| Revision as of 19:49, 15 September 2007 editUna Smith (talk | contribs)Autopatrolled, Pending changes reviewers23,024 edits Undid revision 158063043 by 88.198.136.147 (talk); link spam all or none← Previous edit | Latest revision as of 08:08, 13 November 2024 edit undoGuccizBud (talk | contribs)Extended confirmed users18,338 editsm →Mature teratoma: Copy edit ▸ Presentation ▸ Reference to in-article section visually augmented via section linking & crossreferencing templates.Tags: Mobile edit Mobile app edit Android app edit App select source | ||
| (530 intermediate revisions by more than 100 users not shown) | |||
| Line 1: | Line 1: | ||
| {{Short description|Type of germ cell tumor}} | |||
| {{Infobox_Disease | | |||
| {{Infobox medical condition (new) | |||
| Name = {{PAGENAME}} | | |||
| |
| name = Teratoma | ||
| | image = Mature cystic teratoma of ovary.jpg | |||
| Caption = | | |||
| | caption = A small (4 cm) ] of an ovary, discovered during ] | |||
| DiseasesDB = 3604 | | |||
| | field = ], ] | |||
| DiseasesDB_mult = {{DiseasesDB2|12952}} {{DiseasesDB2|12966}} | | |||
| | symptoms = Minimal, painless lump<ref name=Raj2007/><ref name=NORD2007/> | |||
| ICD10 = | | |||
| | complications = ], ], ]<ref name=Raj2007/><ref name=NORD2007/><ref name=Sab2014/> | |||
| ICD9 = | | |||
| |
| onset = | ||
| |
| duration = | ||
| | types = Mature, immature<ref name=NCI2017/> | |||
| MedlinePlus = | | |||
| | causes = Unknown<ref name=NORD2007/> | |||
| eMedicineSubj = med | | |||
| | risks = | |||
| eMedicineTopic = 3449 | | |||
| | diagnosis = ]<ref name=NORD2007/> | |||
| MeshID = D013724 | | |||
| | differential = ], ], ]<ref name=Dav2012/> | |||
| | prevention = | |||
| | treatment = Surgery, ]<ref name=Dav2012/><ref name=Pri2008/> | |||
| | medication = | |||
| | prognosis = | |||
| | frequency = 1 in 30,000 newborns (])<ref name=Cor2014/> | |||
| | deaths = | |||
| }} | }} | ||
| <!-- Definition and symptoms --> | |||
| {{wiktionarypar|teratoma}} | |||
| A '''teratoma''' is a ] made up of several types of ], such as ], ], ], or ].<ref name=NCI2017>{{cite web|title=NCI Dictionary of Cancer Terms|url=https://www.cancer.gov/publications/dictionaries/cancer-terms?cdrid=44248|website=National Cancer Institute|access-date=20 December 2017|date = 2011-02-02}}</ref> Teratomata typically form in the ] (where it is known as a ]), ], or ].<ref name="NCI2017" /> | |||
| A '''teratoma''' is a type of ] (specifically, a ]). The word teratoma comes from Greek and means roughly "monstrous tumor". Definitive diagnosis of a teratoma is based on its ]: a teratoma is a tumor with ] or ] components resembling normal derivatives of all three ]s. Rarely, not all three germ layers are identifiable. The tissues of a teratoma, although normal in themselves, may be quite different from surrounding tissues, and may be highly inappropriate, even grotesque (hence the ''monstrous''): teratomas have been reported to contain ], ], ] and very rarely more complex organs such as ]ball, ], and ]. Usually, however, a teratoma will contain no organs but rather one or more tissues normally found in organs such as the brain, thyroid, liver, and lung. | |||
| {{TOC limit|3}} | |||
| == |
==Symptoms== | ||
| Symptoms may be minimal if the tumor is small.<ref name="NORD2007" /> A testicular teratoma may present as a painless lump.<ref name="Raj2007" /> Complications may include ], ], or ].<ref name="Raj2007">{{cite book| vauthors = Raja SG |title=Access to Surgery: 500 single best answer questions in general and systematic pathology|date=2007|publisher=PasTest Ltd|isbn=9781905635368|page=508|url=https://books.google.com/books?id=p2VzWJBpHDAC&pg=PA508|language=en}}</ref><ref name="NORD2007" /><ref name="Sab2014">{{cite book | vauthors = Millet I, Perrochia H, Pages-Bouic E, Curros-Doyon F, Rathat G, Taourel P | chapter = CT and MR of Benign Ovarian Germ Cell Tumours | veditors = Saba L, Acharya UR, Guerriero S, Suri JS |title=Ovarian Neoplasm Imaging|date=2014|publisher=Springer Science & Business Media|isbn=9781461486336 |page=165 | chapter-url=https://books.google.com/books?id=AjLBBAAAQBAJ&pg=PA165|language=en}}</ref> | |||
| <!-- Cause and diagnosis --> | |||
| {{main|Germ cell tumor}} | |||
| They are a type of ] (a tumor that begins in the cells that give rise to ] or ]).<ref name=NCI2017/><ref name=NCI2017Mat>{{cite web|title=Mature teratoma|url=https://www.cancer.gov/publications/dictionaries/cancer-terms?cdrid=443575|website=National Cancer Institute|access-date=20 December 2017|date = 2011-02-02}}</ref> They are divided into two types: mature and immature.<ref name=NCI2017/> Mature teratomas include ]s and are generally ].<ref name=NCI2017Mat/> Immature teratomas may be ]ous.<ref name=NCI2017/><ref>{{cite book| veditors = Noor MR, Hseon TE, Jeffrey LJ | chapter = Ovarian Germ Cell Tumors |title=Gynaecologic Cancer: A Handbook for Students and Practitioners|date=2014|publisher=CRC Press|isbn=9789814463065|page=446| chapter-url=https://books.google.com/books?id=5-bMAwAAQBAJ&pg=PA446|language=en}}</ref> Most ovarian teratomas are mature.<ref name=Fal2007>{{cite book| vauthors = Falcone T, Hurd WW |title=Clinical Reproductive Medicine and Surgery|date=2007|publisher=Elsevier Health Sciences|isbn=978-0323033091|page=749|url=https://books.google.com/books?id=fOPtaEIKvcIC&pg=PA749|language=en}}</ref> In adults, testicular teratomas are generally cancerous.<ref>{{cite book| vauthors = Oyasu R, Yang XJ, Yoshida O |title=Questions in Daily Urologic Practice: Updates for Urologists and Diagnostic Pathologists |date=2009 |publisher=Springer Science & Business Media |isbn=9784431728191 |page=253 |url=https://books.google.com/books?id=mD5iUSqheb8C&pg=PA253 |language=en}}</ref> Definitive diagnosis is based on a ].<ref name=NORD2007>{{cite web|title=Sacrococcygeal Teratoma|url=https://rarediseases.org/rare-diseases/sacrococcygeal-teratoma/|website=NORD (National Organization for Rare Disorders)|access-date=20 December 2017|date=2007}}</ref> | |||
| <!-- Treatment --> | |||
| Teratomas belong to a class of tumors known as ]tous ] (NSGCT). All tumors of this class are the result of abnormal development of ] cells: ]s and ]. Teratomas of embryonal origin are ]; teratomas of germ cell origin may or may not be congenital (this is not known). The kind of pluripotent cell appears to be unimportant, apart from constraining the location of the teratoma in the body. | |||
| Treatment of coccyx, testicular, and ovarian teratomas is generally by surgery.<ref name=Dav2012/><ref name=Pri2008>{{cite book| vauthors = Price P, Sikora K, Illidge T |title=Treatment of Cancer | edition = Fifth |date=2008|publisher=CRC Press|isbn=9780340912218|page=713|url=https://books.google.com/books?id=KYIYF2MAUP4C&pg=PA713|language=en}}</ref><ref>{{cite book| vauthors = Hillard PJ, Hillard PA |title=The 5-minute Obstetrics and Gynecology Consult|date=2008|publisher=Lippincott Williams & Wilkins|isbn=9780781769426|page=140|url=https://books.google.com/books?id=fOoFIQOdIhkC&pg=PA140|language=en}}</ref> Testicular and immature ovarian teratomas are also frequently treated with ].<ref name=Pri2008/><ref name=Fal2007/> | |||
| <!-- Epidemiology --> | |||
| ===Location and incidence=== | |||
| Teratomas occur in the coccyx in about one in 30,000 newborns, making them one of the most common tumors in this age group.<ref name=Dav2012/><ref name=Cor2014>{{cite book| vauthors = Corton MM, Leveno KJ, Bloom SL, Hoffman BL |title=Williams Obstetrics 24/E (EBOOK)|date=2014|publisher=McGraw Hill Professional |isbn=9780071798945 |page=Chapter 16|url=https://books.google.com/books?id=TlPOAgAAQBAJ|language=en}}</ref> Females are affected more often than males.<ref name=Dav2012>{{cite book| vauthors = Davies M, Inglis G, Jardine L, Koorts P |title=Antenatal Consults: A Guide for Neonatologists and Paediatricians - E-Book|date=2012|publisher=Elsevier Health Sciences|isbn=978-0729581080 |page=298 |url=https://books.google.com/books?id=soTU42jrIkUC&pg=PA298|language=en}}</ref> Ovarian teratomas represent about a quarter of ] and are typically noticed during middle age.<ref name=Fal2007/> Testicular teratomas represent almost half of ]s.<ref>{{cite book| vauthors = Hart I, Newton RW |title=Endocrinology|date=2012|publisher=Springer Science & Business Media|isbn=9789401092982|page=157|url=https://books.google.com/books?id=QbjUBgAAQBAJ&pg=PA157|language=en}}</ref> They can occur in both children and adults.<ref>{{cite book| vauthors = McDougal WS, Wein AJ, Kavoussi LR, Partin AW, Peters CA, Ramchandani P |title=Campbell-Walsh Urology | edition = 10th |date=2011 |publisher = Elsevier Health Sciences|isbn=978-1455723171|page=663|url=https://books.google.com/books?id=tKcS1A2Q9dAC&pg=PA663|language=en}}</ref> The term comes from the Greek word for "monster"<ref>{{cite book| vauthors = Chang AE, Ganz PA, Hayes DF, Kinsella T, Pass HI, Schiller JH, Stone RM, Strecher V |title=Oncology: An Evidence-Based Approach|date=2007|publisher=Springer Science & Business Media |isbn=9780387310565 |page=848|url=https://books.google.com/books?id=vxh6u1-ETk0C&pg=PA848|language=en}}</ref> plus the "-oma" suffix used for tumors. | |||
| Teratomas can cause an autoimmune illness called ]. In this condition, the teratomas may contain B cells with NMDA-receptor specificities.<ref>{{cite journal | vauthors = Makuch M, Wilson R, Al-Diwani A, Varley J, Kienzler AK, Taylor J, Berretta A, Fowler D, Lennox B, Leite MI, Waters P, Irani SR | display-authors = 6 | title = N-methyl-D-aspartate receptor antibody production from germinal center reactions: Therapeutic implications | journal = Annals of Neurology | volume = 83 | issue = 3 | pages = 553–561 | date = March 2018 | pmid = 29406578 | pmc = 5925521 | doi = 10.1002/ana.25173 }}</ref> | |||
| Teratomas derived from germ cells occur in the ] in males and ] in females. Teratomas derived from embryonal cells usually occur on the body midline: in the brain, elsewhere inside the ], in the nose, in the tongue, under the tongue, and in the ] (cervical teratoma), ], ], and attached to the ]. However, teratomas may also occur elsewhere: very rarely in solid organs (most notably the heart and liver) and hollow organs (such as the stomach and bladder), and more commonly on the ]. Embryonal teratomas most commonly occur in the sacrococcygeal region: ] is the single most common tumor found in ]. | |||
| After teratoma removal surgery, a risk exists of regrowth in place, or in nearby organs.<ref>{{cite journal | vauthors = Choi KW, Jeon WJ, Chae HB, Park SM, Youn SJ, Shin HM, Sung RH, Lee SJ | display-authors = 6 | title = | language = ko | journal = The Korean Journal of Gastroenterology = Taehan Sohwagi Hakhoe Chi | volume = 42 | issue = 3 | pages = 242–245 | date = September 2003 | pmid = 14532748 | url = http://pdf.medrang.co.kr/Kjg/042/Kjg042-03-11.pdf }}</ref> | |||
| Of teratomas on the skull sutures, approximately 50% are found in or adjacent to the ]<ref></ref>. | |||
| ==Types== | |||
| Teratoma qualifies as a ], but is not extremely rare. Sacrococcygeal teratoma alone is diagnosed at birth in 1 out of 40,000 babies. Given the current ] ], this equals 5 per day or 1800 per year. Add to that number sacrococcygeal teratomas diagnosed later in life, and teratomas in other locations, and the ] approaches 10,000 new diagnoses of teratoma per year. | |||
| ===Mature teratoma===<!-- ] redirects here --> | |||
| ===Hypotheses of origin=== | |||
| ] | |||
| ] | |||
| A mature teratoma is a grade 0 teratoma. They are highly variable in form and histology, and may be solid, cystic, or a combination of the two. A mature teratoma often contains several different types of tissue such as ], ], and ]. Skin may surround a cyst and grow abundant ] {{xref|(see: {{slink||Dermoid cyst}})}}. Mature teratomas generally are benign, with 0.17–2% of mature cystic teratomas becoming malignant.<ref name="MandalBadhe2012">{{cite journal | vauthors = Mandal S, Badhe BA | title = Malignant transformation in a mature teratoma with metastatic deposits in the omentum: a case report | journal = Case Reports in Pathology | volume = 2012 | pages = 568062 | year = 2012 | pmid = 23082264 | pmc = 3469088 | doi = 10.1155/2012/568062 | doi-access = free }}</ref> | |||
| === Immature teratoma === | |||
| Concerning the origin of teratomas, there exist numerous hypotheses.<ref name="Gonzalez-Crussi1982">Gonzalez-Crussi, F. (1982) Extragonadal Teratomas. Atlas of Tumor Pathology, Second Series, Fascicle 18. ], Washington D.C.</ref> These hypotheses are not to be confused with the unrelated hypothesis that ] (see below) is not a teratoma at all but rather a ]. | |||
| Immature teratoma is the malignant counterpart of the mature teratoma and contains immature tissues which typically show ] ]al histopathology. Immature teratoma has one of the lowest rates of ] of any tumor type and results from one of five mechanisms of ].<ref name=":0">{{cite journal | vauthors = Heskett MB, Sanborn JZ, Boniface C, Goode B, Chapman J, Garg K, Rabban JT, Zaloudek C, Benz SC, Spellman PT, Solomon DA, Cho RJ | display-authors = 6 | title = Multiregion exome sequencing of ovarian immature teratomas reveals 2N near-diploid genomes, paucity of somatic mutations, and extensive allelic imbalances shared across mature, immature, and disseminated components | journal = Modern Pathology | volume = 33 | issue = 6 | pages = 1193–1206 | date = June 2020 | pmid = 31911616 | pmc = 7286805 | doi = 10.1038/s41379-019-0446-y }}</ref> | |||
| === Gliomatosis peritoneii === | |||
| Gliomatosis peritoneii, which presents as a deposition of mature glial cells in the peritoneum, is almost exclusively seen in conjunction with cases of ovarian teratoma. Through genetic studies of exome sequence, it was found that gliomatosis is genetically identical to the parent ovarian tumor and developed from cells that disseminate from the ovarian teratoma.<ref name=":0" /> | |||
| === Dermoid cyst === | === Dermoid cyst === | ||
| A ] is a mature teratoma containing hair (sometimes very abundant) and other structures characteristic of normal skin and other tissues derived from the ectoderm. The term is most often applied to teratoma on the skull sutures and in the ovaries of females. | A ] is a mature cystic teratoma containing hair (sometimes very abundant) and other structures characteristic of normal skin and other tissues derived from the ]. The term is most often applied to teratoma on the skull sutures and in the ovaries of females.{{citation needed|date=June 2020}} | ||
| {{clear left}} | |||
| === Fetus in fetu and fetiform teratoma=== | === Fetus ''in fetu'' and fetiform teratoma=== | ||
| ] and fetiform teratoma are rare forms of mature teratomas that include one or more components resembling a malformed fetus. Both forms may contain or appear to contain complete organ systems, even major body parts, such as a torso or limbs. Fetus ''in fetu ''differs from fetiform teratoma in having an apparent ] and ].<ref name="Gonzalez-Crussi1982"/> | |||
| Most authorities agree that fetiform teratomas are highly developed mature teratomas; the natural history of fetus in fetu |
Most authorities agree that fetiform teratomas are highly developed mature teratomas; the natural history of fetus ''in fetu'' is controversial.<ref name="Gonzalez-Crussi1982"/> It has been noted that fetiform teratoma is reported more often (by gynecologists) in ovarian teratomas, and fetus ''in fetu'' is reported more often (by general surgeons) in retroperitoneal teratomas. Fetus ''in fetu'' has often been interpreted as a ] growing within its ]. As such, this interpretation assumes a special complication of ]ning, one of several grouped under the term ]. In many cases, the fetus ''in fetu'' is reported to occupy a fluid-filled cyst within a mature teratoma.<ref name="pmid6724790">{{cite journal | vauthors = Abbott TM, Hermann WJ, Scully RE | title = Ovarian fetiform teratoma (homunculus) in a 9-year-old girl | journal = International Journal of Gynecological Pathology | volume = 2 | issue = 4 | pages = 392–402 | year = 1984 | pmid = 6724790 | doi = 10.1097/00004347-198404000-00007 }}</ref><ref>{{cite journal | vauthors = Saito K, Katsumata Y, Hirabuki T, Kato K, Yamanaka M | title = Fetus-in-fetu: parasite or neoplasm? A study of two cases | journal = Fetal Diagnosis and Therapy | volume = 22 | issue = 5 | pages = 383–388 | year = 2007 | pmid = 17556829 | doi = 10.1159/000103301 | s2cid = 57099054 }}</ref><ref>{{cite journal | vauthors = Kajbafzadeh AM, Baharnoori M | title = Fetus in fetu | journal = The Canadian Journal of Urology | volume = 13 | issue = 5 | pages = 3277–3278 | date = October 2006 | pmid = 17076951 }}</ref><ref>{{cite journal | vauthors = Chua JH, Chui CH, Sai Prasad TR, Jabcobsen AS, Meenakshi A, Hwang WS | title = Fetus-in-fetu in the pelvis: report of a case and literature review | journal = Annals of the Academy of Medicine, Singapore | volume = 34 | issue = 10 | pages = 646–649 | date = November 2005 | pmid = 16382253 | url = http://www.annals.edu.sg/pdf/34VolNo10200511/V34N10p646.pdf }}</ref> Cysts within mature teratomas may have partially-developed organ systems: reports include cases of partial ], ] and a rudimentary, beating heart.<ref>{{cite journal | vauthors = Lee YH, Kim SG, Choi SH, Kim IS, Kim SH | title = Ovarian mature cystic teratoma containing homunculus: a case report | journal = Journal of Korean Medical Science | volume = 18 | issue = 6 | pages = 905–907 | date = December 2003 | pmid = 14676454 | pmc = 3055135 | doi = 10.3346/jkms.2003.18.6.905 | url = http://jkms.kams.or.kr/2003/pdf/12905.pdf | url-status = dead | archive-url = https://web.archive.org/web/20110722140946/http://jkms.kams.or.kr/2003/pdf/12905.pdf | archive-date = 2011-07-22 }}<!-- also available at: http://www.biomedsearch.com/attachments/00/14/67/64/14676454/14676454.pdf and http://jkms.xmlink.kr/Synapse/Data/PDFData/0063JKMS/jkms-18-905.pdf --></ref><ref>{{cite journal | vauthors = Kazez A, Ozercan IH, Erol FS, Faik Ozveren M, Parmaksiz E | title = Sacrococcygeal heart: a very rare differentiation in teratoma | journal = European Journal of Pediatric Surgery | volume = 12 | issue = 4 | pages = 278–280 | date = August 2002 | pmid = 12369008 | doi = 10.1055/s-2002-34483 | s2cid = 260136953 }}</ref> | ||
| |author=Kazez A, Ozercan IH, Erol FS, Faik Ozveren M, Parmaksiz E | |||
| |title=Sacrococcygeal heart: a very rare differentiation in teratoma. | |||
| |journal=European journal of pediatric surgery (Zeitschrift für Kinderchirurgie) | |||
| |volume=12 | |||
| |issue=4 | |||
| |pages=278-80 | |||
| |year=2002 | |||
| |pmid=12369008 | |||
| |doi=10.1055/s-2002-34483 | |||
| |issn= | |||
| }}{{PMID|12369008}}</ref> | |||
| Regardless of whether fetus in fetu and fetiform teratoma are one entity or two, they are distinct from and not to be confused with ]. | Regardless of whether fetus ''in fetu'' and fetiform teratoma are one entity or two, they are distinct from and not to be confused with ]. | ||
| === Struma ovarii === | === Struma ovarii === | ||
| {{main|Struma ovarii}} | |||
| A '''struma ovarii''' (literally: ] of the ovary) is a rare form of mature teratoma that contains mostly ] tissue. Despite its name, struma ovarii is not restricted to the ovary. Only 5% of struma ovarii are malignant.{{Fact|date=June 2007}} | |||
| A struma ovarii (also known as ] of the ovary or ovarian goiter) is a rare form of mature teratoma that contains mostly ] tissue.<ref>{{cite journal | vauthors = Frysak Z, Schovanek J, Halenka M, Metelkova I, Duskova M, Karasek D | title = Ovarian Goiter as a Rare Cause of Hyperthyroidism | journal = Acta Endocrinologica | volume = 12 | issue = 3 | pages = 335–338 | date = 2016 | pmid = 31149110 | pmc = 6535264 | doi = 10.4183/aeb.2016.335 }}</ref> | |||
| === Epignathus === | |||
| ==Pathology classification of individual teratomas== | |||
| {{main|Epignathus}} | |||
| Epignathus is a rare teratoma originating in the oropharyngeal area that occurs ''in utero''. It presents with a mass protruding from the mouth at birth. Untreated, breathing is impossible. An ] is the recommended initial treatment. | |||
| Teratomas commonly are classified using the Gonzalez-Crussi<ref name="Gonzalez-Crussi1982"/> grading system: 0 or mature (]); 1 or immature, probably benign; 2 or immature, possibly ] (]ous); and 3 or frankly malignant. See also ]. Teratomas are also classified by their content: a solid teratoma contains only tissues (perhaps including more complex structures); a cystic teratoma contain only pockets of fluid or semi-fluid such as ], ], or fat; a mixed teratoma contains both solid and cystic parts. Cystic teratomas usually are grade 0 and, conversely, grade 0 teratomas usually are cystic. | |||
| ==Fetal Teratomas== | |||
| Grade 0, 1 and 2 pure teratomas have the potential to become malignant (grade 3), and malignant pure teratomas have the potential to ]. These rare forms of '''teratoma with malignant transformation''' may contain elements of somatic (non germ cell) malignancy such as ], ] or ].<ref name="pmid17080330">{{cite journal | |||
| Teratomas may be found in babies, children, and adults. Teratomas of embryonal origin are most often found in babies at birth, in young children, and, since the advent of ], in fetuses. | |||
| |author=Harms D, Zahn S, Göbel U, Schneider DT | |||
| |title=Pathology and molecular biology of teratomas in childhood and adolescence. | |||
| |journal=Klinische Pädiatrie | |||
| |volume=218 | |||
| |issue=6 | |||
| |pages=296-302 | |||
| |year=2006 | |||
| |pmid=17080330 | |||
| |doi=10.1055/s-2006-942271 | |||
| }}</ref> | |||
| A teratoma may contain elements of other germ cell tumors, in which case it is not a pure teratoma but rather is a '''mixed''' ] and is malignant. In infants and young children, these elements usually are ], followed by ]. Finally, a teratoma can be pure and not malignant yet highly aggressive: this is exemplified by '''growing teratoma syndrome''', in which chemotherapy eliminates the malignant elements of a mixed tumor, leaving pure teratoma which paradoxically begins to grow very rapidly. | |||
| The most diagnosed fetal teratomas are ] (Altman types I, II, and III) and cervical (neck) teratoma. Because these teratomas project from the fetal body into the surrounding ], they can be seen during routine prenatal ultrasound exams. Teratomas within the fetal body are less easily seen with ultrasound; for these, MRI of the pregnant uterus is more informative.<ref>{{cite journal | vauthors = Danzer E, Hubbard AM, Hedrick HL, Johnson MP, Wilson RD, Howell LJ, Flake AW, Adzick NS | display-authors = 6 | title = Diagnosis and characterization of fetal sacrococcygeal teratoma with prenatal MRI | journal = AJR. American Journal of Roentgenology | volume = 187 | issue = 4 | pages = W350–W356 | date = October 2006 | pmid = 16985105 | doi = 10.2214/AJR.05.0152 }}</ref><ref>{{cite journal | vauthors = Kocaoglu M, Frush DP | title = Pediatric presacral masses | journal = Radiographics | volume = 26 | issue = 3 | pages = 833–857 | year = 2006 | pmid = 16702458 | doi = 10.1148/rg.263055102 }}</ref> | |||
| === Teratoma graded benign may prove to be malignant === | |||
| ===Complications=== | |||
| A "benign" or grade 0 teratoma nonetheless has a non-zero risk of malignancy. Recurrence with malignant ] has been reported in many cases of formerly grade 0 teratoma, even in fetiform teratoma.<ref name="pmid17561476">{{cite journal | |||
| Teratomas are not dangerous for the fetus unless either a ] occurs or a large amount of blood flows through the tumor (known as vascular steal). The mass effect frequently consists of obstruction of normal passage of fluids from surrounding organs. The vascular steal can place a strain on the growing heart of the fetus, even resulting in heart failure, thus must be monitored by fetal ]. | |||
| | author = Chen YH, Chang CH, Chen KC, Diau GY, Loh IW, Chu CC | |||
| | title = Malignant transformation of a well-organized sacrococcygeal fetiform teratoma in a newborn male. | |||
| | journal = J. Formos. Med. Assoc. | |||
| | volume = 106 | |||
| | issue = 5 | |||
| | pages = 400-2 | |||
| | year = 2007 | |||
| | pmid = 17561476 | |||
| | doi = | |||
| | issn = | |||
| }} (publisher offers free full text PDF to registered users)</ref> | |||
| ==Pathophysiology== | |||
| === Teratoma with malignant transformation=== | |||
| {{main|Germ cell tumor}} | |||
| Teratomas belong to a class of tumors known as ]tous ]. All tumors of this class are the result of abnormal development of ] cells: ]s and ]. Teratomas of embryonic origin are ]; teratomas of germ cell origin may or may not be congenital. The kind of pluripotent cell appears to be unimportant, apart from constraining the location of the teratoma in the body. | |||
| Teratomas derived from germ cells occur in the ] and ]. Teratomas derived from embryonic cells usually occur on the subject's midline: in the brain, elsewhere in the ], in the nose, in the tongue, under the tongue, and in the ] (cervical teratoma), ], ], and attached to the ]. Teratomas may also occur elsewhere: very rarely in solid organs (most notably the heart and liver) and hollow organs (such as the stomach and bladder), and more commonly on the ]. | |||
| A '''teratoma with malignant transformation''' or '''TMT''' is a very rare form of teratoma that may contain elements of somatic (non germ cell) malignant tumors such as ], ] or ].<ref name="pmid17080330">{{cite journal | |||
| |author=Harms D, Zahn S, Göbel U, Schneider DT | |||
| |title=Pathology and molecular biology of teratomas in childhood and adolescence. | |||
| |journal=Klinische Pädiatrie | |||
| |volume=218 | |||
| |issue=6 | |||
| |pages=296-302 | |||
| |year=2006 | |||
| |pmid=17080330 | |||
| |doi=10.1055/s-2006-942271 | |||
| }}</ref> Of 641 children with pure teratoma, 9 developed TMT<ref>{{cite journal | |||
| | author = Biskup W, Calaminus G, Schneider DT, Leuschner I, Göbel U | |||
| | title = Teratoma with malignant transformation: experiences of the cooperative GPOH protocols MAKEI 83/86/89/96. | |||
| | journal = Klinische Pädiatrie | |||
| | volume = 218 | |||
| | issue = 6 | |||
| | pages = 303-8 | |||
| | year = 2006 | |||
| | pmid = 17080331 | |||
| | doi = 10.1055/s-2006-942272 | |||
| | issn = | |||
| }}</ref>: 5 ], 2 ], and 2 embryonal (here, these last are classified among germ cell tumors). | |||
| Teratoma rarely include more complicated body parts such as ], ],<ref>{{cite journal | vauthors = Shintaku M, Sakuma T, Ohbayashi C, Maruo M | title = Well-formed cerebellum and brainstem-like structures in a mature ovarian teratoma: Neuropathological observations | language = en-US | journal = Neuropathology | volume = 37 | issue = 2 | pages = 122–128 | date = April 2017 | pmid = 28042664 | doi = 10.1111/neup.12360 | s2cid = 25588284 }}</ref> ],<ref name="pmid6540049">{{cite journal | vauthors = Chi JG, Lee YS, Park YS, Chang KY | title = Fetus-in-fetu: report of a case | journal = American Journal of Clinical Pathology | volume = 82 | issue = 1 | pages = 115–119 | date = July 1984 | pmid = 6540049 | doi = 10.1093/ajcp/82.1.115 }}</ref><ref name="pmid9841706">{{cite journal | vauthors = Sergi C, Ehemann V, Beedgen B, Linderkamp O, Otto HF | title = Huge fetal sacrococcygeal teratoma with a completely formed eye and intratumoral DNA ploidy heterogeneity | journal = Pediatric and Developmental Pathology | volume = 2 | issue = 1 | pages = 50–57 | year = 1999 | pmid = 9841706 | doi = 10.1007/s100249900089 | s2cid = 22847474 }}</ref> or ].<ref name="pmid19184054">{{cite journal | vauthors = Arlikar JD, Mane SB, Dhende NP, Sanghavi Y, Valand AG, Butale PR | title = Fetus in fetu: two case reports and review of literature | journal = Pediatric Surgery International | volume = 25 | issue = 3 | pages = 289–292 | date = March 2009 | pmid = 19184054 | doi = 10.1007/s00383-009-2328-8 | s2cid = 11210782 }}</ref> | |||
| === Extraspinal ependymoma === | |||
| ===Hypotheses of origin=== | |||
| ], usually considered to be a ] (a type of non-germ cell tumor), may be an unusual form of mature teratoma.<ref>Aktuğ T, Hakgüder G, Sarioğlu S, Akgür FM, Olguner M, Pabuçcuoğlu U. (2000) Sacrococcygeal extraspinal ependymomas: the role of coccygectomy. J Pediatr Surg. 35(3):515-518. </ref>{{Fact|date=June 2007}} | |||
| Concerning the origin of teratomas, numerous hypotheses exist.<ref name="Gonzalez-Crussi1982">Gonzalez-Crussi F (1982) Extragonadal Teratomas. Atlas of Tumor Pathology, Second Series, Fascicle 18. ], Washington D.C.</ref> These hypotheses are not to be confused with the unrelated hypothesis that fetus ''in fetu'' (see below) is not a teratoma at all, but rather a ]. | |||
| ==Diagnosis== | |||
| ==Initial diagnosis== | |||
| ] | |||
| ] of a teratoma showing tissue from all three ]s: ] (immature ] - left-upper), ] (gastrointestinal glands - center-bottom) and ] (epidermis - right)]] | |||
| Teratomas are thought to originate ''in utero'', so can be considered ] tumors. Many teratomas are not diagnosed until much later in childhood or in adulthood. Large tumors are more likely to be diagnosed early on. Sacrococcygeal and cervical teratomas are often detected by prenatal ]. Additional diagnostic methods may include prenatal ]. In rare circumstances, the tumor is so large that the fetus may be damaged or die. In the case of large sacrococcygeal teratomas, a significant portion of the fetus' ] is redirected toward the teratoma (a phenomenon called ]), causing ], or ], of the fetus. In certain cases, ] may be indicated. | |||
| Beyond the newborn period, symptoms of a teratoma depend on its location and organ of origin. Ovarian teratomas often present with abdominal or ], caused by ] of the ovary or irritation of its ligaments. A recently discovered condition where ovarian teratomas cause encephalitis associated with antibodies against the ] receptor antibody (NMDAR) - often referred to as "]", was identified as a serious complication. Patients develop a multistage illness that progresses from psychosis, memory deficits, seizures, and language disintegration into a state of unresponsiveness with catatonic features often associated with abnormal movements, and autonomic and breathing instability.<ref>{{cite journal | vauthors = Dalmau J, Lancaster E, Martinez-Hernandez E, Rosenfeld MR, Balice-Gordon R | title = Clinical experience and laboratory investigations in patients with anti-NMDAR encephalitis | journal = The Lancet. Neurology | volume = 10 | issue = 1 | pages = 63–74 | date = January 2011 | pmid = 21163445 | pmc = 3158385 | doi = 10.1016/S1474-4422(10)70253-2 }}</ref> Testicular teratomas present as a palpable mass in the testis; ] teratomas often cause compression of the lungs or the airways and may present with ] and/or respiratory symptoms. | |||
| Teratomas are thought to be present since birth, or even before birth, and therefore can be considered ] tumors. However, many teratomas are not diagnosed until much later in childhood or in adulthood. Large tumors are more likely to be diagnosed early on. Sacrococcygeal and cervical teratomas are often detected by prenatal ]. Additional diagnostic methods may include prenatal ]. In rare circumstances, the tumor is so large that the ] may be damaged or die. In the case of large sacrococcygeal teratomas, a significant portion of the fetus' ] is redirected toward the teratoma (a phenomenon called ]), causing ], or ], of the fetus. In certain cases, ] may be indicated. | |||
| Some teratomas contain ] elements, which secrete ]. Its detection may help to confirm the diagnosis and is often used as a marker for recurrence or treatment efficacy, but is rarely the method of initial diagnosis. (Maternal serum ] is a useful ] for other fetal conditions, including ], ], and ] defects such as ].) | |||
| Beyond the newborn period, symptoms of a teratoma depend on its location and organ of origin. ] teratomas often present with abdominal or ], caused by ] of the ] or irritation of its ligaments. Testicular teratomas present as a palpable mass in the ]; ] teratomas often cause compression of the lungs or the airways and may present with ] and/or respiratory symptoms. | |||
| ===Classification=== | |||
| Some teratomas contain ] elements, which secrete ] (AFP). Detection of AFP may help to confirm the diagnosis and is often used as a marker for recurrence or treatment efficacy, but is rarely the method of initial diagnosis. (Maternal serum ], or MSAFP, is a useful ] for other fetal conditions, including ], ] and ] defects such as ]). | |||
| Regardless of location in the body, a teratoma is classified according to a ] system. This indicates whether ] or ] may be needed in addition to surgery. Teratomas commonly are classified using the ]<ref name="Gonzalez-Crussi1982"/> grading system: 0 or mature (]); 1 or immature, probably benign; 2 or immature, possibly ] (cancerous); and 3 or frankly malignant. If frankly malignant, the tumor is a cancer for which additional cancer staging applies.{{citation needed|date=June 2020}} | |||
| Teratomas are also classified by their content; a solid teratoma contains only tissues (perhaps including more complex structures); a cystic teratoma contains only pockets of fluid or semifluid such as ], ], or fat; a mixed teratoma contains both solid and cystic parts. Cystic teratomas usually are grade 0 and, conversely, grade 0 teratomas usually are cystic. | |||
| ==Time of presentation== | |||
| Grades 0, 1, and 2 pure teratomas have the potential to become malignant (grade 3), and malignant pure teratomas have the potential to ]. These rare forms of teratoma with malignant transformation may contain elements of somatic (not germ cell) malignancy such as ], ], or ].<ref name="pmid17080330">{{cite journal | vauthors = Harms D, Zahn S, Göbel U, Schneider DT | title = Pathology and molecular biology of teratomas in childhood and adolescence | journal = Klinische Padiatrie | volume = 218 | issue = 6 | pages = 296–302 | year = 2006 | pmid = 17080330 | doi = 10.1055/s-2006-942271 | s2cid = 20627932 }}</ref> | |||
| Teratomas of germ cell origin usually are found (ie, ''present'') in adult men and women, but they may also be found in children and infants. Teratomas of embryonal origin are most often found in babies at birth, in young children, and, since the advent of ], in fetuses. | |||
| A teratoma may contain elements of other germ cell tumors, in which case it is not a pure teratoma, but rather is a mixed ] and is malignant. In infants and young children, these elements usually are ], followed by ]. Finally, a teratoma can be pure and not malignant yet highly aggressive; this is exemplified by growing teratoma syndrome, in which chemotherapy eliminates the malignant elements of a mixed tumor, leaving pure teratoma, which paradoxically begins to grow very rapidly.<ref>{{cite journal | vauthors = Scavuzzo A, Santana Ríos ZA, Noverón NR, Jimenez Ríos MA | title = Growing teratoma syndrome | journal = Case Reports in Urology | volume = 2014 | pages = 139425 | date = 2014 | pmid = 25197607 | pmc = 4150507 | doi = 10.1155/2014/139425 | doi-access = free }}</ref> | |||
| ==== Malignant transformation==== | |||
| The most commonly diagnosed fetal teratomas are ] (Altman types I, II, and III) and cervical (neck) teratoma. Because these teratomas project from the fetal body into the surrounding ], they can be seen during routine prenatal ultrasound exams. Teratomas within the fetal body are less easily seen with ultrasound; for these, MRI of the pregnant uterus is more informative.<ref>Diagnosis and characterization of fetal sacrococcygeal teratoma with prenatal MRI. | |||
| A "benign" grade 0 (mature) teratoma nonetheless has a risk of malignancy. Recurrence with malignant ] has been reported in cases of formerly benign mature teratoma,<ref name="pmid9781660">{{cite journal | vauthors = Ohno Y, Kanematsu T | title = An endodermal sinus tumor arising from a mature cystic teratoma in the retroperitoneum in a child: is a mature teratoma a premalignant condition? | journal = Human Pathology | volume = 29 | issue = 10 | pages = 1167–1169 | date = October 1998 | pmid = 9781660 | doi = 10.1016/S0046-8177(98)90432-4 }}</ref><ref name="pmid17564180">{{cite journal | vauthors = Utsuki S, Oka H, Sagiuchi T, Shimizu S, Suzuki S, Fujii K | title = Malignant transformation of intracranial mature teratoma to yolk sac tumor after late relapse. Case report | journal = Journal of Neurosurgery | volume = 106 | issue = 6 | pages = 1067–1069 | date = June 2007 | pmid = 17564180 | doi = 10.3171/jns.2007.106.6.1067 | s2cid = 23864999 }}</ref> even in fetiform teratoma and fetus in fetu.<ref name="pmid17561476">{{cite journal | vauthors = Chen YH, Chang CH, Chen KC, Diau GY, Loh IW, Chu CC | title = Malignant transformation of a well-organized sacrococcygeal fetiform teratoma in a newborn male | journal = Journal of the Formosan Medical Association = Taiwan Yi Zhi | volume = 106 | issue = 5 | pages = 400–402 | date = May 2007 | pmid = 17561476 | doi = 10.1016/S0929-6646(09)60326-0 | doi-access = }}{{Dead link|date=June 2018 |bot=InternetArchiveBot |fix-attempted=no }}</ref><ref name="pmid9349774">{{cite journal | vauthors = Hopkins KL, Dickson PK, Ball TI, Ricketts RR, O'Shea PA, Abramowsky CR | title = Fetus-in-fetu with malignant recurrence | journal = Journal of Pediatric Surgery | volume = 32 | issue = 10 | pages = 1476–1479 | date = October 1997 | pmid = 9349774 | doi = 10.1016/S0022-3468(97)90567-4 }}</ref> ] has been found in a mature cystic teratoma at the time of initial surgery.<ref name="pmid18592797">{{cite journal | vauthors = Arioz DT, Tokyol C, Sahin FK, Koker G, Yilmaz S, Yilmazer M, Ozalp S | title = Squamous cell carcinoma arising in a mature cystic teratoma of the ovary in young patient with elevated carbohydrate antigen 19-9 | journal = European Journal of Gynaecological Oncology | volume = 29 | issue = 3 | pages = 282–284 | year = 2008 | pmid = 18592797 }}</ref> A grade 1 immature teratoma that appears to be benign (e.g., because AFP is not elevated) has a much higher risk of malignancy, and requires adequate follow-up.<ref name="pmid15895292">{{cite journal | vauthors = Muscatello L, Giudice M, Feltri M | title = Malignant cervical teratoma: report of a case in a newborn | journal = European Archives of Oto-Rhino-Laryngology | volume = 262 | issue = 11 | pages = 899–904 | date = November 2005 | pmid = 15895292 | doi = 10.1007/s00405-005-0917-2 | s2cid = 11556991 }}</ref><ref name="pmid15928937">{{cite journal | vauthors = Ukiyama E, Endo M, Yoshida F, Tezuka T, Kudo K, Sato S, Akatsuka S, Hata J | display-authors = 6 | title = Recurrent yolk sac tumor following resection of a neonatal immature gastric teratoma | journal = Pediatric Surgery International | volume = 21 | issue = 7 | pages = 585–588 | date = July 2005 | pmid = 15928937 | doi = 10.1007/s00383-005-1404-y | s2cid = 40147917 }}</ref><ref name="pmid7508500">{{cite journal | vauthors = Bilik R, Shandling B, Pope M, Thorner P, Weitzman S, Ein SH | title = Malignant benign neonatal sacrococcygeal teratoma | journal = Journal of Pediatric Surgery | volume = 28 | issue = 9 | pages = 1158–1160 | date = September 1993 | pmid = 7508500 | doi = 10.1016/0022-3468(93)90154-D }}</ref><ref name="pmid7692755">{{cite journal | vauthors = Hawkins E, Issacs H, Cushing B, Rogers P | title = Occult malignancy in neonatal sacrococcygeal teratomas. A report from a Combined Pediatric Oncology Group and Children's Cancer Group study | journal = The American Journal of Pediatric Hematology/Oncology | volume = 15 | issue = 4 | pages = 406–409 | date = November 1993 | pmid = 7692755 }}</ref> | |||
| Danzer E, Hubbard AM, Hedrick HL, Johnson MP, Wilson RD, Howell LJ, Flake AW, Adzick NS. | |||
| This grade of teratoma also may be difficult to diagnose correctly. It can be confused with other small round cell neoplasms such as neuroblastoma, small cell carcinoma of hypercalcemic type, primitive neuroectodermal tumor, Wilm's tumor, desmoplastic small round cell tumor, and non-Hodgkin ].<ref name="pmid18618728">{{cite journal | vauthors = Ramalingam P, Teague D, Reid-Nicholson M | title = Imprint cytology of high-grade immature ovarian teratoma: a case report, literature review, and distinction from other ovarian small round cell tumors | journal = Diagnostic Cytopathology | volume = 36 | issue = 8 | pages = 595–599 | date = August 2008 | pmid = 18618728 | doi = 10.1002/dc.20849 | s2cid = 21066080 }}</ref> | |||
| AJR Am J Roentgenol. 2006 Oct;187(4):W350-6. | |||
| PMID: 16985105 | |||
| </ref><ref>Pediatric presacral masses. | |||
| Kocaoglu M, Frush DP. | |||
| Radiographics. 2006 May-Jun;26(3):833-57. Review. | |||
| PMID: 16702458 | |||
| </ref> | |||
| A teratoma with malignant transformation is a very rare form of teratoma that may contain elements of somatic malignant tumors such as leukemia, carcinoma, or sarcoma.<ref name="pmid17080330"/> Of 641 children with pure teratoma, nine developed TMT:<ref>{{cite journal | vauthors = Biskup W, Calaminus G, Schneider DT, Leuschner I, Göbel U | title = Teratoma with malignant transformation: experiences of the cooperative GPOH protocols MAKEI 83/86/89/96 | journal = Klinische Padiatrie | volume = 218 | issue = 6 | pages = 303–308 | year = 2006 | pmid = 17080331 | doi = 10.1055/s-2006-942272 | s2cid = 260569521 }}</ref> five carcinoma, two ], and two embryonal carcinoma (here, these last are classified among germ cell tumors). | |||
| ==Complications== | |||
| ==== Extraspinal ependymoma ==== | |||
| Teratomas are not dangerous for the fetus unless there is either a ] or a large amount of blood flow through the tumor (known as ''vascular steal''). The mass effect frequently consists of obstruction of normal passage of fluids from surrounding organs. The vascular steal can place a strain on the growing heart of the fetus, even resulting in heart failure, and thus must be monitored by fetal ]. | |||
| Extraspinal ], usually considered to be a glioma (a type of nongerm cell tumor), may be an unusual form of mature teratoma.<ref>{{cite journal | vauthors = Aktuğ T, Hakgüder G, Sarioğlu S, Akgür FM, Olguner M, Pabuçcuoğlu U | title = Sacrococcygeal extraspinal ependymomas: the role of coccygectomy | journal = Journal of Pediatric Surgery | volume = 35 | issue = 3 | pages = 515–518 | date = March 2000 | pmid = 10726703 | doi = 10.1016/S0022-3468(00)90228-8 }}</ref> | |||
| After surgery, there is a risk of regrowth in place, or in nearby organs<ref></ref> | |||
| ==Treatment== | ==Treatment== | ||
| ===Surgery=== | ===Surgery=== | ||
| The treatment of choice is complete surgical removal ( |
The treatment of choice is complete surgical removal (''i.e.,'' complete resection).<ref>{{cite journal | vauthors = Tapper D, Lack EE | title = Teratomas in infancy and childhood. A 54-year experience at the Children's Hospital Medical Center | journal = Annals of Surgery | volume = 198 | issue = 3 | pages = 398–410 | date = September 1983 | pmid = 6684416 | pmc = 1353316 | doi = 10.1097/00000658-198309000-00016 }}</ref><ref>{{cite journal | vauthors = Göbel U, Schneider DT, Calaminus G, Haas RJ, Schmidt P, Harms D | title = Germ-cell tumors in childhood and adolescence. GPOH MAKEI and the MAHO study groups | journal = Annals of Oncology | volume = 11 | issue = 3 | pages = 263–271 | date = March 2000 | pmid = 10811491 | doi = 10.1023/a:1008360523160 | doi-access = free }}</ref> Teratomas are normally well-encapsulated and noninvasive of surrounding tissues, hence they are relatively easy to resect from surrounding tissues. Exceptions include teratomas in the brain, and very large, complex teratomas that have pushed into and become interlaced with adjacent muscles and other structures. | ||
| Prevention of recurrence does not require ''en bloc'' resection of surrounding tissues. | Prevention of recurrence does not require ''en bloc'' resection of surrounding tissues. | ||
| ===Chemotherapy=== | ===Chemotherapy=== | ||
| For malignant teratomas, usually, surgery is followed by chemotherapy. |
For malignant teratomas, usually, surgery is followed by chemotherapy. | ||
| Teratomas that are in surgically inaccessible locations, or are very complex, or are likely to be malignant (due to late discovery and/or treatment) sometimes are treated first with chemotherapy. | Teratomas that are in surgically inaccessible locations, or are very complex, or are likely to be malignant (due to late discovery and/or treatment) sometimes are treated first with chemotherapy. {{citation needed |date=February 2016}} | ||
| ===Clinical trials=== | |||
| {{globalize|date=June 2007}} | |||
| There are now (2007) two ] in progress that address ], both of which include teratomas.<ref></ref><ref></ref> | |||
| ===Follow-up=== | ===Follow-up=== | ||
| Although often described as benign, a teratoma does have malignant potential. A UK study of 351 infants and children diagnosed with "benign" teratoma reported 227 with MT, 124 with IT. Five years after surgery, event-free survival was 92.2% and 85.9%, respectively, and overall survival was 99% and 95.1%.<ref name="pmid18541896">{{cite journal | vauthors = Mann JR, Gray ES, Thornton C, Raafat F, Robinson K, Collins GS, Gornall P, Huddart SN, Hale JP, Oakhill A | display-authors = 6 | title = Mature and immature extracranial teratomas in children: the UK Children's Cancer Study Group Experience | journal = Journal of Clinical Oncology | volume = 26 | issue = 21 | pages = 3590–3597 | date = July 2008 | pmid = 18541896 | doi = 10.1200/JCO.2008.16.0622 | doi-access = free }}</ref> A similar study in Italy reported on 183 infants and children diagnosed with teratoma. At 10 years after surgery, event-free and overall survival were 90.4% and 98%, respectively.<ref name="pmid17333214">{{cite journal | vauthors = Lo Curto M, D'Angelo P, Cecchetto G, Klersy C, Dall'Igna P, Federico A, Siracusa F, Alaggio R, Bernini G, Conte M, De Laurentis T, Di Cataldo A, Inserra A, Santoro N, Tamaro P, Indolfi P | display-authors = 6 | title = Mature and immature teratomas: results of the first paediatric Italian study | journal = Pediatric Surgery International | volume = 23 | issue = 4 | pages = 315–322 | date = April 2007 | pmid = 17333214 | doi = 10.1007/s00383-007-1890-1 | s2cid = 1380993 }}</ref> | |||
| Depending on which tissue(s) it contains, a teratoma may secrete a variety of chemicals with systemic effects. Some teratomas secrete the "pregnancy hormone" ] (βhCG), which can be used in clinical practice to monitor the successful treatment or relapse in patients with a known HCG-secreting teratoma. This hormone is not recommended as a diagnostic marker, because most teratomas do not secrete it. Some teratomas secrete ], in some cases to such a degree that it can lead to clinical ] in the patient. Of special concern is the secretion of ] (AFP); under some circumstances AFP can be used as a diagnostic marker specific for the presence of ] cells within the teratoma. These cells can develop into a frankly malignant tumor known as ] or ]. | Depending on which tissue(s) it contains, a teratoma may secrete a variety of chemicals with systemic effects. Some teratomas secrete the "pregnancy hormone" ] (βhCG), which can be used in clinical practice to monitor the successful treatment or relapse in patients with a known HCG-secreting teratoma. This hormone is not recommended as a diagnostic marker, because most teratomas do not secrete it. Some teratomas secrete ], in some cases to such a degree that it can lead to clinical ] in the patient. Of special concern is the secretion of ] (AFP); under some circumstances, AFP can be used as a diagnostic marker specific for the presence of ] cells within the teratoma. These cells can develop into a frankly malignant tumor known as ] or ]. | ||
| Adequate follow-up requires close observation, involving repeated physical examination, scanning (ultrasound, MRI, or CT), and measurement of AFP and/or βhCG.<ref name="pmid10561269">{{cite journal | vauthors = Marina NM, Cushing B, Giller R, Cohen L, Lauer SJ, Ablin A, Weetman R, Cullen J, Rogers P, Vinocur C, Stolar C, Rescorla F, Hawkins E, Heifetz S, Rao PV, Krailo M, Castleberry RP | display-authors = 6 | title = Complete surgical excision is effective treatment for children with immature teratomas with or without malignant elements: A Pediatric Oncology Group/Children's Cancer Group Intergroup Study | journal = Journal of Clinical Oncology | volume = 17 | issue = 7 | pages = 2137–2143 | date = July 1999 | pmid = 10561269 | doi = 10.1200/JCO.1999.17.7.2137 }}</ref><ref name="pmid10454682">{{cite journal | vauthors = Cushing B, Giller R, Ablin A, Cohen L, Cullen J, Hawkins E, Heifetz SA, Krailo M, Lauer SJ, Marina N, Rao PV, Rescorla F, Vinocur CD, Weetman RM, Castleberry RP | display-authors = 6 | title = Surgical resection alone is effective treatment for ovarian immature teratoma in children and adolescents: a report of the pediatric oncology group and the children's cancer group | journal = American Journal of Obstetrics and Gynecology | volume = 181 | issue = 2 | pages = 353–358 | date = August 1999 | pmid = 10454682 | doi = 10.1016/S0002-9378(99)70561-2 }}</ref> | |||
| ==Epidemiology== | |||
| ==Use in basic research== | |||
| ]s by ] and risk of ], with mature cystic teratoma at bottom and ] at right.<ref>- {{cite journal| vauthors = Vaidya S, Sharma P, KC S, Vaidya SA |title=Spectrum of ovarian tumors in a referral hospital in Nepal|journal=Journal of Pathology of Nepal|volume=4|issue=7|year=2014|pages=539–543|issn=2091-0908|doi=10.3126/jpn.v4i7.10295|doi-access=free}}<br />- Minor adjustment for mature cystic teratomas (0.17 to 2% risk of ovarian cancer): {{cite journal | vauthors = Mandal S, Badhe BA | title = Malignant transformation in a mature teratoma with metastatic deposits in the omentum: a case report | journal = Case Reports in Pathology | volume = 2012 | pages = 568062 | year = 2012 | pmid = 23082264 | pmc = 3469088 | doi = 10.1155/2012/568062 | doi-access = free }}</ref>]] | |||
| Embryonal teratomas most commonly occur in the sacrococcygeal region; ] is the single most common tumor found in newborn humans. | |||
| Of teratomas on the skull sutures, about 50% are found in or adjacent to the ].<ref>{{EMedicine|oph|620|Orbital dermoid cyst}}</ref> Limbal dermoid is a ], not a teratoma. | |||
| In light of the ], teratomas are being looked at as an alternative source for research since they lack the potential to grow into functional human beings. | |||
| Teratoma qualifies as a ], but is not extremely rare. Sacrococcygeal teratoma alone is diagnosed at birth in one out of 40,000 humans. Given the current human population and birth rate, this equals five per day or 1800 per year. Add to that number sacrococcygeal teratomas diagnosed later in life, and teratomas in other locales, and the ] approaches 10,000 new diagnoses of teratoma per year.{{citation needed |date=February 2016}} | |||
| ==References== | |||
| <div class="references-small"> | |||
| <references/> | |||
| </div> | |||
| == |
==Other animals== | ||
| Ovarian teratomas have been reported in ]s,<ref name="pmid15065985">{{cite journal | vauthors = Catone G, Marino G, Mancuso R, Zanghì A | title = Clinicopathological features of an equine ovarian teratoma | journal = Reproduction in Domestic Animals = Zuchthygiene | volume = 39 | issue = 2 | pages = 65–69 | date = April 2004 | pmid = 15065985 | doi = 10.1111/j.1439-0531.2003.00476.x | hdl = 11581/112802 }}</ref> | |||
| ]s,<ref>{{cite web |url=http://www.cnn.com/2016/01/09/us/idaho-deformed-mountain-lion/ |title=Deformed Mountain Lion a mystery |author=Artemis Moshtaghian |date=January 11, 2016 |website= CNN|publisher=Cable News Network }}</ref><ref name="pmid16363331">{{cite journal | vauthors = Lefebvre R, Theoret C, Doré M, Girard C, Laverty S, Vaillancourt D | title = Ovarian teratoma and endometritis in a mare | journal = The Canadian Veterinary Journal | volume = 46 | issue = 11 | pages = 1029–1033 | date = November 2005 | pmid = 16363331 | pmc = 1259148 }}</ref> and canines.<ref>{{cite journal | vauthors = Gruys E, van Dijk JE | title = Four canine ovarian teratomas and a nonovarian feline teratoma | journal = Veterinary Pathology | volume = 13 | issue = 6 | pages = 455–459 | year = 1976 | pmid = 1006958 | doi = 10.1177/030098587601300609 | s2cid = 46250641 }}</ref> Teratomas also occur, rarely, in other species.<ref name="pmid18622858">{{cite journal | vauthors = López RM, Múrcia DB | title = First description of malignant retrobulbar and intracranial teratoma in a lesser kestrel (Falco naumanni) | journal = Avian Pathology | volume = 37 | issue = 4 | pages = 413–414 | date = August 2008 | pmid = 18622858 | doi = 10.1080/03079450802216660 | s2cid = 748134 | doi-access = free }}</ref> | |||
| == Use in stem cell research == | |||
| Tumor pages for locations in which teratoma can occur: | |||
| Pluripotent stem cells including human induced pluripotent stem cells have a unique property of being able to generate teratomas when injected in rodents in the research laboratory.<ref>{{cite journal | vauthors = Gutierrez-Aranda I, Ramos-Mejia V, Bueno C, Munoz-Lopez M, Real PJ, Mácia A, Sanchez L, Ligero G, Garcia-Parez JL, Menendez P | display-authors = 6 | title = Human induced pluripotent stem cells develop teratoma more efficiently and faster than human embryonic stem cells regardless the site of injection | journal = Stem Cells | volume = 28 | issue = 9 | pages = 1568–1570 | date = September 2010 | pmid = 20641038 | pmc = 2996086 | doi = 10.1002/stem.471 }}</ref> The roots of this observation has been attributed to ] of the ].<ref>{{cite web |title=A Stem Cell Legacy: Leroy Stevens |url=https://www.the-scientist.com/news/a-stem-cell-legacy-leroy-stevens-56114 |website=The Scientist Magazine® |language=en}}</ref> In 1970, Stevens noticed that the cell populations that gave rise to teratomas were very similar to the cells of very early embryos. | |||
| *] | |||
| For this reason, the so-called "teratoma assay" is one of the gold-standard validation assays for pluripotent stem cells.<ref>{{Cite web| vauthors = Knoepfler P |date=2021-01-14|title=What is a teratoma? Research & treatment|url=https://ipscell.com/2021/01/what-is-a-teratoma-research-prevention-treatment/|access-date=2021-02-07|website=The Niche|language=en-US}}</ref> Because differentiated human pluripotent stem cells are being developed as the basis for numerous regenerative medicine therapies, there is concern that residual undifferentiated stem cells could lead to teratoma formation in injected patients, and researchers are working to develop methods to address this concern.<ref>{{cite journal | vauthors = Lee MO, Moon SH, Jeong HC, Yi JY, Lee TH, Shim SH, Rhee YH, Lee SH, Oh SJ, Lee MY, Han MJ, Cho YS, Chung HM, Kim KS, Cha HJ | display-authors = 6 | title = Inhibition of pluripotent stem cell-derived teratoma formation by small molecules | journal = Proceedings of the National Academy of Sciences of the United States of America | volume = 110 | issue = 35 | pages = E3281–E3290 | date = August 2013 | pmid = 23918355 | pmc = 3761568 | doi = 10.1073/pnas.1303669110 | doi-access = free | bibcode = 2013PNAS..110E3281L }}</ref> | |||
| *] | |||
| *] | |||
| *] | |||
| *] | |||
| *] | |||
| *] | |||
| *] | |||
| New research has looked at utilizing the human teratoma in chimeric animal studies as a promising platform for modeling multi-lineage human development, pan-tissue functional genetic screening, and tissue engineering.<ref>{{Cite journal |last1=McDonald |first1=Daniella |last2=Wu |first2=Yan |last3=Dailamy |first3=Amir |last4=Tat |first4=Justin |last5=Parekh |first5=Udit |last6=Zhao |first6=Dongxin |last7=Hu |first7=Michael |last8=Tipps |first8=Ann |last9=Zhang |first9=Kun |last10=Mali |first10=Prashant |date=2020-11-25 |title=Defining the Teratoma as a Model for Multi-lineage Human Development |journal=Cell |volume=183 |issue=5 |pages=1402–1419.e18 |doi=10.1016/j.cell.2020.10.018 |issn=1097-4172 |pmc=7704916 |pmid=33152263}}</ref> | |||
| ==External links== | |||
| == References == | |||
| ===Technical information=== | |||
| {{reflist}} | |||
| * | |||
| * (also ) | |||
| * article in the ] | |||
| {{NCI-cancer-dict}} | |||
| == External links == | |||
| {{Tumors}} | |||
| {{Wikiquote}} | |||
| {{Soft tissue tumors and sarcomas}} | |||
| {{Commons category|Teratomas}} | |||
| {{Endocrine pathology|state=collapsed}} | |||
| {{wiktionary|teratoma}} | |||
| *humpath pathology images {{Webarchive|url=https://web.archive.org/web/20170901031726/http://www.humpath.com/spip.php?page=article&id_article=2657 |date=2017-09-01 }} (Teratomas), {{Webarchive|url=https://web.archive.org/web/20170901031732/http://www.humpath.com/spip.php?page=article&id_article=4541 |date=2017-09-01 }} (Mature teratoma), {{Webarchive|url=https://web.archive.org/web/20170901031656/http://www.humpath.com/spip.php?page=article&id_article=5350 |date=2017-09-01 }} (Immature teratoma) | |||
| *{{EMedicine|med|2248|cystic teratoma}} (also ) | |||
| {{Medical resources | |||
| | DiseasesDB = 3604 | |||
| | ICD10 = {{ICD10|C22.7}}, {{ICD10|C56}}, {{ICD10|C62}} (] C62.930), {{ICD10|D13.4}}, {{ICD10|D27}}, {{ICD10|D29.2}}, {{ICD10|O33.7}}, {{ICD10|O66.3}} | |||
| | ICD9 = | |||
| | ICDO = 9080 | |||
| | OMIM = | |||
| | MedlinePlus = | |||
| | eMedicineSubj = med | |||
| | eMedicineTopic = 3449 | |||
| | MeshID = D013724 | |||
| | diseasesDB_mult = {{DiseasesDB2|12952}} {{DiseasesDB2|12966}} | |||
| | SNOMED CT = 36591000119102 | |||
| }} | |||
| {{Germ cell tumors}} | |||
| {{Skin tumors, dermis}} | |||
| {{Genital neoplasia}} | |||
| {{Male genital neoplasia}} | |||
| {{Authority control}} | |||
| ] | ] | ||
| ] | ] | ||
| ] | ] | ||
| ] | ] | ||
| ] | ] | ||
| ] | ] | ||
| ] | ] | ||
| ] | ] | ||
| ] | ] | ||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
| ] | |||
Latest revision as of 08:08, 13 November 2024
Type of germ cell tumor Medical condition| Teratoma | |
|---|---|
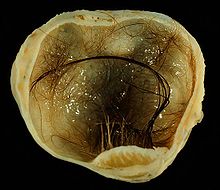 | |
| A small (4 cm) dermoid cyst of an ovary, discovered during cesarean section | |
| Specialty | Gynecology, oncology |
| Symptoms | Minimal, painless lump |
| Complications | Ovarian torsion, testicular torsion, hydrops fetalis |
| Types | Mature, immature |
| Causes | Unknown |
| Diagnostic method | Tissue biopsy |
| Differential diagnosis | Lipoma, dermoid, myelomeningocele |
| Treatment | Surgery, chemotherapy |
| Frequency | 1 in 30,000 newborns (coccyx) |
A teratoma is a tumor made up of several types of tissue, such as hair, muscle, teeth, or bone. Teratomata typically form in the tailbone (where it is known as a sacrococcygeal teratoma), ovary, or testicle.
Symptoms
Symptoms may be minimal if the tumor is small. A testicular teratoma may present as a painless lump. Complications may include ovarian torsion, testicular torsion, or hydrops fetalis.
They are a type of germ cell tumor (a tumor that begins in the cells that give rise to sperm or eggs). They are divided into two types: mature and immature. Mature teratomas include dermoid cysts and are generally benign. Immature teratomas may be cancerous. Most ovarian teratomas are mature. In adults, testicular teratomas are generally cancerous. Definitive diagnosis is based on a tissue biopsy.
Treatment of coccyx, testicular, and ovarian teratomas is generally by surgery. Testicular and immature ovarian teratomas are also frequently treated with chemotherapy.
Teratomas occur in the coccyx in about one in 30,000 newborns, making them one of the most common tumors in this age group. Females are affected more often than males. Ovarian teratomas represent about a quarter of ovarian tumors and are typically noticed during middle age. Testicular teratomas represent almost half of testicular cancers. They can occur in both children and adults. The term comes from the Greek word for "monster" plus the "-oma" suffix used for tumors.
Teratomas can cause an autoimmune illness called Anti-NMDA receptor encephalitis. In this condition, the teratomas may contain B cells with NMDA-receptor specificities.
After teratoma removal surgery, a risk exists of regrowth in place, or in nearby organs.
Types
Mature teratoma


A mature teratoma is a grade 0 teratoma. They are highly variable in form and histology, and may be solid, cystic, or a combination of the two. A mature teratoma often contains several different types of tissue such as skin, muscle, and bone. Skin may surround a cyst and grow abundant hair (see: § Dermoid cyst). Mature teratomas generally are benign, with 0.17–2% of mature cystic teratomas becoming malignant.
Immature teratoma
Immature teratoma is the malignant counterpart of the mature teratoma and contains immature tissues which typically show primitive or embryonal neuroectodermal histopathology. Immature teratoma has one of the lowest rates of somatic mutation of any tumor type and results from one of five mechanisms of meiotic failure.
Gliomatosis peritoneii
Gliomatosis peritoneii, which presents as a deposition of mature glial cells in the peritoneum, is almost exclusively seen in conjunction with cases of ovarian teratoma. Through genetic studies of exome sequence, it was found that gliomatosis is genetically identical to the parent ovarian tumor and developed from cells that disseminate from the ovarian teratoma.
Dermoid cyst
A dermoid cyst is a mature cystic teratoma containing hair (sometimes very abundant) and other structures characteristic of normal skin and other tissues derived from the ectoderm. The term is most often applied to teratoma on the skull sutures and in the ovaries of females.
Fetus in fetu and fetiform teratoma
Fetus in fetu and fetiform teratoma are rare forms of mature teratomas that include one or more components resembling a malformed fetus. Both forms may contain or appear to contain complete organ systems, even major body parts, such as a torso or limbs. Fetus in fetu differs from fetiform teratoma in having an apparent spine and bilateral symmetry.
Most authorities agree that fetiform teratomas are highly developed mature teratomas; the natural history of fetus in fetu is controversial. It has been noted that fetiform teratoma is reported more often (by gynecologists) in ovarian teratomas, and fetus in fetu is reported more often (by general surgeons) in retroperitoneal teratomas. Fetus in fetu has often been interpreted as a fetus growing within its twin. As such, this interpretation assumes a special complication of twinning, one of several grouped under the term parasitic twin. In many cases, the fetus in fetu is reported to occupy a fluid-filled cyst within a mature teratoma. Cysts within mature teratomas may have partially-developed organ systems: reports include cases of partial cranial bones, long bones and a rudimentary, beating heart.
Regardless of whether fetus in fetu and fetiform teratoma are one entity or two, they are distinct from and not to be confused with ectopic pregnancy.
Struma ovarii
Main article: Struma ovariiA struma ovarii (also known as goitre of the ovary or ovarian goiter) is a rare form of mature teratoma that contains mostly thyroid tissue.
Epignathus
Main article: EpignathusEpignathus is a rare teratoma originating in the oropharyngeal area that occurs in utero. It presents with a mass protruding from the mouth at birth. Untreated, breathing is impossible. An EXIT procedure is the recommended initial treatment.
Fetal Teratomas
Teratomas may be found in babies, children, and adults. Teratomas of embryonal origin are most often found in babies at birth, in young children, and, since the advent of ultrasound imaging, in fetuses.
The most diagnosed fetal teratomas are sacrococcygeal teratoma (Altman types I, II, and III) and cervical (neck) teratoma. Because these teratomas project from the fetal body into the surrounding amniotic fluid, they can be seen during routine prenatal ultrasound exams. Teratomas within the fetal body are less easily seen with ultrasound; for these, MRI of the pregnant uterus is more informative.
Complications
Teratomas are not dangerous for the fetus unless either a mass effect occurs or a large amount of blood flows through the tumor (known as vascular steal). The mass effect frequently consists of obstruction of normal passage of fluids from surrounding organs. The vascular steal can place a strain on the growing heart of the fetus, even resulting in heart failure, thus must be monitored by fetal echocardiography.
Pathophysiology
Main article: Germ cell tumorTeratomas belong to a class of tumors known as nonseminomatous germ cell tumor. All tumors of this class are the result of abnormal development of pluripotent cells: germ cells and embryonal cells. Teratomas of embryonic origin are congenital; teratomas of germ cell origin may or may not be congenital. The kind of pluripotent cell appears to be unimportant, apart from constraining the location of the teratoma in the body.
Teratomas derived from germ cells occur in the testicle and ovaries. Teratomas derived from embryonic cells usually occur on the subject's midline: in the brain, elsewhere in the skull, in the nose, in the tongue, under the tongue, and in the neck (cervical teratoma), mediastinum, retroperitoneum, and attached to the coccyx. Teratomas may also occur elsewhere: very rarely in solid organs (most notably the heart and liver) and hollow organs (such as the stomach and bladder), and more commonly on the skull sutures.
Teratoma rarely include more complicated body parts such as teeth, brain matter, eyes, or torso.
Hypotheses of origin
Concerning the origin of teratomas, numerous hypotheses exist. These hypotheses are not to be confused with the unrelated hypothesis that fetus in fetu (see below) is not a teratoma at all, but rather a parasitic twin.
Diagnosis


Teratomas are thought to originate in utero, so can be considered congenital tumors. Many teratomas are not diagnosed until much later in childhood or in adulthood. Large tumors are more likely to be diagnosed early on. Sacrococcygeal and cervical teratomas are often detected by prenatal ultrasound. Additional diagnostic methods may include prenatal magnetic resonance imaging. In rare circumstances, the tumor is so large that the fetus may be damaged or die. In the case of large sacrococcygeal teratomas, a significant portion of the fetus' blood flow is redirected toward the teratoma (a phenomenon called steal syndrome), causing heart failure, or hydrops, of the fetus. In certain cases, fetal surgery may be indicated.
Beyond the newborn period, symptoms of a teratoma depend on its location and organ of origin. Ovarian teratomas often present with abdominal or pelvic pain, caused by torsion of the ovary or irritation of its ligaments. A recently discovered condition where ovarian teratomas cause encephalitis associated with antibodies against the N-methyl-D-aspartate receptor antibody (NMDAR) - often referred to as "anti-NMDA receptor encephalitis", was identified as a serious complication. Patients develop a multistage illness that progresses from psychosis, memory deficits, seizures, and language disintegration into a state of unresponsiveness with catatonic features often associated with abnormal movements, and autonomic and breathing instability. Testicular teratomas present as a palpable mass in the testis; mediastinal teratomas often cause compression of the lungs or the airways and may present with chest pain and/or respiratory symptoms.
Some teratomas contain yolk sac elements, which secrete alpha-fetoprotein. Its detection may help to confirm the diagnosis and is often used as a marker for recurrence or treatment efficacy, but is rarely the method of initial diagnosis. (Maternal serum alpha-fetoprotein is a useful screening test for other fetal conditions, including Down syndrome, spina bifida, and abdominal wall defects such as gastroschisis.)
Classification
Regardless of location in the body, a teratoma is classified according to a cancer staging system. This indicates whether chemotherapy or radiation therapy may be needed in addition to surgery. Teratomas commonly are classified using the Gonzalez-Crussi grading system: 0 or mature (benign); 1 or immature, probably benign; 2 or immature, possibly malignant (cancerous); and 3 or frankly malignant. If frankly malignant, the tumor is a cancer for which additional cancer staging applies.
Teratomas are also classified by their content; a solid teratoma contains only tissues (perhaps including more complex structures); a cystic teratoma contains only pockets of fluid or semifluid such as cerebrospinal fluid, sebum, or fat; a mixed teratoma contains both solid and cystic parts. Cystic teratomas usually are grade 0 and, conversely, grade 0 teratomas usually are cystic.
Grades 0, 1, and 2 pure teratomas have the potential to become malignant (grade 3), and malignant pure teratomas have the potential to metastasize. These rare forms of teratoma with malignant transformation may contain elements of somatic (not germ cell) malignancy such as leukemia, carcinoma, or sarcoma. A teratoma may contain elements of other germ cell tumors, in which case it is not a pure teratoma, but rather is a mixed germ cell tumor and is malignant. In infants and young children, these elements usually are endodermal sinus tumor, followed by choriocarcinoma. Finally, a teratoma can be pure and not malignant yet highly aggressive; this is exemplified by growing teratoma syndrome, in which chemotherapy eliminates the malignant elements of a mixed tumor, leaving pure teratoma, which paradoxically begins to grow very rapidly.
Malignant transformation
A "benign" grade 0 (mature) teratoma nonetheless has a risk of malignancy. Recurrence with malignant endodermal sinus tumor has been reported in cases of formerly benign mature teratoma, even in fetiform teratoma and fetus in fetu. Squamous cell carcinoma has been found in a mature cystic teratoma at the time of initial surgery. A grade 1 immature teratoma that appears to be benign (e.g., because AFP is not elevated) has a much higher risk of malignancy, and requires adequate follow-up. This grade of teratoma also may be difficult to diagnose correctly. It can be confused with other small round cell neoplasms such as neuroblastoma, small cell carcinoma of hypercalcemic type, primitive neuroectodermal tumor, Wilm's tumor, desmoplastic small round cell tumor, and non-Hodgkin lymphoma.
A teratoma with malignant transformation is a very rare form of teratoma that may contain elements of somatic malignant tumors such as leukemia, carcinoma, or sarcoma. Of 641 children with pure teratoma, nine developed TMT: five carcinoma, two glioma, and two embryonal carcinoma (here, these last are classified among germ cell tumors).
Extraspinal ependymoma
Extraspinal ependymoma, usually considered to be a glioma (a type of nongerm cell tumor), may be an unusual form of mature teratoma.
Treatment
Surgery
The treatment of choice is complete surgical removal (i.e., complete resection). Teratomas are normally well-encapsulated and noninvasive of surrounding tissues, hence they are relatively easy to resect from surrounding tissues. Exceptions include teratomas in the brain, and very large, complex teratomas that have pushed into and become interlaced with adjacent muscles and other structures.
Prevention of recurrence does not require en bloc resection of surrounding tissues.
Chemotherapy
For malignant teratomas, usually, surgery is followed by chemotherapy.
Teratomas that are in surgically inaccessible locations, or are very complex, or are likely to be malignant (due to late discovery and/or treatment) sometimes are treated first with chemotherapy.
Follow-up
Although often described as benign, a teratoma does have malignant potential. A UK study of 351 infants and children diagnosed with "benign" teratoma reported 227 with MT, 124 with IT. Five years after surgery, event-free survival was 92.2% and 85.9%, respectively, and overall survival was 99% and 95.1%. A similar study in Italy reported on 183 infants and children diagnosed with teratoma. At 10 years after surgery, event-free and overall survival were 90.4% and 98%, respectively.
Depending on which tissue(s) it contains, a teratoma may secrete a variety of chemicals with systemic effects. Some teratomas secrete the "pregnancy hormone" human chorionic gonadotropin (βhCG), which can be used in clinical practice to monitor the successful treatment or relapse in patients with a known HCG-secreting teratoma. This hormone is not recommended as a diagnostic marker, because most teratomas do not secrete it. Some teratomas secrete thyroxine, in some cases to such a degree that it can lead to clinical hyperthyroidism in the patient. Of special concern is the secretion of alpha-fetoprotein (AFP); under some circumstances, AFP can be used as a diagnostic marker specific for the presence of yolk sac cells within the teratoma. These cells can develop into a frankly malignant tumor known as yolk sac tumor or endodermal sinus tumor.
Adequate follow-up requires close observation, involving repeated physical examination, scanning (ultrasound, MRI, or CT), and measurement of AFP and/or βhCG.
Epidemiology

Embryonal teratomas most commonly occur in the sacrococcygeal region; sacrococcygeal teratoma is the single most common tumor found in newborn humans.
Of teratomas on the skull sutures, about 50% are found in or adjacent to the orbit. Limbal dermoid is a choristoma, not a teratoma.
Teratoma qualifies as a rare disease, but is not extremely rare. Sacrococcygeal teratoma alone is diagnosed at birth in one out of 40,000 humans. Given the current human population and birth rate, this equals five per day or 1800 per year. Add to that number sacrococcygeal teratomas diagnosed later in life, and teratomas in other locales, and the incidence approaches 10,000 new diagnoses of teratoma per year.
Other animals
Ovarian teratomas have been reported in mares, mountain lions, and canines. Teratomas also occur, rarely, in other species.
Use in stem cell research
Pluripotent stem cells including human induced pluripotent stem cells have a unique property of being able to generate teratomas when injected in rodents in the research laboratory. The roots of this observation has been attributed to Leroy Stevens of the Jackson Laboratory. In 1970, Stevens noticed that the cell populations that gave rise to teratomas were very similar to the cells of very early embryos. For this reason, the so-called "teratoma assay" is one of the gold-standard validation assays for pluripotent stem cells. Because differentiated human pluripotent stem cells are being developed as the basis for numerous regenerative medicine therapies, there is concern that residual undifferentiated stem cells could lead to teratoma formation in injected patients, and researchers are working to develop methods to address this concern.
New research has looked at utilizing the human teratoma in chimeric animal studies as a promising platform for modeling multi-lineage human development, pan-tissue functional genetic screening, and tissue engineering.
References
- ^ Raja SG (2007). Access to Surgery: 500 single best answer questions in general and systematic pathology. PasTest Ltd. p. 508. ISBN 9781905635368.
- ^ "Sacrococcygeal Teratoma". NORD (National Organization for Rare Disorders). 2007. Retrieved 20 December 2017.
- ^ Millet I, Perrochia H, Pages-Bouic E, Curros-Doyon F, Rathat G, Taourel P (2014). "CT and MR of Benign Ovarian Germ Cell Tumours". In Saba L, Acharya UR, Guerriero S, Suri JS (eds.). Ovarian Neoplasm Imaging. Springer Science & Business Media. p. 165. ISBN 9781461486336.
- ^ "NCI Dictionary of Cancer Terms". National Cancer Institute. 2011-02-02. Retrieved 20 December 2017.
- ^ Davies M, Inglis G, Jardine L, Koorts P (2012). Antenatal Consults: A Guide for Neonatologists and Paediatricians - E-Book. Elsevier Health Sciences. p. 298. ISBN 978-0729581080.
- ^ Price P, Sikora K, Illidge T (2008). Treatment of Cancer (Fifth ed.). CRC Press. p. 713. ISBN 9780340912218.
- ^ Corton MM, Leveno KJ, Bloom SL, Hoffman BL (2014). Williams Obstetrics 24/E (EBOOK). McGraw Hill Professional. p. Chapter 16. ISBN 9780071798945.
- ^ "Mature teratoma". National Cancer Institute. 2011-02-02. Retrieved 20 December 2017.
- Noor MR, Hseon TE, Jeffrey LJ, eds. (2014). "Ovarian Germ Cell Tumors". Gynaecologic Cancer: A Handbook for Students and Practitioners. CRC Press. p. 446. ISBN 9789814463065.
- ^ Falcone T, Hurd WW (2007). Clinical Reproductive Medicine and Surgery. Elsevier Health Sciences. p. 749. ISBN 978-0323033091.
- Oyasu R, Yang XJ, Yoshida O (2009). Questions in Daily Urologic Practice: Updates for Urologists and Diagnostic Pathologists. Springer Science & Business Media. p. 253. ISBN 9784431728191.
- Hillard PJ, Hillard PA (2008). The 5-minute Obstetrics and Gynecology Consult. Lippincott Williams & Wilkins. p. 140. ISBN 9780781769426.
- Hart I, Newton RW (2012). Endocrinology. Springer Science & Business Media. p. 157. ISBN 9789401092982.
- McDougal WS, Wein AJ, Kavoussi LR, Partin AW, Peters CA, Ramchandani P (2011). Campbell-Walsh Urology (10th ed.). Elsevier Health Sciences. p. 663. ISBN 978-1455723171.
- Chang AE, Ganz PA, Hayes DF, Kinsella T, Pass HI, Schiller JH, Stone RM, Strecher V (2007). Oncology: An Evidence-Based Approach. Springer Science & Business Media. p. 848. ISBN 9780387310565.
- Makuch M, Wilson R, Al-Diwani A, Varley J, Kienzler AK, Taylor J, et al. (March 2018). "N-methyl-D-aspartate receptor antibody production from germinal center reactions: Therapeutic implications". Annals of Neurology. 83 (3): 553–561. doi:10.1002/ana.25173. PMC 5925521. PMID 29406578.
- Choi KW, Jeon WJ, Chae HB, Park SM, Youn SJ, Shin HM, et al. (September 2003). "[A recurred case of a mature ovarian teratoma presenting as a rectal mass]" (PDF). The Korean Journal of Gastroenterology = Taehan Sohwagi Hakhoe Chi (in Korean). 42 (3): 242–245. PMID 14532748.
- Mandal S, Badhe BA (2012). "Malignant transformation in a mature teratoma with metastatic deposits in the omentum: a case report". Case Reports in Pathology. 2012: 568062. doi:10.1155/2012/568062. PMC 3469088. PMID 23082264.
- ^ Heskett MB, Sanborn JZ, Boniface C, Goode B, Chapman J, Garg K, et al. (June 2020). "Multiregion exome sequencing of ovarian immature teratomas reveals 2N near-diploid genomes, paucity of somatic mutations, and extensive allelic imbalances shared across mature, immature, and disseminated components". Modern Pathology. 33 (6): 1193–1206. doi:10.1038/s41379-019-0446-y. PMC 7286805. PMID 31911616.
- ^ Gonzalez-Crussi F (1982) Extragonadal Teratomas. Atlas of Tumor Pathology, Second Series, Fascicle 18. Armed Forces Institute of Pathology, Washington D.C.
- Abbott TM, Hermann WJ, Scully RE (1984). "Ovarian fetiform teratoma (homunculus) in a 9-year-old girl". International Journal of Gynecological Pathology. 2 (4): 392–402. doi:10.1097/00004347-198404000-00007. PMID 6724790.
- Saito K, Katsumata Y, Hirabuki T, Kato K, Yamanaka M (2007). "Fetus-in-fetu: parasite or neoplasm? A study of two cases". Fetal Diagnosis and Therapy. 22 (5): 383–388. doi:10.1159/000103301. PMID 17556829. S2CID 57099054.
- Kajbafzadeh AM, Baharnoori M (October 2006). "Fetus in fetu". The Canadian Journal of Urology. 13 (5): 3277–3278. PMID 17076951.
- Chua JH, Chui CH, Sai Prasad TR, Jabcobsen AS, Meenakshi A, Hwang WS (November 2005). "Fetus-in-fetu in the pelvis: report of a case and literature review" (PDF). Annals of the Academy of Medicine, Singapore. 34 (10): 646–649. PMID 16382253.
- Lee YH, Kim SG, Choi SH, Kim IS, Kim SH (December 2003). "Ovarian mature cystic teratoma containing homunculus: a case report" (PDF). Journal of Korean Medical Science. 18 (6): 905–907. doi:10.3346/jkms.2003.18.6.905. PMC 3055135. PMID 14676454. Archived from the original (PDF) on 2011-07-22.
- Kazez A, Ozercan IH, Erol FS, Faik Ozveren M, Parmaksiz E (August 2002). "Sacrococcygeal heart: a very rare differentiation in teratoma". European Journal of Pediatric Surgery. 12 (4): 278–280. doi:10.1055/s-2002-34483. PMID 12369008. S2CID 260136953.
- Frysak Z, Schovanek J, Halenka M, Metelkova I, Duskova M, Karasek D (2016). "Ovarian Goiter as a Rare Cause of Hyperthyroidism". Acta Endocrinologica. 12 (3): 335–338. doi:10.4183/aeb.2016.335. PMC 6535264. PMID 31149110.
- Danzer E, Hubbard AM, Hedrick HL, Johnson MP, Wilson RD, Howell LJ, et al. (October 2006). "Diagnosis and characterization of fetal sacrococcygeal teratoma with prenatal MRI". AJR. American Journal of Roentgenology. 187 (4): W350 – W356. doi:10.2214/AJR.05.0152. PMID 16985105.
- Kocaoglu M, Frush DP (2006). "Pediatric presacral masses". Radiographics. 26 (3): 833–857. doi:10.1148/rg.263055102. PMID 16702458.
- Shintaku M, Sakuma T, Ohbayashi C, Maruo M (April 2017). "Well-formed cerebellum and brainstem-like structures in a mature ovarian teratoma: Neuropathological observations". Neuropathology. 37 (2): 122–128. doi:10.1111/neup.12360. PMID 28042664. S2CID 25588284.
- Chi JG, Lee YS, Park YS, Chang KY (July 1984). "Fetus-in-fetu: report of a case". American Journal of Clinical Pathology. 82 (1): 115–119. doi:10.1093/ajcp/82.1.115. PMID 6540049.
- Sergi C, Ehemann V, Beedgen B, Linderkamp O, Otto HF (1999). "Huge fetal sacrococcygeal teratoma with a completely formed eye and intratumoral DNA ploidy heterogeneity". Pediatric and Developmental Pathology. 2 (1): 50–57. doi:10.1007/s100249900089. PMID 9841706. S2CID 22847474.
- Arlikar JD, Mane SB, Dhende NP, Sanghavi Y, Valand AG, Butale PR (March 2009). "Fetus in fetu: two case reports and review of literature". Pediatric Surgery International. 25 (3): 289–292. doi:10.1007/s00383-009-2328-8. PMID 19184054. S2CID 11210782.
- Dalmau J, Lancaster E, Martinez-Hernandez E, Rosenfeld MR, Balice-Gordon R (January 2011). "Clinical experience and laboratory investigations in patients with anti-NMDAR encephalitis". The Lancet. Neurology. 10 (1): 63–74. doi:10.1016/S1474-4422(10)70253-2. PMC 3158385. PMID 21163445.
- ^ Harms D, Zahn S, Göbel U, Schneider DT (2006). "Pathology and molecular biology of teratomas in childhood and adolescence". Klinische Padiatrie. 218 (6): 296–302. doi:10.1055/s-2006-942271. PMID 17080330. S2CID 20627932.
- Scavuzzo A, Santana Ríos ZA, Noverón NR, Jimenez Ríos MA (2014). "Growing teratoma syndrome". Case Reports in Urology. 2014: 139425. doi:10.1155/2014/139425. PMC 4150507. PMID 25197607.
- Ohno Y, Kanematsu T (October 1998). "An endodermal sinus tumor arising from a mature cystic teratoma in the retroperitoneum in a child: is a mature teratoma a premalignant condition?". Human Pathology. 29 (10): 1167–1169. doi:10.1016/S0046-8177(98)90432-4. PMID 9781660.
- Utsuki S, Oka H, Sagiuchi T, Shimizu S, Suzuki S, Fujii K (June 2007). "Malignant transformation of intracranial mature teratoma to yolk sac tumor after late relapse. Case report". Journal of Neurosurgery. 106 (6): 1067–1069. doi:10.3171/jns.2007.106.6.1067. PMID 17564180. S2CID 23864999.
- Chen YH, Chang CH, Chen KC, Diau GY, Loh IW, Chu CC (May 2007). "Malignant transformation of a well-organized sacrococcygeal fetiform teratoma in a newborn male". Journal of the Formosan Medical Association = Taiwan Yi Zhi. 106 (5): 400–402. doi:10.1016/S0929-6646(09)60326-0. PMID 17561476.
- Hopkins KL, Dickson PK, Ball TI, Ricketts RR, O'Shea PA, Abramowsky CR (October 1997). "Fetus-in-fetu with malignant recurrence". Journal of Pediatric Surgery. 32 (10): 1476–1479. doi:10.1016/S0022-3468(97)90567-4. PMID 9349774.
- Arioz DT, Tokyol C, Sahin FK, Koker G, Yilmaz S, Yilmazer M, Ozalp S (2008). "Squamous cell carcinoma arising in a mature cystic teratoma of the ovary in young patient with elevated carbohydrate antigen 19-9". European Journal of Gynaecological Oncology. 29 (3): 282–284. PMID 18592797.
- Muscatello L, Giudice M, Feltri M (November 2005). "Malignant cervical teratoma: report of a case in a newborn". European Archives of Oto-Rhino-Laryngology. 262 (11): 899–904. doi:10.1007/s00405-005-0917-2. PMID 15895292. S2CID 11556991.
- Ukiyama E, Endo M, Yoshida F, Tezuka T, Kudo K, Sato S, et al. (July 2005). "Recurrent yolk sac tumor following resection of a neonatal immature gastric teratoma". Pediatric Surgery International. 21 (7): 585–588. doi:10.1007/s00383-005-1404-y. PMID 15928937. S2CID 40147917.
- Bilik R, Shandling B, Pope M, Thorner P, Weitzman S, Ein SH (September 1993). "Malignant benign neonatal sacrococcygeal teratoma". Journal of Pediatric Surgery. 28 (9): 1158–1160. doi:10.1016/0022-3468(93)90154-D. PMID 7508500.
- Hawkins E, Issacs H, Cushing B, Rogers P (November 1993). "Occult malignancy in neonatal sacrococcygeal teratomas. A report from a Combined Pediatric Oncology Group and Children's Cancer Group study". The American Journal of Pediatric Hematology/Oncology. 15 (4): 406–409. PMID 7692755.
- Ramalingam P, Teague D, Reid-Nicholson M (August 2008). "Imprint cytology of high-grade immature ovarian teratoma: a case report, literature review, and distinction from other ovarian small round cell tumors". Diagnostic Cytopathology. 36 (8): 595–599. doi:10.1002/dc.20849. PMID 18618728. S2CID 21066080.
- Biskup W, Calaminus G, Schneider DT, Leuschner I, Göbel U (2006). "Teratoma with malignant transformation: experiences of the cooperative GPOH protocols MAKEI 83/86/89/96". Klinische Padiatrie. 218 (6): 303–308. doi:10.1055/s-2006-942272. PMID 17080331. S2CID 260569521.
- Aktuğ T, Hakgüder G, Sarioğlu S, Akgür FM, Olguner M, Pabuçcuoğlu U (March 2000). "Sacrococcygeal extraspinal ependymomas: the role of coccygectomy". Journal of Pediatric Surgery. 35 (3): 515–518. doi:10.1016/S0022-3468(00)90228-8. PMID 10726703.
- Tapper D, Lack EE (September 1983). "Teratomas in infancy and childhood. A 54-year experience at the Children's Hospital Medical Center". Annals of Surgery. 198 (3): 398–410. doi:10.1097/00000658-198309000-00016. PMC 1353316. PMID 6684416.
- Göbel U, Schneider DT, Calaminus G, Haas RJ, Schmidt P, Harms D (March 2000). "Germ-cell tumors in childhood and adolescence. GPOH MAKEI and the MAHO study groups". Annals of Oncology. 11 (3): 263–271. doi:10.1023/a:1008360523160. PMID 10811491.
- Mann JR, Gray ES, Thornton C, Raafat F, Robinson K, Collins GS, et al. (July 2008). "Mature and immature extracranial teratomas in children: the UK Children's Cancer Study Group Experience". Journal of Clinical Oncology. 26 (21): 3590–3597. doi:10.1200/JCO.2008.16.0622. PMID 18541896.
- Lo Curto M, D'Angelo P, Cecchetto G, Klersy C, Dall'Igna P, Federico A, et al. (April 2007). "Mature and immature teratomas: results of the first paediatric Italian study". Pediatric Surgery International. 23 (4): 315–322. doi:10.1007/s00383-007-1890-1. PMID 17333214. S2CID 1380993.
- Marina NM, Cushing B, Giller R, Cohen L, Lauer SJ, Ablin A, et al. (July 1999). "Complete surgical excision is effective treatment for children with immature teratomas with or without malignant elements: A Pediatric Oncology Group/Children's Cancer Group Intergroup Study". Journal of Clinical Oncology. 17 (7): 2137–2143. doi:10.1200/JCO.1999.17.7.2137. PMID 10561269.
- Cushing B, Giller R, Ablin A, Cohen L, Cullen J, Hawkins E, et al. (August 1999). "Surgical resection alone is effective treatment for ovarian immature teratoma in children and adolescents: a report of the pediatric oncology group and the children's cancer group". American Journal of Obstetrics and Gynecology. 181 (2): 353–358. doi:10.1016/S0002-9378(99)70561-2. PMID 10454682.
- - Vaidya S, Sharma P, KC S, Vaidya SA (2014). "Spectrum of ovarian tumors in a referral hospital in Nepal". Journal of Pathology of Nepal. 4 (7): 539–543. doi:10.3126/jpn.v4i7.10295. ISSN 2091-0908.
- Minor adjustment for mature cystic teratomas (0.17 to 2% risk of ovarian cancer): Mandal S, Badhe BA (2012). "Malignant transformation in a mature teratoma with metastatic deposits in the omentum: a case report". Case Reports in Pathology. 2012: 568062. doi:10.1155/2012/568062. PMC 3469088. PMID 23082264. - Orbital dermoid cyst at eMedicine
- Catone G, Marino G, Mancuso R, Zanghì A (April 2004). "Clinicopathological features of an equine ovarian teratoma". Reproduction in Domestic Animals = Zuchthygiene. 39 (2): 65–69. doi:10.1111/j.1439-0531.2003.00476.x. hdl:11581/112802. PMID 15065985.
- Artemis Moshtaghian (January 11, 2016). "Deformed Mountain Lion a mystery". CNN. Cable News Network.
- Lefebvre R, Theoret C, Doré M, Girard C, Laverty S, Vaillancourt D (November 2005). "Ovarian teratoma and endometritis in a mare". The Canadian Veterinary Journal. 46 (11): 1029–1033. PMC 1259148. PMID 16363331.
- Gruys E, van Dijk JE (1976). "Four canine ovarian teratomas and a nonovarian feline teratoma". Veterinary Pathology. 13 (6): 455–459. doi:10.1177/030098587601300609. PMID 1006958. S2CID 46250641.
- López RM, Múrcia DB (August 2008). "First description of malignant retrobulbar and intracranial teratoma in a lesser kestrel (Falco naumanni)". Avian Pathology. 37 (4): 413–414. doi:10.1080/03079450802216660. PMID 18622858. S2CID 748134.
- Gutierrez-Aranda I, Ramos-Mejia V, Bueno C, Munoz-Lopez M, Real PJ, Mácia A, et al. (September 2010). "Human induced pluripotent stem cells develop teratoma more efficiently and faster than human embryonic stem cells regardless the site of injection". Stem Cells. 28 (9): 1568–1570. doi:10.1002/stem.471. PMC 2996086. PMID 20641038.
- "A Stem Cell Legacy: Leroy Stevens". The Scientist Magazine®.
- Knoepfler P (2021-01-14). "What is a teratoma? Research & treatment". The Niche. Retrieved 2021-02-07.
- Lee MO, Moon SH, Jeong HC, Yi JY, Lee TH, Shim SH, et al. (August 2013). "Inhibition of pluripotent stem cell-derived teratoma formation by small molecules". Proceedings of the National Academy of Sciences of the United States of America. 110 (35): E3281 – E3290. Bibcode:2013PNAS..110E3281L. doi:10.1073/pnas.1303669110. PMC 3761568. PMID 23918355.
- McDonald, Daniella; Wu, Yan; Dailamy, Amir; Tat, Justin; Parekh, Udit; Zhao, Dongxin; Hu, Michael; Tipps, Ann; Zhang, Kun; Mali, Prashant (2020-11-25). "Defining the Teratoma as a Model for Multi-lineage Human Development". Cell. 183 (5): 1402–1419.e18. doi:10.1016/j.cell.2020.10.018. ISSN 1097-4172. PMC 7704916. PMID 33152263.
![]() This article incorporates public domain material from Dictionary of Cancer Terms. U.S. National Cancer Institute.
This article incorporates public domain material from Dictionary of Cancer Terms. U.S. National Cancer Institute.
External links
- humpath pathology images #2657 Archived 2017-09-01 at the Wayback Machine (Teratomas), #4541 Archived 2017-09-01 at the Wayback Machine (Mature teratoma), #5350 Archived 2017-09-01 at the Wayback Machine (Immature teratoma)
- cystic teratoma at eMedicine (also search EMedicine for all articles containing the word teratoma)
| Classification | D |
|---|---|
| External resources |
| Germ cell tumors | |
|---|---|
| Germinomatous | |
| Nongerminomatous | |
| Skin cancer of the dermis | |||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Dermis | |||||||||||||||||
| Subcutaneous tumors |
| ||||||||||||||||
| |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Testicles |
| ||||||||
| Prostate | |||||||||
| Penis | |||||||||