, the vast majority of these labour hour losses (87%) were in the agricultural sector.
Working in extreme heat can lead to labor force productivity decreases as well as participation because employees' health may be weaker due to heat related health problems, such as dehydration, fatigue, dizziness, and confusion.
Sports and outdoor exercise
With regards to sporting activities, it has been observed that "hot weather reduces the likelihood of engaging in exercise". Furthermore, participating in sports during excessive heat can lead to injury or even death. It is also well established that regular physical activity is beneficial for human health, including mental health. Therefore, an increase in hot days due to climate change could indirectly affect health due to people exercising less.
Droughts
Further information: Drought § Social and health impactsClimate change affects multiple factors associated with droughts, such as how much rain falls and how fast the rain evaporates again. Warming over land increases the severity and frequency of droughts around much of the world. Many of the consequences of droughts have effects on human health.
Floods
Further information: Flood § Health impactsDue to an increase in heavy rainfall events, floods are expected to become more severe in the future when they do occur. However, the interactions between rainfall and flooding are complex. In some regions, flooding is expected to become rarer. This depends on several factors, such as changes in rain and snowmelt, but also soil moisture. Floods have short and long-term negative implications to people's health and well-being. Short term implications include mortalities, injuries and diseases, while long term implications include non-communicable diseases and psychosocial health aspects. For example, the 2022 Pakistan floods (which were likely more severe because of climate change) affected people's health directly and indirectly. There were outbreaks of diseases like malaria, dengue, and other skin diseases.

Wildfires
Further information: Wildfire § Health effectsClimate change increases wildfire potential and activity. Climate change leads to a warmer ground temperature and its effects include earlier snowmelt dates, drier than expected vegetation, increased number of potential fire days, increased occurrence of summer droughts, and a prolonged dry season. Wood smoke from wildfires produces particulate matter that has damaging effects to human health. The health effects of wildfire smoke exposure include exacerbation and development of respiratory illness such as asthma and chronic obstructive pulmonary disorder; increased risk of lung cancer, mesothelioma and tuberculosis; increased airway hyper-responsiveness; changes in levels of inflammatory mediators and coagulation factors; and respiratory tract infection.
Storms
Further information: Effects of climate change § Extreme storms, and Tropical cyclones and climate changeStorms become wetter under climate change. These include tropical cyclones and extratropical cyclones. Both the maximum and mean rainfall rates increase. This more extreme rainfall is also true for thunderstorms in some regions. Furthermore, tropical cyclones and storm tracks are moving towards the poles. This means some regions will see large changes in maximum wind speeds. Scientists expect there will be fewer tropical cyclones. But they expect their strength to increase.
Health risks from climate-sensitive infectious diseases
This section is an excerpt from Climate change and infectious diseases.

Global climate change has increased the occurrence of some infectious diseases. Infectious diseases whose transmission is impacted by climate change include, for example, vector-borne diseases like dengue fever, malaria, tick-borne diseases, leishmaniasis, zika fever, chikungunya and Ebola. One mechanism contributing to increased disease transmission is that climate change is altering the geographic range and seasonality of the insects (or disease vectors) that can carry the diseases. Scientists stated a clear observation in 2022: "The occurrence of climate-related food-borne and waterborne diseases has increased (very high confidence)."
Infectious diseases that are sensitive to climate can be grouped into: vector-borne diseases (transmitted via mosquitos, ticks etc.), waterborne diseases (transmitted via viruses or bacteria through water), and food-borne diseases.(spread through pathogens via food) Climate change affects the distribution of these diseases due to the expanding geographic range and seasonality of these diseases and their vectors. Like other ways climate change affects human health, climate change exacerbates existing inequalities and challenges in managing infectious disease.
Mosquito-borne diseases that are sensitive to climate include malaria, lymphatic filariasis, Rift Valley fever, yellow fever, dengue fever, Zika virus, and chikungunya. Scientists found in 2022 that rising temperatures are increasing the areas where dengue fever, malaria and other mosquito-carried diseases are able to spread. Warmer temperatures are also advancing to higher elevations, allowing mosquitoes to survive in places that were previously in hospitable to them. This risks malaria returning to areas where it was previously eradicated.Health risks from changes in air quality
Indoor air quality
Indoor air pollution is known to affect the health, comfort, and well-being of building occupants. It has also been linked to sick building syndrome, respiratory issues, reduced productivity, and impaired learning in schools. Indoor air quality is linked inextricably to outdoor air quality. Climate change can affect indoor air quality by increasing the level of outdoor air pollutants such as ozone and particulate matter, for example through emissions from wildfires caused by extreme heat and drought. There are numerous predictions for how indoor air pollutants will change in future. Models have attempted to predict how the forecasted scenarios will affect indoor air quality and indoor comfort parameters such as humidity and temperature.
The net-zero challenge requires significant changes in the performance of both new and retrofitted buildings. Increased energy efficient housing (without good ventilation systems) can trap pollutants inside them, whether produced indoors or outdoors, and lead to an increase in human exposure.
Ozone-related health burden
Further information: Ozone § Ozone air pollution, Ozone § Low level ozone in urban areas, and Ground-level ozone § Ozone and the climate
The relationship between surface ozone (also called ground-level ozone) and ambient temperature is complex. Changes in air temperature and water content affect the air's chemistry and the rates of chemical reactions that create and remove ozone. Many chemical reaction rates increase with temperature and lead to increased ozone production. Climate change projections show that rising temperatures and water vapour in the atmosphere will likely increase surface ozone in polluted areas like the eastern United States.
On the other hand, ozone concentrations could decrease in a warming climate if anthropogenic ozone-precursor emissions (e.g., nitrogen oxides) continue to decrease through implementation of policies and practices. Therefore, future surface ozone concentrations depend on the climate change mitigation steps taken (more or less methane emissions) as well as air pollution control steps taken.
High surface ozone concentrations often occur during heat waves in the United States. Throughout much of the eastern United States, ozone concentrations during heat waves are at least 20% higher than the summer average. Broadly speaking, surface ozone levels are higher in cities with high levels of air pollution. Ozone pollution in urban areas affects denser populations, and is worsened by high populations of vehicles, which emit pollutants NO2 and VOCs, the main contributors to problematic ozone levels.
There is a great deal of evidence to show that surface ozone can harm lung function and irritate the respiratory system. Exposure to ozone (and the pollutants that produce it) is linked to premature death, asthma, bronchitis, heart attack, and other cardiopulmonary problems. High ozone concentrations irritate the lungs and thus affect respiratory function, especially among people with asthma. People who are most at risk from breathing in ozone air pollution are those with respiratory issues, children, older adults and those who typically spend long periods of time outside such as construction workers.
Other health risks
Health risks from food and water insecurity
Further information: Effects of climate change on agriculture, Water security § Climate change, and Effects of climate change on livestockClimate change affects many aspects of food security through "multiple and interconnected pathways". Many of these are related to the effects of climate change on agriculture, for example failed crops due to more extreme weather events. This comes on top of other coexisting crises that reduce food security in many regions. Less food security means more undernutrition with all its associated health problems. Food insecurity is increasing at the global level (some of the underlying causes are related to climate change, others are not) and about 720–811 million people suffered from hunger in 2020.
The number of deaths resulting from climate change-induced changes to food availability are difficult to estimate. The 2022 IPCC Sixth Assessment Report does not quantify this number in its chapter on food security. A modelling study from 2016 found "a climate change–associated net increase of 529,000 adult deaths worldwide from expected reductions in food availability (particularly fruit and vegetables) by 2050, as compared with a reference scenario without climate change."
A headline finding in 2021 regarding marine food security stated that: "In 2018–20, nearly 70% of countries showed increases in average sea surface temperature in their territorial waters compared within 2003–05, reflecting an increasing threat to their marine food productivity and marine food security". (see also climate change and fisheries).
Mental health risks
This section is an excerpt from Effects of climate change on mental health.

Pollen allergies
A warming climate can lead to increases of pollen season lengths and concentrations in some regions of the world. For example, in northern mid-latitudes regions, the spring pollen season is now starting earlier. This can affect people with pollen allergies (hay fever). The rise in pollen also comes from rising CO2 concentrations in the atmosphere and resulting CO2 fertilisation effects.
Reduced nutritional value of crops
This section is an excerpt from Effects of climate change on agriculture § Reduced nutritional value of crops.
Harmful algal blooms in oceans and lakes
See also: Harmful algal bloom
The warming oceans and lakes are leading to more frequent harmful algal blooms. Also, during droughts, surface waters are even more susceptible to harmful algal blooms and microorganisms. Algal blooms increase water turbidity, suffocating aquatic plants, and can deplete oxygen, killing fish. Some kinds of blue-green algae (cyanobacteria) create neurotoxins, hepatoxins, cytotoxins or endotoxins that can cause serious and sometimes fatal neurological, liver and digestive diseases in humans. Cyanobacteria grow best in warmer temperatures (especially above 25 degrees Celsius), and so areas of the world that are experiencing general warming as a result of climate change are also experiencing harmful algal blooms more frequently and for longer periods of time.
One of these toxin producing algae is Pseudo-nitzschia fraudulenta. This species produces a substance called domoic acid which is responsible for amnesic shellfish poisoning. The toxicity of this species has been shown to increase with greater CO2 concentrations associated with ocean acidification. Some of the more common illnesses reported from harmful algal blooms include; Ciguatera fish poisoning, paralytic shellfish poisoning, azaspiracid shellfish poisoning, diarrhetic shellfish poisoning, neurotoxic shellfish poisoning and the above-mentioned amnesic shellfish poisoning.
Potential health benefits
It is possible that a potential health benefit from global warming could result from fewer cold days in winter: This could lead to some mental health benefits. However, the evidence on this correlation is regarded as inconsistent in 2022.
Benefits from climate change mitigation and adaptation
See also: Climate change mitigation § Co-benefitsThe potential health benefits (also called "co-benefits") from climate change mitigation and adaptation measures are significant, having been described as "the greatest global health opportunity" of the 21st century. Measures can not only mitigate future health effects from climate change but also improve health directly. Climate change mitigation is interconnected with various co-benefits (such as reduced air pollution and associated health benefits) and how it is carried out (in terms of e.g. policymaking) could also determine its effect on living standards (whether and how inequality and poverty are reduced).
There are many health co-benefits associated with climate action. These include those of cleaner air, healthier diets (e.g. less red meat), more active lifestyles, and increased exposure to green urban spaces. Access to urban green spaces provides benefits to mental health as well.
In the transportation sector mitigation strategies could enable more equitable access to transportation services and reduce congestion. Biking reduces greenhouse gas emissions while reducing the effects of a sedentary lifestyle at the same time According to PLoS Medicine: "obesity, diabetes, heart disease, and cancer, which are in part related to physical inactivity, may be reduced by a switch to low-carbon transport—including walking and cycling."
Future sustainable pathways scenarios may result in an annual reduction of 1.18 million air pollution-related deaths, 5.86 million diet-related deaths, and 1.15 million deaths due to physical inactivity, across nine countries by 2040. These benefits were attributable to the mitigation of direct greenhouse gas emissions and the accompanying actions that reduce exposure to harmful pollutants, as well as improved diets and safe physical activity. Globally the cost of limiting warming to 2 °C is less than the value of the extra years of life due to cleaner air - and in India and China much less.
Studies suggest that efforts to reduce consumption of goods and services have largely beneficial effects on 18 constituents of well-being.
Addressing inequality can assist with climate change mitigation efforts. Placing health as a key focus of the Nationally Determined Contributions could present an opportunity to increase ambition and realise health co-benefits.
Air pollution reduction
Air pollution generated by fossil fuel combustion is both a major driver of global warming and the cause of a large number of annual deaths with some estimates as high as 8.7 million excess deaths during 2018. Climate change mitigation policies can lead to lower emissions of co-emitted air pollutants, for instance by shifting away from fossil fuel combustion. Gases such as black carbon and methane contribute both to global warming and to air pollution. Their mitigation can bring benefits in terms of limiting global temperature increases as well as improving air quality. Implementation of the climate pledges made in the run-up to the Paris Agreement could therefore have significant benefits for human health by improving air quality.
The replacement of coal-based energy with renewables can lower the number of premature deaths caused by air pollution and decrease health costs associated with coal-related respiratory diseases. This switch to renewable energy is crucial, as air pollution is responsible for over 13 million deaths annually.
Global estimates

Estimating deaths (mortality) or DALYs (morbidity) from the effects of climate change at the global level is very difficult. A 2014 study by the World Health Organization estimated the effect of climate change on human health, but not all of the effects of climate change were included. For example, the effects of more frequent and extreme storms were excluded. The study assessed deaths from heat exposure in elderly people, increases in diarrhea, malaria, dengue, coastal flooding, and childhood undernutrition. The authors estimated that climate change was projected to cause an additional 250,000 deaths per year between 2030 and 2050 but also stated that "these numbers do not represent a prediction of the overall impacts of climate change on health, since we could not quantify several important causal pathways".
Climate change was responsible for 3% of diarrhoea, 3% of malaria, and 3.8% of dengue fever deaths worldwide in 2004. Total attributable mortality was about 0.2% of deaths in 2004; of these, 85% were child deaths. The effects of more frequent and extreme storms were excluded from this study.
The health effects of climate change are expected to rise in line with projected ongoing global warming for different climate change scenarios. A review found if warming reaches or exceeds 2 °C this century, roughly 1 billion premature deaths would be caused by anthropogenic global warming.
Society and culture
Vulnerability
Further information: Climate change vulnerabilityA 2021 report published in The Lancet found that climate change does not affect people's health in an equal way. The greatest impact tends to fall on the most vulnerable such as the poor, women, children, the elderly, people with pre-existing health concerns, other minorities and outdoor workers.
Social factors shape health outcomes as people are rendered more or less able to adapt to harms. For example there are "demographic, socioeconomic, housing, health (such as pre-existing health conditions), neighbourhood, and geographical factors" that moderate the effect of climate change on human health.
Climate justice and climate migrants
Further information: Climate justice and Climate migrantMuch of the health burden associated with climate change falls on vulnerable people (e.g. indigenous peoples and economically disadvantaged communities). As a result, people of disadvantaged sociodemographic groups experience unequal risks. Often these people will have made a disproportionately low contribution toward man-made global warming, thus leading to concerns over climate justice.
Climate change has diverse effects on migration activities, and can lead to decreases or increases in the number of people who migrate. Migration activities can have an effect on health and well-being, in particular for mental health. Migration in the context of climate change can be grouped into four types: adaptive migration (see also climate change adaptation), involuntary migration, organised relocation of populations, and immobility (which is when people are unable or unwilling to move even though it is recommended).
The observed contribution of climate change to conflict risk is small in comparison with cultural, socioeconomic, and political causes. There is some evidence that rural-to-urban migration within countries worsens the conflict risk in violence prone regions. But there is no evidence that migration between countries would increase the risk of violence.
Communication strategies
Further information: Individual action on climate changeStudies have found that when communicating climate change with the public, it can help encourage engagement if it is framed as a health concern, rather than as an environmental issue. This is especially the case when comparing a health related framing to one that emphasised environmental doom, as was common in the media at least up until 2017. Communicating the co-benefits to health helps underpin greenhouse gas reduction strategies. Safeguarding health—particularly of the most vulnerable—is a frontline local climate change adaptation goal.
Connections with public health policies
Due to its significant impact on human health, climate change has become a major concern for public health policy. The United States Environmental Protection Agency had issued a 100-page report on global warming and human health back in 1989. By the early years of the 21st century, climate change was increasingly addressed as a public health concern at a global level, for example in 2006 at Nairobi by UN secretary general Kofi Annan. Since 2018, factors such as the 2018 heat wave, the Greta effect and the IPCC's 2018 Special Report on Global Warming of 1.5 °C further increased the urgency for responding to climate change as a global health issue.
The World Bank has suggested a framework that can strengthen health systems to make them more resilient and climate-sensitive.
Placing health as a key focus of the Nationally Determined Contributions could present an opportunity to increase ambition and realize health co-benefits.
In 2019, the Australian Medical Association formally declared climate change as a health emergency.
Research shows that health professionals around the world agree that climate change is real, is caused by humans, and is causing increased health problems in their communities. Health professionals can act by informing people about health harms and ways to address them, by lobbying leaders to take action, and by taking steps to decarbonize their own homes and workplaces.
See also
- Effects of climate change
- Health policy
- Health system
- Environmental health
- Occupational heat stress
- Water security
References
- Atwoli, Lukoye; Baqui, Abdullah H; Benfield, Thomas; Bosurgi, Raffaella; Godlee, Fiona; Hancocks, Stephen; Horton, Richard; Laybourn-Langton, Laurie; Monteiro, Carlos Augusto; Norman, Ian; Patrick, Kirsten; Praities, Nigel; Olde Rikkert, Marcel G M; Rubin, Eric J; Sahni, Peush (2021-09-04). "Call for emergency action to limit global temperature increases, restore biodiversity, and protect health". The Lancet. 398 (10304): 939–941. doi:10.1016/S0140-6736(21)01915-2. PMC 8428481. PMID 34496267.
- "WHO calls for urgent action to protect health from climate change – Sign the call". World Health Organization. 2015. Archived from the original on October 8, 2015. Retrieved 2020-04-19.
- ^ Romanello, Marina; McGushin, Alice; Di Napoli, Claudia; Drummond, Paul; Hughes, Nick; Jamart, Louis; et al. (October 2021). "The 2021 report of the Lancet Countdown on health and climate change: code red for a healthy future" (PDF). The Lancet. 398 (10311): 1619–1662. doi:10.1016/S0140-6736(21)01787-6. hdl:10278/3746207. PMC 7616807. PMID 34687662. S2CID 239046862.
- Baker, Rachel E.; Mahmud, Ayesha S.; Miller, Ian F.; Rajeev, Malavika; Rasambainarivo, Fidisoa; Rice, Benjamin L.; et al. (April 2022). "Infectious disease in an era of global change". Nature Reviews Microbiology. 20 (4): 193–205. doi:10.1038/s41579-021-00639-z. ISSN 1740-1534. PMC 8513385. PMID 34646006.
- Wilson, Mary E. (2010). "Geography of infectious diseases". Infectious Diseases: 1055–1064. doi:10.1016/B978-0-323-04579-7.00101-5. ISBN 978-0-323-04579-7. PMC 7152081.
- Levy, Karen; Smith, Shanon M.; Carlton, Elizabeth J. (2018). "Climate Change Impacts on Waterborne Diseases: Moving Toward Designing Interventions". Current Environmental Health Reports. 5 (2): 272–282. Bibcode:2018CEHR....5..272L. doi:10.1007/s40572-018-0199-7. ISSN 2196-5412. PMC 6119235. PMID 29721700.
- Watts, Nick; Amann, Markus; Arnell, Nigel; Ayeb-Karlsson, Sonja; Belesova, Kristine; Boykoff, Maxwell; et al. (16 November 2019). "The 2019 report of The Lancet Countdown on health and climate change: ensuring that the health of a child born today is not defined by a changing climate" (PDF). The Lancet. 394 (10211): 1836–1878. Bibcode:2019Lanc..394.1836W. doi:10.1016/S0140-6736(19)32596-6. PMC 7616843. PMID 31733928. S2CID 207976337.
- Romanello, Marina; McGushin, Alice; Di Napoli, Claudia; Drummond, Paul; Hughes, Nick; Jamart, Louis; et al. (October 2021). "The 2021 report of the Lancet Countdown on health and climate change: code red for a healthy future" (PDF). The Lancet. 398 (10311): 1619–1662. doi:10.1016/S0140-6736(21)01787-6. hdl:10278/3746207. PMC 7616807. PMID 34687662. S2CID 239046862.
- ^ Watts, Nick; Adger, W Neil; Agnolucci, Paolo; Blackstock, Jason; Byass, Peter; Cai, Wenjia; et al. (2015). "Health and climate change: policy responses to protect public health". The Lancet. 386 (10006): 1861–1914. doi:10.1016/S0140-6736(15)60854-6. hdl:10871/17695. PMID 26111439. S2CID 205979317.
- Myers, Samuel S.; Bernstein, Aaron (2011-02-01). "The coming health crisis: indirect health effects of global climate change". F1000 Biology Reports. 3: 3. doi:10.3410/B3-3. PMC 3042309. PMID 21399764.
- Di Napoli, Claudia; McGushin, Alice; Romanello, Marina; Ayeb-Karlsson, Sonja; Cai, Wenjia; Chambers, Jonathan; Dasgupta, Shouro; Escobar, Luis E.; Kelman, Ilan; Kjellstrom, Tord; Kniveton, Dominic; Liu, Yang; Liu, Zhao; Lowe, Rachel; Martinez-Urtaza, Jaime (2022-04-06). "Tracking the impacts of climate change on human health via indicators: lessons from the Lancet Countdown". BMC Public Health. 22 (1): 663. doi:10.1186/s12889-022-13055-6. ISSN 1471-2458. PMC 8985369. PMID 35387618.
- "Operational framework for building climate resilient health systems". www.who.int. 2015. Retrieved 2022-04-13.
- Seneviratne, Sonia I.; Zhang, Xuebin; Adnan, M.; Badi, W.; et al. (2021). "Chapter 11: Weather and climate extreme events in a changing climate" (PDF). Climate Change 2021: The Physical Science Basis. Contribution of Working Group I to the Sixth Assessment Report of the Intergovernmental Panel on Climate. Cambridge University Press. p. 1517.
- Attribution of Extreme Weather Events in the Context of Climate Change (Report). Washington, DC: The National Academies Press. 2016. pp. 127–136. doi:10.17226/21852. ISBN 978-0-309-38094-2. Archived from the original on 2022-02-15. Retrieved 2020-02-22.
- IPCC (2021). "Summary for Policymakers" (PDF). The Physical Science Basis. Contribution of Working Group I to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change. p. 40. ISBN 978-92-9169-158-6.
- Lenton, Timothy M.; Xu, Chi; Abrams, Jesse F.; Ghadiali, Ashish; Loriani, Sina; Sakschewski, Boris; et al. (2023-05-22). "Quantifying the human cost of global warming". Nature Sustainability. 6 (10): 1237–1247. Bibcode:2023NatSu...6.1237L. doi:10.1038/s41893-023-01132-6. hdl:10871/132650. ISSN 2398-9629. S2CID 249613346.
- "Climate change: More than 3bn could live in extreme heat by 2070". BBC News. 5 May 2020. Archived from the original on 5 May 2020. Retrieved 6 May 2020.
- Xu, Chi; Kohler, Timothy A.; Lenton, Timothy M.; Svenning, Jens-Christian; Scheffer, Marten (26 May 2020). "Future of the human climate niche – Supplementary Materials". Proceedings of the National Academy of Sciences. 117 (21): 11350–11355. Bibcode:2020PNAS..11711350X. doi:10.1073/pnas.1910114117. PMC 7260949. PMID 32366654.
- Kemp, Luke; Xu, Chi; Depledge, Joanna; Ebi, Kristie L.; Gibbins, Goodwin; Kohler, Timothy A.; et al. (23 August 2022). "Climate Endgame: Exploring catastrophic climate change scenarios". Proceedings of the National Academy of Sciences. 119 (34): e2108146119. Bibcode:2022PNAS..11908146K. doi:10.1073/pnas.2108146119. ISSN 0027-8424. PMC 9407216. PMID 35914185.
- ^ Demain, Jeffrey G. (24 March 2018). "Climate Change and the Impact on Respiratory and Allergic Disease: 2018". Current Allergy and Asthma Reports. 18 (4): 22. doi:10.1007/s11882-018-0777-7. PMID 29574605. S2CID 4440737.
- Hajat, Shakoor; Casula, Anna; Murage, Peninah; Omoyeni, Daniel; Gray, Tom; Plummer, Zoe; Steenkamp, Retha; Nitsch, Dorothea (1 March 2024). "Ambient heat and acute kidney injury: case-crossover analysis of 1 354 675 automated e-alert episodes linked to high-resolution climate data". The Lancet Planetary Health. 8 (3): e156–e162. doi:10.1016/s2542-5196(24)00008-1. ISSN 2542-5196. PMID 38453381.
- "Hot weather increases the risk of acute kidney injury". NIHR Evidence. 13 August 2024. doi:10.3310/nihrevidence_63987.
- ^ Romanello, Marina; Di Napoli, Claudia; Drummond, Paul; Green, Carole; Kennard, Harry; Lampard, Pete; et al. (November 5, 2022). "The 2022 report of the Lancet Countdown on health and climate change: health at the mercy of fossil fuels". The Lancet. 400 (10363): 1619–1654. doi:10.1016/S0140-6736(22)01540-9. PMC 7616806. PMID 36306815.
- ^ Glaser; et al. (2016). "Climate Change and the Emergent Epidemic of CKD from Heat Stress in Rural Communities: the Case for Heat Stress Nephropathy". Clinical Journal of the American Society of Nephrology. 11 (8): 1472–83. doi:10.2215/CJN.13841215. PMC 4974898. PMID 27151892.
- ^ Shih, Gerry (2023-01-06). "The world's torrid future is etched in the crippled kidneys of Nepali workers". The Washington Post. Retrieved 2023-01-20.
- ^ Milman, Oliver (8 March 2021). "Global heating pushes tropical regions towards limits of human livability". The Guardian. Retrieved 24 June 2021.
- Chow, Denise (2022-05-07). "Deadly 'wet-bulb temperatures' are being stoked by climate change and heat waves". NBC News. Retrieved 2022-07-22.
- Shaw, R.; Luo, Y.; Cheong, T. S.; Halim, S. Abdul; Chaturvedi, S.; Hashizume, M.; et al. (2022). "Asia" (PDF). In Pörtner, H.-O.; Roberts, D. C.; Tignor, M.; Poloczanska, E. S.; Mintenbeck, K.; Alegría, A.; et al. (eds.). Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change. Cambridge and New York: Cambridge University Press. pp. 1457–1579. doi:10.1017/9781009325844.012. ISBN 978-1-009-32584-4.
- Sherwood, S. C.; Huber, M. (25 May 2010). "An adaptability limit to climate change due to heat stress". Proceedings of the National Academy of Sciences of the USA. 107 (21): 9552–5. Bibcode:2010PNAS..107.9552S. doi:10.1073/pnas.0913352107. PMC 2906879. PMID 20439769.
- Madge, Grahame (2021-11-09). "One billion face heat-stress risk from 2°C rise". Met Office. Retrieved 2021-11-10.
- Raymond, Colin; Matthews, Tom; Horton, Radley M. (2020). "The emergence of heat and humidity too severe for human tolerance". Science Advances. 6 (19): eaaw1838. Bibcode:2020SciA....6.1838R. doi:10.1126/sciadv.aaw1838. PMC 7209987. PMID 32494693.
- "Climate driven extreme heat threatens human habitation on earth". Open Access Government. Penn State College of Health and Human Development, Purdue University College of Sciences, Purdue Institute for a Sustainable Future. 16 October 2023. Retrieved 22 October 2023.
- ^ Kovats, R. Sari; Hajat, Shakoor (April 2008). "Heat Stress and Public Health: A Critical Review". Annual Review of Public Health. 29 (1): 41–55. doi:10.1146/annurev.publhealth.29.020907.090843. PMID 18031221.
- Hancock, P. A.; Vasmatzidis, I. (2003). "Effects of heat stress on cognitive performance: the current state of knowledge". International Journal of Hyperthermia. 19 (3): 355–372. CiteSeerX 10.1.1.464.7830. doi:10.1080/0265673021000054630. PMID 12745975. S2CID 13960829.
- Koppe, Christina; Kovats, Sari; Jendritzky, Gerd; Menne, Bettina (2004). "Heat-waves: risks and responses". Health and Global Environmental Change Series. 2. Archived from the original on 2023-03-22. Retrieved 2023-03-16.
- Witt, Christian; Schubert, André Jean; Jehn, Melissa; Holzgreve, Alfred; Liebers, Uta; Endlicher, Wilfried; Scherer, Dieter (2015-12-21). "The Effects of Climate Change on Patients With Chronic Lung Disease. A Systematic Literature Review". Deutsches Ärzteblatt International. 112 (51–52): 878–883. doi:10.3238/arztebl.2015.0878. ISSN 1866-0452. PMC 4736555. PMID 26900154.
- ^ Tuholske, Cascade; Caylor, Kelly; Funk, Chris; Verdin, Andrew; Sweeney, Stuart; Grace, Kathryn; Peterson, Pete; Evans, Tom (2021-10-12). "Global urban population exposure to extreme heat". Proceedings of the National Academy of Sciences of the United States of America. 118 (41): e2024792118. Bibcode:2021PNAS..11824792T. doi:10.1073/pnas.2024792118. ISSN 1091-6490. PMC 8521713. PMID 34607944.
- ^ Möller, V.; van Diemen, R.; Matthews, J. B. R.; Méndez, C.; Semenov, S.; Fuglestvedt, J. S.; Reisinger, A. (2022). "Annex II: Glossary" (PDF). In Pörtner, H.-O.; Roberts, D. C.; Tignor, M.; Poloczanska, E. S.; Mintenbeck, K.; Alegría, A.; et al. (eds.). Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change. Cambridge and New York: Cambridge University Press. pp. 2897–2930. doi:10.1017/9781009325844.029.
- ^ Fox, M.; Zuidema, C.; Bauman, B.; Burke, T.; Sheehan, M. (2019). "Integrating Public Health into Climate Change Policy and Planning: State of Practice Update". International Journal of Environmental Research and Public Health. 16 (18): 3232. doi:10.3390/ijerph16183232. PMC 6765852. PMID 31487789.
 Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License
Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License
- Robine, Jean-Marie; Cheung, Siu Lan K; Le Roy, Sophie; Van Oyen, Herman; Griffiths, Clare; Michel, Jean-Pierre; Herrmann, François Richard (2008). "Death toll exceeded 70,000 in Europe during the summer of 2003". Comptes Rendus Biologies. 331 (2): 171–8. doi:10.1016/j.crvi.2007.12.001. PMID 18241810.
- Haider, Kamran; Anis, Khurrum (24 June 2015). "Heat Wave Death Toll Rises to 2,000 in Pakistan's Financial Hub". Bloomberg News. Retrieved 3 August 2015.
- Mansoor, Hasan (30 June 2015). "Heatstroke leaves another 26 dead in Sindh". Dawn. Retrieved 9 August 2015.
- Wong, Carissa (2024). "How climate change is hitting Europe: three graphics reveal health impacts". Nature. 630 (8018). Lancet Public Health: 800–801. Bibcode:2024Natur.630..800W. doi:10.1038/d41586-024-02006-3. PMID 38890517. Retrieved 27 June 2024.
- Coley, D.; Kershaw, T. J.; Eames, M. (2012). "A comparison of structural and behavioural adaptations to future proofing buildings against higher temperatures" (PDF). Building and Environment. 55: 159–166. Bibcode:2012BuEnv..55..159C. doi:10.1016/j.buildenv.2011.12.011. hdl:10871/13936. S2CID 55303235.
- Coley, D.; Kershaw, T. J. (2010). "Changes in internal temperatures within the built environment as a response to a changing climate" (PDF). Building and Environment. 45 (1): 89–93. Bibcode:2010BuEnv..45...89C. doi:10.1016/j.buildenv.2009.05.009.
- Liu, Xingcai (February 2020). "Reductions in Labor Capacity from Intensified Heat Stress in China under Future Climate Change". International Journal of Environmental Research and Public Health. 17 (4): 1278. doi:10.3390/ijerph17041278. PMC 7068449. PMID 32079330.
- ^ Cissé, G.; McLeman, R.; Adams, H.; Aldunce, P.; Bowen, K.; Campbell-Lendrum, D.; et al. (2022). "Chapter 7: Health, Wellbeing, and the Changing Structure of Communities" (PDF). In Pörtner, H.-O.; Roberts, D. C.; Tignor, M.; Poloczanska, E. S.; Mintenbeck, K.; Alegría, A.; et al. (eds.). Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change (Report). Cambridge and New York: Cambridge University Press. pp. 1041–1170. doi:10.1017/9781009325844.009.
- Cook, Benjamin I.; Mankin, Justin S.; Anchukaitis, Kevin J. (2018-05-12). "Climate Change and Drought: From Past to Future". Current Climate Change Reports. 4 (2): 164–179. Bibcode:2018CCCR....4..164C. doi:10.1007/s40641-018-0093-2. ISSN 2198-6061. S2CID 53624756.
- ^ Douville, H., K. Raghavan, J. Renwick, R.P. Allan, P.A. Arias, M. Barlow, R. Cerezo-Mota, A. Cherchi, T.Y. Gan, J. Gergis, D. Jiang, A. Khan, W. Pokam Mba, D. Rosenfeld, J. Tierney, and O. Zolina, 2021: Chapter 8: Water Cycle Changes. In Climate Change 2021: The Physical Science Basis. Contribution of Working Group I to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change . Cambridge University Press, Cambridge, United Kingdom and New York, NY, USA, pp. 1055–1210, doi:10.1017/9781009157896.010.
- Alderman, Katarzyna; Turner, Lyle R.; Tong, Shilu (June 2012). "Floods and human health: A systematic review" (PDF). Environment International. 47: 37–47. Bibcode:2012EnInt..47...37A. doi:10.1016/j.envint.2012.06.003. PMID 22750033.
- Zhong, Raymond (15 September 2022). "In a First Study of Pakistan's Floods, Scientists See Climate Change at Work". The New York Times.
- "Climate Change Likely Worsened Pakistan's Devastating Floods". Scientific American.
- "Public health risks increasing in flood-affected Pakistan, warns WHO". November 2022.
- "UN Warns Deadly Diseases Spreading Fast in Flood-Ravaged Pakistan". 3 October 2022.
- Liu, Y.; Stanturf, J.; Goodrick, S. (February 2010). "Trends in global wildfire potential in a changing climate". Forest Ecology and Management. 259 (4): 685–697. Bibcode:2010ForEM.259..685L. doi:10.1016/j.foreco.2009.09.002.
- Westerling, A.; Hidalgo, H.; Cayan, D.; Swetnam, T. (August 2006). "Warming and earlier spring increase Western U.S. Forest Wildfire Activity". Science. 313 (5789): 940–943. Bibcode:2006Sci...313..940W. doi:10.1126/science.1128834. PMID 16825536.
- ^ Naeher, Luke P.; Brauer, Mmichael; Lipsett, Michael; et al. (January 2007). "Woodsmoke health effects: A review". Inhalation Toxicology. 19 (1): 67–106. Bibcode:2007InhTx..19...67N. CiteSeerX 10.1.1.511.1424. doi:10.1080/08958370600985875. PMID 17127644. S2CID 7394043.
- ^ Seneviratne, Sonia I.; Zhang, Xuebin; Adnan, M.; et al. (2021). "Chapter 11: Weather and climate extreme events in a changing climate" (PDF). Climate Change 2021: The Physical Science Basis. Contribution of Working Group I to the Sixth Assessment Report of the Intergovernmental Panel on Climate. Cambridge University Press. p. 1519.
- ^ Knutson, Thomas; Camargo, Suzana J.; Chan, Johnny C. L.; Emanuel, Kerry; Ho, Chang-Hoi; Kossin, James; Mohapatra, Mrutyunjay; Satoh, Masaki; Sugi, Masato; Walsh, Kevin; Wu, Liguang (August 6, 2019). "Tropical Cyclones and Climate Change Assessment: Part II. Projected Response to Anthropogenic Warming". Bulletin of the American Meteorological Society. 101 (3): BAMS–D–18–0194.1. Bibcode:2020BAMS..101E.303K. doi:10.1175/BAMS-D-18-0194.1. hdl:1721.1/124705.
- Van de Vuurst, Paige; Escobar, Luis E. (2023). "Climate change and infectious disease: a review of evidence and research trends". Infectious Diseases of Poverty. 12 (1): 51. doi:10.1186/s40249-023-01102-2. hdl:10919/115131. PMC 10186327. PMID 37194092.
- Silburn, Alan; Arndell, Joel (2024-12-01). "The impact of dengue viruses: Surveillance, response, and public health implications in Queensland, Australia". Public Health in Practice. 8: 100529. doi:10.1016/j.puhip.2024.100529. ISSN 2666-5352. PMC 11282963. PMID 39071864.
- IPCC, 2022: Summary for Policymakers . In: Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change . Cambridge University Press, Cambridge, UK and New York, NY, USA, pp. 3–33, doi:10.1017/9781009325844.001.
- ^ Cissé, G., R. McLeman, H. Adams, P. Aldunce, K. Bowen, D. Campbell-Lendrum, S. Clayton, K.L. Ebi, J. Hess, C. Huang, Q. Liu, G. McGregor, J. Semenza, and M.C. Tirado, 2022: Chapter 7: Health, Wellbeing, and the Changing Structure of Communities. In: Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change . Cambridge University Press, Cambridge, UK and New York, NY, USA, pp. 1041–1170, doi:10.1017/9781009325844.009.
- Romanello, Marina; McGushin, Alice; Di Napoli, Claudia; Drummond, Paul; Hughes, Nick; Jamart, Louis; Kennard, Harry; Lampard, Pete; Solano Rodriguez, Baltazar; Arnell, Nigel; Ayeb-Karlsson, Sonja; Belesova, Kristine; Cai, Wenjia; Campbell-Lendrum, Diarmid; Capstick, Stuart; Chambers, Jonathan; Chu, Lingzhi; Ciampi, Luisa; Dalin, Carole; Dasandi, Niheer; Dasgupta, Shouro; Davies, Michael; Dominguez-Salas, Paula; Dubrow, Robert; Ebi, Kristie L; Eckelman, Matthew; Ekins, Paul; Escobar, Luis E; Georgeson, Lucien; Grace, Delia; Graham, Hilary; Gunther, Samuel H; Hartinger, Stella; He, Kehan; Heaviside, Clare; Hess, Jeremy; Hsu, Shih-Che; Jankin, Slava; Jimenez, Marcia P; Kelman, Ilan; et al. (October 2021). "The 2021 report of the Lancet Countdown on health and climate change: code red for a healthy future" (PDF). The Lancet. 398 (10311): 1619–1662. doi:10.1016/S0140-6736(21)01787-6. hdl:10278/3746207. PMC 7616807. PMID 34687662. S2CID 239046862.
- Reiter, Paul (2001). "Climate Change and Mosquito-Borne Disease". Environmental Health Perspectives. 109 (1): 141–161. Bibcode:2001EnvHP.109S.141R. doi:10.1289/ehp.01109s1141. PMC 1240549. PMID 11250812. Archived from the original on 24 August 2011.
- Hunter, P.R. (2003). "Climate change and waterborne and vector-borne disease". Journal of Applied Microbiology. 94: 37S–46S. doi:10.1046/j.1365-2672.94.s1.5.x. PMID 12675935. S2CID 9338260.
- McMichael, A.J.; Woodruff, R.E.; Hales, S. (11 March 2006). "Climate change and human health: present and future risks". The Lancet. 367 (9513): 859–869. doi:10.1016/s0140-6736(06)68079-3. PMID 16530580. S2CID 11220212.
- Silburn, Alan; Arndell, Joel (2024-12-01). "The impact of dengue viruses: Surveillance, response, and public health implications in Queensland, Australia". Public Health in Practice. 8: 100529. doi:10.1016/j.puhip.2024.100529. ISSN 2666-5352. PMC 11282963. PMID 39071864.
- Epstein, Paul R.; Ferber, Dan (2011). "The Mosquito's Bite". Changing Planet, Changing Health: How the Climate Crisis Threatens Our Health and what We Can Do about it. University of California Press. pp. 29–61. ISBN 978-0-520-26909-5.
- "Climate Change 2021: The Physical Science Basis". Intergovernmental Panel on Climate Change. Archived (PDF) from the original on May 26, 2023. Retrieved April 15, 2024.
- Chen, Guochao; Qiu, Minghao; Wang, Peng; Zhang, Yuqiang; Shindell, Drew; Zhang, Hongliang (19 July 2024). "Continuous wildfires threaten public and ecosystem health under climate change across continents". Frontiers of Environmental Science & Engineering. 18 (10): 130. Bibcode:2024FrESE..18..130C. doi:10.1007/s11783-024-1890-6. ISSN 2095-2201.
- Gherasim, Alina; Lee, Alison G.; Bernstein, Jonathan A. (November 14, 2023). "Impact of Climate Change on Indoor Air Quality". Immunology and Allergy Clinics of North America. 44 (1): 55–73. doi:10.1016/j.iac.2023.09.001. PMID 37973260. Archived from the original on November 15, 2023. Retrieved April 15, 2024.
- Lacressonnière, Gwendoline; Watson, Laura; Gauss, Michael; Engardt, Magnuz; Andersson, Camilla; Beekmann, Matthias; Colette, Augustin; Foret, Gilles; Josse, Béatrice; Marécal, Virginie; Nyiri, Agnes; Siour, Guillaume; Sobolowski, Stefan; Vautard, Robert (February 1, 2017). "Particulate matter air pollution in Europe in a +2 °C warming world". Atmospheric Environment. 154: 129–140. Bibcode:2017AtmEn.154..129L. doi:10.1016/j.atmosenv.2017.01.037. Archived from the original on November 17, 2023. Retrieved April 15, 2024.
- Lee, J; Lewis, A; Monks, P; Jacob, M; Hamilton, J; Hopkins, J; Watson, N; Saxton, J; Ennis, C; Carpenter, L (September 26, 2006). "Ozone photochemistry and elevated isoprene during the UK heatwave of august 2003". Atmospheric Environment. 40 (39): 7598–7613. Bibcode:2006AtmEn..40.7598L. doi:10.1016/j.atmosenv.2006.06.057. Archived from the original on October 26, 2022. Retrieved April 15, 2024.
- Salthammer, Tunga; Schieweck, Alexandra; Gu, Jianwei; Ameri, Shaghayegh; Uhde, Erik (August 7, 2018). "Future trends in ambient air pollution and climate in Germany – Implications for the indoor environment". Building and Environment. 143: 661–670. Bibcode:2018BuEnv.143..661S. doi:10.1016/j.buildenv.2018.07.050.
- Zhong, L.; Lee, C.-S.; Haghighat, F. (December 1, 2016). "Indoor ozone and climate change". Sustainable Cities and Society. 28: 466–472. doi:10.1016/j.scs.2016.08.020. Archived from the original on November 28, 2022. Retrieved April 15, 2024.
- Zhao, Jiangyue; Uhde, Erik; Salthammer, Tunga; Antretter, Florian; Shaw, David; Carslaw, Nicola; Schieweck, Alexandra (December 9, 2023). "Long-term prediction of the effects of climate change on indoor climate and air quality". Environmental Research. 243: 117804. doi:10.1016/j.envres.2023.117804. PMID 38042519.
- Niculita-Hirzel, Hélène (March 16, 2022). "Latest Trends in Pollutant Accumulations at Threatening Levels in Energy-Efficient Residential Buildings with and without Mechanical Ventilation: A Review". International Journal of Environmental Research and Public Health. 19 (6): 3538. doi:10.3390/ijerph19063538. ISSN 1660-4601. PMC 8951331. PMID 35329223.
- UK Health Security Agency (2024) . "Chapter 5: Impact of climate change policies on indoor environmental quality and health in UK housing". Health Effects of Climate Change (HECC) in the UK: 2023 report (published 15 January 2024).
- Ebi, Kristie L.; McGregor, Glenn (2008-11-01). "Climate Change, Tropospheric Ozone and Particulate Matter, and Health Impacts". Environmental Health Perspectives. 116 (11): 1449–1455. Bibcode:2008EnvHP.116.1449E. doi:10.1289/ehp.11463. PMC 2592262. PMID 19057695.
- ^ Diem, Jeremy E.; Stauber, Christine E.; Rothenberg, Richard (2017-05-16). Añel, Juan A. (ed.). "Heat in the southeastern United States: Characteristics, trends, and potential health impact". PLOS ONE. 12 (5): e0177937. Bibcode:2017PLoSO..1277937D. doi:10.1371/journal.pone.0177937. ISSN 1932-6203. PMC 5433771. PMID 28520817.
 Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License
Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License
- ^ Szopa, S., V. Naik, B. Adhikary, P. Artaxo, T. Berntsen, W.D. Collins, S. Fuzzi, L. Gallardo, A. Kiendler-Scharr, Z. Klimont, H. Liao, N. Unger, and P. Zanis, 2021: Chapter 6: Short-Lived Climate Forcers. In Climate Change 2021: The Physical Science Basis. Contribution of Working Group I to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change . Cambridge University Press, Cambridge, United Kingdom and New York, NY, USA, pp. 817–922, doi:10.1017/9781009157896.008.
- Sharma, Sumit; Sharma, Prateek; Khare, Mukesh; Kwatra, Swati (May 2016). "Statistical behavior of ozone in urban environment". Sustainable Environment Research. 26 (3): 142–148. Bibcode:2016SuEnR..26..142S. doi:10.1016/j.serj.2016.04.006.
- Health Aspects of Air Pollution with Particulate Matter, Ozone and Nitrogen Dioxide Archived 2012-04-14 at the Wayback Machine. WHO-Europe report 13–15 January 2003 (PDF)
- Answer to follow-up questions from CAFE (2004) Archived 2005-09-09 at the Wayback Machine (PDF)
- EPA Course Developers (2016-03-21). "Health Effects of Ozone in the General Population". EPA.
- Weinhold B (2008). "Ozone nation: EPA standard panned by the people". Environ. Health Perspect. 116 (7): A302–A305. doi:10.1289/ehp.116-a302. PMC 2453178. PMID 18629332.
- US EPA, OAR (2015-06-05). "Health Effects of Ozone Pollution". www.epa.gov. Retrieved 2023-04-29.
- Bezner Kerr, R., T. Hasegawa, R. Lasco, I. Bhatt, D. Deryng, A. Farrell, H. Gurney-Smith, H. Ju, S. Lluch-Cota, F. Meza, G. Nelson, H. Neufeldt, and P. Thornton, 2022: Chapter 5: Food, Fibre, and Other Ecosystem Products. In: Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change . Cambridge University Press, Cambridge, UK and New York, NY, USA, doi:10.1017/9781009325844.007.
- Springmann, Marco; Mason-D'Croz, Daniel; Robinson, Sherman; Garnett, Tara; Godfray, H Charles J; Gollin, Douglas; Rayner, Mike; Ballon, Paola; Scarborough, Peter (2016). "Global and regional health effects of future food production under climate change: a modelling study". The Lancet. 387 (10031): 1937–1946. doi:10.1016/S0140-6736(15)01156-3. PMID 26947322. S2CID 41851492.
- Haines, Andy; Ebi, Kristie (2019). Solomon, Caren G. (ed.). "The Imperative for Climate Action to Protect Health". New England Journal of Medicine. 380 (3): 263–273. doi:10.1056/NEJMra1807873. PMID 30650330. S2CID 58662802.
- Doherty, Susan; Clayton, Thomas J (2011). "The psychological impacts of global climate change". American Psychologist. 66 (4): 265–276. CiteSeerX 10.1.1.454.8333. doi:10.1037/a0023141. PMID 21553952.
- ^ Berry, Helen; Kathryn, Bowen; Kjellstrom, Tord (2009). "Climate change and mental health: a causal pathways framework". International Journal of Public Health. 55 (2): 123–132. doi:10.1007/s00038-009-0112-0. PMID 20033251. S2CID 22561555.
- ^ Charlson, Fiona; Ali, Suhailah; Benmarhnia, Tarik; Pearl, Madeleine; Massazza, Alessandro; Augustinavicius, Jura; Scott, James G. (2021). "Climate Change and Mental Health: A Scoping Review". International Journal of Environmental Research and Public Health. 18 (9): 4486. doi:10.3390/ijerph18094486. PMC 8122895. PMID 33922573.
 Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License
Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License
- Sakakibara, Chie (2008-10-01). ""our Home is Drowning": IÑupiat Storytelling and Climate Change in Point Hope, Alaskalaska*". Geographical Review. 98 (4): 473. doi:10.1111/j.1931-0846.2008.tb00312.x. ISSN 0016-7428.
- Anderegg, William R. L.; Abatzoglou, John T.; Anderegg, Leander D. L.; Bielory, Leonard; Kinney, Patrick L.; Ziska, Lewis (16 February 2021). "Anthropogenic climate change is worsening North American pollen seasons". Proceedings of the National Academy of Sciences. 118 (7): e2013284118. Bibcode:2021PNAS..11813284A. doi:10.1073/pnas.2013284118. PMC 7896283. PMID 33558232.
- Loladze I (May 2014). "Hidden shift of the ionome of plants exposed to elevated CO2 depletes minerals at the base of human nutrition". eLife. 3 (9): e02245. doi:10.7554/eLife.02245. PMC 4034684. PMID 24867639.
- Riahi, Keywan; van Vuuren, Detlef P.; Kriegler, Elmar; Edmonds, Jae; O'Neill, Brian C.; Fujimori, Shinichiro; Bauer, Nico; Calvin, Katherine; Dellink, Rob; Fricko, Oliver; Lutz, Wolfgang; Popp, Alexander; Cuaresma, Jesus Crespo; KC, Samir; Leimbach, Marian; Jiang, Leiwen; Kram, Tom; Rao, Shilpa; Emmerling, Johannes; Ebi, Kristie; Hasegawa, Tomoko; Havlík, Petr; Humpenoder, Florian; Da Silva, Lara Aleluia; Smith, Steve; Stehfest, Elke; Bosetti, Valentina; Eom, Jiyong; Gernaat, David; Masui, Toshihiko; Rogelj, Joeri; Strefler, Jessica; Drouet, Laurent; Krey, Volker; Luderer, Gunnar; Harmsen, Mathijs; Takahashi, Kiyoshi; Baumstark, Lavinia; Doelman, Johnathan C.; Kainuma, Mikiko; Klimont, Zbigniew; Marangoni, Giacomo; Lotze-Campen, Hermann; Obersteiner, Michael; Tabeau, Andrzej; Tavoni, Massimo (1 February 2017). "The Shared Socioeconomic Pathways and their energy, land use, and greenhouse gas emissions implications: An overview". Global Environmental Change. 42 (9): 153–168. Bibcode:2017GEC....42..153R. doi:10.1016/j.gloenvcha.2016.05.009. hdl:10044/1/78069.
- Mbow C, Rosenzweig C, Barioni LG, Benton TG, Herrero M, Krishnapillai M, et al. (2019). "Chapter 5: Food Security" (PDF). In Shukla PR, Skea J, Calvo Buendia E, Masson-Delmotte V, Pörtner HO, Roberts DC, et al. (eds.). Climate Change and Land: an IPCC special report on climate change, desertification, land degradation, sustainable land management, food security, and greenhouse gas fluxes in terrestrial ecosystems.
- Milius S (13 December 2017). "Worries grow that climate change will quietly steal nutrients from major food crops". Science News. Retrieved 21 January 2018.
- Bezner Kerr, R., T. Hasegawa, R. Lasco, I. Bhatt, D. Deryng, A. Farrell, H. Gurney-Smith, H. Ju, S. Lluch-Cota, F. Meza, G. Nelson, H. Neufeldt, and P. Thornton, 2022: Chapter 5: Food, Fibre, and Other Ecosystem Products. In: Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change . Cambridge University Press, Cambridge, UK and New York, NY, USA, doi:10.1017/9781009325844.007.
- Smith MR, Myers SS (27 August 2018). "Impact of anthropogenic CO2 emissions on global human nutrition". Nature Climate Change. 8 (9): 834–839. Bibcode:2018NatCC...8..834S. doi:10.1038/s41558-018-0253-3. ISSN 1758-678X. S2CID 91727337.
- Davis N (27 August 2018). "Climate change will make hundreds of millions more people nutrient deficient". The Guardian. Retrieved 29 August 2018.
- Epstein, Paul R.; Ferber, Dan (2011). "The Mosquito's Bite". Changing Planet, Changing Health: How the Climate Crisis Threatens Our Health and what We Can Do about it. University of California Press. pp. 29–61. ISBN 978-0-520-26909-5.
- McMichael, A.J.; Woodruff, R.E.; Hales, S. (11 March 2006). "Climate change and human health: present and future risks". The Lancet. 367 (9513): 859–869. doi:10.1016/s0140-6736(06)68079-3. PMID 16530580. S2CID 11220212.
- Epstein, Paul R.; Ferber, Dan (2011). "Mozambique". Changing Planet, Changing Health: How the Climate Crisis Threatens Our Health and what We Can Do about it. University of California Press. pp. 6–28. ISBN 978-0-520-26909-5.
- "NRDC: Climate Change Threatens Health: Drought". nrdc.org. 24 October 2022.
- Paerl, Hans W.; Huisman, Jef (4 April 2008). "Blooms Like It Hot". Science. 320 (5872): 57–58. CiteSeerX 10.1.1.364.6826. doi:10.1126/science.1155398. PMID 18388279. S2CID 142881074.
- ^ Tatters, Avery O.; Fu, Fei-Xue; Hutchins, David A. (February 2012). "High CO2 and Silicate Limitation Synergistically Increase the Toxicity of Pseudo-nitzschia fraudulenta". PLOS ONE. 7 (2): e32116. Bibcode:2012PLoSO...732116T. doi:10.1371/journal.pone.0032116. PMC 3283721. PMID 22363805.
- Wingert, Charles J.; Cochlan, William P. (July 2021). "Effects of ocean acidification on the growth, photosynthetic performance, and domoic acid production of the diatom Pseudo-nitzschia australis from the California Current System". Harmful Algae. 107: 102030. Bibcode:2021HAlga.10702030W. doi:10.1016/j.hal.2021.102030. PMID 34456015. S2CID 237841102.
- Workman, Annabelle; Blashki, Grant; Bowen, Kathryn J.; Karoly, David J.; Wiseman, John (April 2018). "The Political Economy of Health Co-Benefits: Embedding Health in the Climate Change Agenda". International Journal of Environmental Research and Public Health. 15 (4): 674. doi:10.3390/ijerph15040674. PMC 5923716. PMID 29617317.
- Molar, Roberto. "Reducing Emissions to Lessen Climate Change Could Yield Dramatic Health Benefits by 2030". Climate Change: Vital Signs of the Planet. Retrieved 1 December 2021.
- Swenarton, Nicole. "Climate action can lessen poverty and inequality worldwide". Rutgers University. Retrieved 1 December 2021.
- ^ IPCC (2022) Summary for policy makers in Climate Change 2022: Mitigation of Climate Change. Contribution of Working Group III to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change, Cambridge University Press, Cambridge, United Kingdom and New York, NY, United States
- Blondel, Benoît; Mispelon, Chloé; Ferguson, Julian (November 2011). Cycle more Often 2 cool down the planet ! (PDF). European Cyclists’ Federation. Archived from the original (PDF) on 17 February 2019. Retrieved 16 April 2019.
- "Cycling - health benefits". Better Health Channel. Retrieved 16 April 2019.
- A. Patz, Jonathan; C. Thomson, Madeleine (31 July 2018). "Climate change and health: Moving from theory to practice". PLOS Medicine. 15 (7): e1002628. doi:10.1371/journal.pmed.1002628. PMC 6067696. PMID 30063707.
- ^ Sampedro, Jon; Smith, Steven J.; Arto, Iñaki; González-Eguino, Mikel; Markandya, Anil; Mulvaney, Kathleen M.; Pizarro-Irizar, Cristina; Van Dingenen, Rita (2020). "Health co-benefits and mitigation costs as per the Paris Agreement under different technological pathways for energy supply". Environment International. 136: 105513. Bibcode:2020EnInt.13605513S. doi:10.1016/j.envint.2020.105513. hdl:10810/44202. PMID 32006762. S2CID 211004787.
- "MCC: Quality of life increases when we live, eat and travel energy-efficiently". idw-online.de. Retrieved 11 December 2021.
- Creutzig, Felix; Niamir, Leila; Bai, Xuemei; Callaghan, Max; Cullen, Jonathan; Díaz-José, Julio; Figueroa, Maria; Grubler, Arnulf; Lamb, William F.; Leip, Adrian; Masanet, Eric; Mata, Érika; Mattauch, Linus; Minx, Jan C.; Mirasgedis, Sebastian (2022). "Demand-side solutions to climate change mitigation consistent with high levels of well-being". Nature Climate Change. 12 (1): 36–46. Bibcode:2022NatCC..12...36C. doi:10.1038/s41558-021-01219-y. ISSN 1758-678X. S2CID 234275540.
- Green, Matthew (9 February 2021). "Fossil fuel pollution causes one in five premature deaths globally: study". Reuters. Archived from the original on 25 February 2021. Retrieved 5 March 2021.
- Vohra, Karn; Vodonos, Alina; Schwartz, Joel; Marais, Eloise A.; Sulprizio, Melissa P.; Mickley, Loretta J. (April 2021). "Global mortality from outdoor fine particle pollution generated by fossil fuel combustion: Results from GEOS-Chem". Environmental Research. 195: 110754. Bibcode:2021ER....19510754V. doi:10.1016/j.envres.2021.110754. PMID 33577774. S2CID 231909881.
- Anenberg, Susan C.; Schwartz, Joel; et al. (1 June 2012). "Global Air Quality and Health Co-benefits of Mitigating Near-Term Climate Change through Methane and Black Carbon Emission Controls". Environmental Health Perspectives. 120 (6): 831–839. Bibcode:2012EnvHP.120..831A. doi:10.1289/ehp.1104301. PMC 3385429. PMID 22418651.
- Vandyck, Toon; Keramidas, Kimon; et al. (22 November 2018). "Air quality co-benefits for human health and agriculture counterbalance costs to meet Paris Agreement pledges". Nature Communications. 9 (1): 4939. Bibcode:2018NatCo...9.4939V. doi:10.1038/s41467-018-06885-9. PMC 6250710. PMID 30467311.
- IASS/CSIR (2019a). "Improving health and reducing costs through renewable energy in South Africa. Assessing the co-benefits of decarbonising the power sector" (PDF). Archived (PDF) from the original on 2021-04-20.
- Nations, United. "Renewable energy – powering a safer future". United Nations. Retrieved 2024-05-13.
- Kemp, Luke; Xu, Chi; Depledge, Joanna; Ebi, Kristie L.; Gibbins, Goodwin; Kohler, Timothy A.; Rockström, Johan; Scheffer, Marten; Schellnhuber, Hans Joachim; Steffen, Will; Lenton, Timothy M. (2022). "Climate Endgame: Exploring catastrophic climate change scenarios". Proceedings of the National Academy of Sciences. 119 (34): e2108146119. Bibcode:2022PNAS..11908146K. doi:10.1073/pnas.2108146119. ISSN 0027-8424. PMC 9407216. PMID 35914185.
- ^ Hales, Simon; Kovats, Sari; Lloyd, Simon; Campbell-Lendrum, Diarmid, eds. (2014). Quantitative risk assessment of the effects of climate change on selected causes of death, 2030s and 2050s. Switzerland: World Health Organization. hdl:10665/134014. ISBN 978-92-4-150769-1.
- WHO (2009). "Ch. 2, Results: 2.6 Environmental risks". Global health risks: mortality and burden of disease attributable to selected major risks (PDF). Geneva, Switzerland: WHO Press. p. 24. ISBN 978-92-4-156387-1. Archived from the original (PDF) on 10 December 2013. Retrieved 4 October 2020.
- Crimmins, A.; Balbus, J.; Gamble, J.L.; Beard, C.B.; Bell, J.E.; Dodgen, D.; Eisen, R.J.; Fann, N.; Hawkins, M.D.; Herring, S.C.; Jantarasami, L.; Mills, D.M.; Saha, S.; Sarofim, M.C.; Trtanj, J.; Ziska, L. (2016). The Impacts of Climate Change on Human Health in the United States: A Scientific Assessment. Bibcode:2016icch.book.....C. doi:10.7930/J0R49NQX. ISBN 978-0-16-093241-0.
- ^ Kent E. Pinkerton , William N. Rom, ed. (2021). "1,2,6,12,13". Climate Change and Global Public Health. Humana. ISBN 978-3-030-54745-5.
- Pearce, Joshua M.; Parncutt, Richard (January 2023). "Quantifying Global Greenhouse Gas Emissions in Human Deaths to Guide Energy Policy". Energies. 16 (16): 6074. doi:10.3390/en16166074. ISSN 1996-1073.
- "Human-caused climate change may lead to 1 billion premature deaths over next century: Study". The Times of India. 2023-08-29. ISSN 0971-8257. Retrieved 2023-09-18.
- Li, Ang; Toll, Mathew; Martino, Erika; Wiesel, Illan; Botha, Ferdi; Bentley, Rebecca (March 2023). "Vulnerability and recovery: Long-term mental and physical health trajectories following climate-related disasters". Social Science & Medicine. 320 (115681): 115681. doi:10.1016/j.socscimed.2023.115681. PMID 36731303. S2CID 256159626.
- Bergstrand, Kelly; Mayer, Brian; Brumback, Babette; Zhang, Yi (June 2015). "Assessing the Relationship Between Social Vulnerability and Community Resilience to Hazards". Social Indicators Research. 122 (2): 391–409. doi:10.1007/s11205-014-0698-3. PMC 5739329. PMID 29276330.
- Epstein, Paul R. (6 October 2005). "Climate Change and Human Health". New England Journal of Medicine. 353 (14): 1433–1436. doi:10.1056/NEJMp058079. PMID 16207843.
- ^ "Human Health". Global Change. Retrieved 25 November 2020.
- Maibach, Edward W; Nisbet, Matthew; Baldwin, Paula; Akerlof, Karen; Diao, Guoqing (December 2010). "Reframing climate change as a public health issue: an exploratory study of public reactions". BMC Public Health. 10 (1): 299. doi:10.1186/1471-2458-10-299. PMC 2898822. PMID 20515503.
- Dasandi, Niheer; Graham, Hilary; Hudson, David; Jankin, Slava; vanHeerde-Hudson, Jennifer; Watts, Nick (20 October 2022). "Positive, global, and health or environment framing bolsters public support for climate policies". Communications Earth & Environment. 3 (1): 239. Bibcode:2022ComEE...3..239D. doi:10.1038/s43247-022-00571-x. S2CID 253041860.
- Anneliese Depoux; Mathieu Hémono; Sophie Puig-Malet; Romain Pédron; Antoine Flahault (2017). "Communicating climate change and health in the media". Public Health Rev. 38: 7. doi:10.1186/s40985-016-0044-1. PMC 5809944. PMID 29450079.
- Per Espen Stoknes (September 2017). How to transform apocalypse fatigue into action on global warming. TED (conference). Retrieved 1 March 2021.
- Davenport, Coral (4 April 2016). "Global Warming Linked to Public Health Risks, White House Says". The New York Times.
- Kavya Balaraman (17 March 2017). "Doctors Warn Climate Change Threatens Public Health; Physicians are noticing an influx of patients whose illnesses are directly or indirectly related to global warming". E&E News. Retrieved 20 March 2017 – via Scientific American.
- Dean Russell; Elisabeth Gawthrop; Veronica Penney; Ali Raj; Bridget Hickey (16 June 2020). "Deadly heat is killing Americans: A decade of inaction on climate puts lives at risk". The Guardian. Retrieved 1 March 2021.
- Operational framework for building climate resilient health systems. WHO. 2015. ISBN 978-92-4-156507-3.
- Hamilton, Ian; Kennard, Harry; McGushin, Alice; Höglund-Isaksson, Lena; Kiesewetter, Gregor; Lott, Melissa; Milner, James; Purohit, Pallav; Rafaj, Peter; Sharma, Rohit; Springmann, Marco (2021). "The public health implications of the Paris Agreement: a modelling study". The Lancet Planetary Health. 5 (2): e74–e83. doi:10.1016/S2542-5196(20)30249-7. PMC 7887663. PMID 33581069.
 This article incorporates text available under the CC BY 4.0 license.
This article incorporates text available under the CC BY 4.0 license.
- Katharine Murphy (2 September 2019). "Australian Medical Association declares climate change a health emergency". The Guardian. Retrieved 19 April 2020.
- Kotcher, John; Maibach, Edward; Miller, Jeni; Campbell, Eryn; Alqodmani, Lujain; Maiero, Marina; Wyns, Arthur (May 2021). "Views of health professionals on climate change and health: a multinational survey study". The Lancet Planetary Health. 5 (5): e316–e323. doi:10.1016/S2542-5196(21)00053-X. PMC 8099728. PMID 33838130.
External links
| Health impacts of climate change by country | |
|---|---|