This is an old revision of this page, as edited by Shangkuanlc (talk | contribs) at 00:37, 15 September 2014 (→Seizures: rearrange paragraphs). The present address (URL) is a permanent link to this revision, which may differ significantly from the current revision.
Revision as of 00:37, 15 September 2014 by Shangkuanlc (talk | contribs) (→Seizures: rearrange paragraphs)(diff) ← Previous revision | Latest revision (diff) | Newer revision → (diff) "Epilepsia" and "Epileptic" redirect here. For the journal, see Epilepsia (journal). For the graphic novel, see Epileptic (graphic novel).Medical condition
| Epilepsy | |
|---|---|
| Specialty | Neurology, epileptology |
| Frequency | 0.9% |
Epilepsy (from the Ancient Greek verb ἐπιλαμβάνειν meaning "to seize, possess, or afflict") is a group of long-term neurological disorders characterized by epileptic seizures. These seizures are episodes that can vary from brief and nearly undetectable to long periods of vigorous shaking. In epilepsy, seizures tend to recur, and have no immediate underlying cause while seizures that occur due to a specific cause are not deemed to represent epilepsy.
In most cases the cause is unknown, although some people develop epilepsy as the result of brain injury, stroke, brain tumor, and drug and alcohol misuse, among others. Epileptic seizures are the result of excessive and abnormal cortical nerve cell activity in the brain. The diagnosis typically involves ruling out other conditions that might cause similar symptoms (such as syncope) as well as figuring out whether any immediate causes are present. Epilepsy can often be confirmed with an electroencephalogram (EEG).
Epilepsy cannot be cured, but seizures are controllable with medication in about 70% of cases. In those whose seizures do not respond to medication, surgery, neurostimulation or dietary changes may be considered. Not all cases of epilepsy are lifelong, and a substantial number of people improve to the point that medication is no longer needed.
About 1% of people worldwide (65 million) have epilepsy, and nearly 80% of cases occur in developing countries. Epilepsy becomes more common as people age. In the developed world, onset of new cases occurs most frequently in infants and the elderly; in the developing world this is in older children and young adults, due to differences in the frequency of the underlying causes. About 5–10% of all people will have an unprovoked seizure by the age of 80, and the chance of experiencing a second seizure is between 40 and 50%. In many areas of the world those with epilepsy either have their ability to drive restricted or disallowed, but most are able to return to driving after a period of time without seizures.
Signs and symptoms
Epilepsy is characterized by a long-term risk of recurrent seizures. These seizures may present in several ways depending on the part of the brain involved and the person's age.
Seizures
The most common type (60%) of seizures are convulsive. Of these, two-thirds begin as focal seizures (which may then become generalized) while one-third begin as generalized seizures. The remaining 40% of seizures are non-convulsive. An example of this type is the absence seizure, which presents as a decreased level of consciousness and usually lasts about 10 seconds.
Focal seizures are often preceded by certain experiences, known as an aura. These may include sensory (visual, hearing or smell), psychic, autonomic, or motor phenomena. Jerking activity may start in a specific muscle group and spread to surrounding muscle groups in which case it is known as a Jacksonian march. Automatisms may occur; these are non-consciously generated activities and mostly simple repetitive movements like smacking of the lips or more complex activities such as attempts to pick something up.
There are six main types of generalized seizures: tonic-clonic, tonic, clonic, myoclonic, absence, and atonic seizures. They all involve loss of consciousness and typically happen without warning.
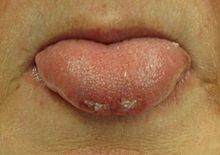
Tonic-clonic seizures present with a contraction of the limbs followed by their extension along with arching of the back which lasts 10–30 seconds (the tonic phase). A cry may be heard due to contraction of the chest muscles. This is then followed by a shaking of the limbs in unison (clonic phase). Tonic seizures produce constant contractions of the muscles. A person often turns blue as breathing is stopped. In clonic seizures there is shaking of the limbs in unison. After the shaking has stopped it may take 10–30 minutes for the person to return to normal; this period is called the "postictal phase". Loss of bowel or bladder control may occur during a seizure. The tongue may be bitten at either the tip or on the sides during a seizure. In tonic-clonic seizure, bites to the sides are more common. Tongue bites are also relatively common in psychogenic non-epileptic seizures.
Myoclonic seizures involve spasms of muscles in either a few areas or all over. Absence seizures can be subtle with only a slight turn of the head or eye blinking. The person does not fall over and returns to normal right after it ends. Atonic seizures involve the loss of muscle activity for greater than one second. This typically occurs on both sides of the body.
About 6% of those with epilepsy have seizures that are often triggered by specific events and are known as reflex seizures. Those with reflex epilepsy have seizures that are only triggered by specific stimuli. Common triggers include flashing lights and sudden noises. In certain types of epilepsy, seizures happen more often during sleep, and in other types they occur almost only when sleeping.
Postictal
After the active portion of a seizure, there is typically a period of confusion referred to as the postictal period before a normal level of consciousness returns. This usually lasts 3 to 15 minutes but may last for hours. Other common symptoms include feeling tired, headache, difficulty speaking, and abnormal behavior. Psychosis after a seizure is relatively common, occurring in 6–10% of people. Often people do not remember what happened during this time. Localized weakness, known as Todd's paralysis, may also occur after a focal seizure. When it occurs it typically lasts for seconds to minutes but may rarely last for a day or two.
Psychosocial
Epilepsy can have adverse effects on social and psychological well-being. These effects may include social isolation, stigmatization, or disability. They may result in lower educational achievement and worse employment outcomes. Learning difficulties are common in those with the condition, and especially among children with epilepsy. The stigma of epilepsy can also affect the families of those with the disease.
Certain disorders occur more often in people with epilepsy, depending partly on the epilepsy syndrome present. These include depression, anxiety disorders, and migraines. Attention-deficit hyperactivity disorder affects three to five times more children with epilepsy than children in the general population. ADHD and epilepsy have significant consequences on a child's behavioral, learning, and social development. Epilepsy is also more common in those with autism.
Causes
See also: Causes of seizuresEpilepsy is not a single disease but a symptom that can result from a number of different disorders. By definition the seizures occur spontaneously and without an immediate cause such as acute illness. The underlying cause of epilepsy may be identified as genetic or as due to structural or metabolic problems, but in 60% of cases the cause is unknown. Genetic, congenital, and developmental conditions are more common among younger people, while brain tumors and strokes are more likely in older people. Seizures may also occur as a consequence of other health problems; if they occur right around a specific cause, such as a stroke, head injury, toxic ingestion or metabolic problem, they are known as acute symptomatic seizures and are in the broader classification of seizure-related disorders rather than epilepsy itself. Many of the causes of acute symptomatic seizures can also lead to latter seizures in which case it is known as secondary epilepsy.
Genetics
Genetics is believed to be involved in the majority of cases, either directly or indirectly. Some epilepsies are due to a single gene defect (1–2%); most are due to the interaction of multiple genes and environmental factors. Each of the single gene defects is rare, with more than 200 in all described. Some of the genes involved affect ion channels, enzymes, GABA, and G protein-coupled receptors.
In identical twins, if one is affected there is a 50–60% chance that the other will also be affected. In non-identical twins the risk is 15%. These risks are greater in those with generalized than focal seizures. If both twins are affected, most of the time they have the same epileptic syndrome (70–90%). Other close relatives of a person with epilepsy have a risk five times that of the general population. Between 1 and 10% of those with Down syndrome and 90% of those with Angelman syndrome have epilepsy.
Secondary
Epilepsy may occur as a result of a number of other conditions including tumors, strokes, head trauma, previous infections of the central nervous system, genetic abnormalities, and as a result of brain damage around the time of birth. Of those with brain tumors, almost 30% have epilepsy, making them the cause of about 4% of cases. The risk is greatest for tumors in the temporal lobe and those that grow slowly. Other mass lesions such as cerebral cavernous malformations and artiovenous malformations have risks as high as 40–60%. Of those who have had a stroke, 2–4% develop epilepsy. In the United Kingdom strokes account for 15% of cases and it is believed to be the cause in 30% of the elderly. Between 6 and 20% of epilepsy is believed to be due to head trauma. Mild brain injury increases the risk about two-fold while severe brain injury increases the risk seven-fold. In those who have experienced a high powered gunshot wound to the head, the risk is about 50%.
The risk of epilepsy following meningitis is less than 10%; that disease more commonly causes seizures during the infection itself. In herpes simplex encephalitis the risk of a seizure is around 50% with a high risk of epilepsy following (up to 25%). Infection with the pork tapeworm, which can result in neurocysticercosis, is the cause of up to half of epilepsy cases in areas of the world where the parasite is common. Epilepsy may also occur after other brain infections such as cerebral malaria, toxoplasmosis, and toxocariasis. Chronic alcohol use increases the risk of epilepsy: those who drink six units of alcohol per day have a two and a half fold increase in risk. Other risks include Alzheimer's disease, multiple sclerosis, tuberous sclerosis, and autoimmune encephalitis. Getting vaccinated does not increase the risk of epilepsy. Malnutrition is a risk factor seen mostly in the developing world, although it is unclear however if it is a direct cause or an association.
Syndromes
See also: List of epilepsy syndromesThere are a number of epilepsy syndromes which are typically grouped by age of onset into neonatal period, childhood, adulthood, and those with no strong age relationship. Additionally there are groups with specific constellations of symptoms, those due to specific metabolic or structural causes, and those of unknown cause. The ability to classify a case of epilepsy into a specific syndrome occurs more often with children. Some types include benign rolandic epilepsy (2.8 per 100,000), childhood absence epilepsy (0.8 per 100,000) and juvenile myoclonic epilepsy (0.7 per 100,000). Febrile seizures and benign neonatal seizures are not forms of epilepsy.
Mechanism
Normally brain electrical activity is non-synchronous. In epileptic seizures, due to structural or functional problems within the brain, a group of neurons begin firing in an abnormal, excessive, and synchronized manner. This results in a wave of depolarization known as a paroxysmal depolarizing shift.
Normally, after an excitatory neuron fires it becomes more resistant to firing for a period of time. This is due in part to the effect of inhibitory neurons, electrical changes within the excitatory neuron, and the negative effects of adenosine. In epilepsy the resistance of excitatory neurons to fire during this period is decreased. This may occur due to changes in ion channels or inhibitory neurons not functioning properly. This then results in a specific area from which seizures may develop, known as a "seizure focus". Another mechanism of epilepsy may be the up-regulation of excitatory circuits or down-regulation of inhibitory circuits following an injury to the brain. These secondary epilepsies occur through processes known as epileptogenesis. Failure of the blood–brain barrier may also be a causal mechanism as it would allow substances in the blood to enter the brain.
Focal seizures begin in one hemisphere of the brain while generalized seizures begin in both hemispheres. Some types of seizures may change brain structure, while others appear to have little effect. Gliosis, neuronal loss, and atrophy of specific areas of the brain are linked to epilepsy but it is unclear if epilepsy causes these changes or if these changes result in epilepsy.
Diagnosis
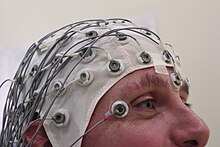
The diagnosis of epilepsy is typically made based on the description of the seizure and surrounding events. An electroencephalogram and neuroimaging are also usually part of the workup. While figuring out a specific epileptic syndrome is often attempted, it is not always possible. Video and EEG monitoring may be useful in difficult cases.
Definition
As of 2014, epilepsy is defined by the International League Against Epilepsy as a person who meets any of the following conditions:
- At least two unprovoked (or reflex) seizures occurring greater than 24 hours apart.
- One unprovoked (or reflex) seizure and a probability of further seizures similar to the general recurrence risk (at least 60%) after two unprovoked seizures, occurring over the next 10 years.
- Diagnosis of an epilepsy syndrome
This is a refinement of their 2005 definition which was "a disorder of the brain characterized by an enduring predisposition to generate epileptic seizures and by the neurobiologic, cognitive, psychological, and social consequences of this condition. The definition of epilepsy requires the occurrence of at least one epileptic seizure."
The 2014 definition is practical in nature and is designed for clinical use. Researchers, statistically-minded epidemiologists and other specialized groups may choose to use the older definition or a definition of their own devising. The ILAE considers doing so is perfectly allowable, so long as it is clear what definition is being used.
Epilepsy is considered to have resolved for individuals who had an age-dependent epilepsy syndrome but are now past the applicable age or those who have remained seizure-free for the last 10 years, with no seizure medicines for the last 5 years. It is therefore possible to outgrow epilepsy or to undergo treatment that causes the epilepsy to be resolved. Resolution of epilepsy unfortunately does not guarantee that it will not return.
In the definition, epilepsy is now called a disease, rather than a disorder. This was a decision of the executive committee of the ILAE, taken because the word "disorder," while perhaps having less stigma than does "disease," also does not express the degree of seriousness that epilepsy deserves.
Classification
Those with seizures should be classified by seizure type, underlying cause, epilepsy syndrome, and events during and around the time of the seizures. Seizure types are organized by whether the source of the seizure is localized (focal seizures) or distributed (generalized seizures) within the brain. Generalized seizures are divided according to the effect on the body and include tonic-clonic (grand mal), absence (petit mal), myoclonic, clonic, tonic, and atonic seizures. Some seizures such as epileptic spasms are of an unknown type.
Focal seizures (previously known as partial seizures) used to be divided into simple partial or complex partial seizure. This is no longer recommended, and instead it is preferred to describe what has occurred during a seizure.
Lab tests
For adults, the testing of electrolyte, blood glucose and calcium levels is important to rule out problems with these as causes. An electrocardiogram can rule out problems with the rhythm of the heart. A lumbar puncture may be useful to diagnose a central nervous system infection but is not routinely needed. In children additional tests may be required such as urine biochemistry and blood testing looking for metabolic disorders.
A high blood prolactin level within the first 20 minutes following a seizure may be useful to confirm an epileptic seizure as opposed to psychogenic non-epileptic seizure. Serum prolactin level is less useful for detecting partial seizures. If it is normal an epileptic seizure is still possible and a serum prolactin does not separate epileptic seizures from syncope. It is not recommended as a routine part of the diagnosis of epilepsy.
EEG
An electroencephalogram (EEG) can assist in showing brain activity suggestive of an increased risk of seizures. It is only recommended for those who are likely to have had an epileptic seizure on the basis of symptoms. In the diagnosis of epilepsy, electroencephalography may help distinguish the type of seizure or syndrome present. In children it is typically only needed after a second seizure. It cannot be used to rule out the diagnosis, and may be falsely positive in those without the disease. In certain situations it may be useful to perform the EEG while the affected individual is sleeping or sleep deprived.
Imaging
Diagnostic imaging by CT scan and MRI is recommended after a first non-febrile seizure to detect structural problems in and around the brain. MRI is generally a better imaging test except when bleeding is suspected, for which CT is more sensitive and more easily available. If someone attends the emergency room with a seizure but returns to normal quickly, imaging tests may be done at a later point. If a person has a previous diagnosis of epilepsy with previous imaging, repeating the imaging is usually not needed even if there are subsequent seizures.
Differential diagnosis
Diagnosis of epilepsy can be difficult, and misdiagnosis is frequent (occurring in about 5 to 30% of cases). A number of other conditions may present very similar signs and symptoms to epilepsy, including syncope, hyperventilation, migraines, narcolepsy, panic attacks and psychogenic non-epileptic seizures (PNES). Approximately one in five people seen at epilepsy clinics have PNES and of those who have PNES about 10% also have epilepsy. Separating the two based on the seizure episode alone without further testing is often difficult.
Children may have behaviors that are easily mistaken for epileptic seizures but are not. These include breath-holding spells, bed wetting, night terrors, tics and shudder attacks. Gastroesophageal reflux may cause arching of the back and twisting of the head to the side in infants, which may be mistaken for tonic-clonic seizures.
Prevention
While many cases are not preventable, efforts to reduce head injuries, provide good care around the time of birth, and reduce environmental parasites such as the pork tapeworm may be effective. Efforts in one part of Central America to decrease rates of pork tapeworm resulted in a 50% decrease in new cases of epilepsy.
Management
Epilepsy is usually treated with daily medication once a second seizure has occurred, but for those at high risk, medication may be started after the first seizure. In some cases, a special diet, the implantation of a neurostimulator, or neurosurgery may be required.
First aid
Rolling a person with an active tonic-clonic seizure onto their side and into the recovery position helps prevent fluids from getting into the lungs. Putting fingers, a bite block or tongue depressor in the mouth is not recommended as it might make the person vomit or result in the rescuer being bitten. Efforts should be taken to prevent further self-injury. Spinal precautions are generally not needed.
If a seizure lasts longer than 5 minutes or if there are more than two seizures in an hour without a return to normal between them it is considered a medical emergency known as status epilepticus. This may require medical help to keep the airway open and protected; a nasopharyngeal airway may be useful for this. At home the recommended initial medication for seizure of a long duration is midazolam placed in the mouth. Diazepam may also be used rectally. In hospital, intravenous lorazepam is preferred. If two doses of benzodiazepines are not effective, other medications such as phenytoin are recommended. Convulsive status epilepticus that does not respond to initial treatment typically requires admission to the intensive care unit and treatment with stronger agents such as thiopentone or propofol.
Medications
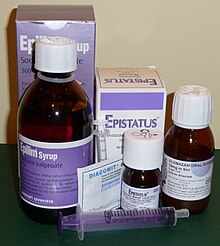
The mainstay treatment of epilepsy is anticonvulsant medications, possibly for the person's entire life. The choice of anticonvulsant is based on seizure type, epilepsy syndrome, other medications used, other health problems, and the person's age and lifestyle. A single medication is recommended initially; if this is not effective, switching to a single other medication is recommended. Two medications at once is only recommended if a single medication does not work. In about half, the first agent is effective; a second single agent helps in about 13% and a third or two agents at the same time may help an additional 4%. About 30% of people continue to have seizures despite anticonvulsant treatment.
There are a number of medications available. Phenytoin, carbamazepine and valproate appear to be equally effective in both focal and generalized seizures. Controlled release carbamazepine appears to work as well as immediate release carbamazepine, and may have fewer side effects. In the United Kingdom, carbamazepine or lamotrigine are recommended as first-line treatment for focal seizures, with levetiracetam and valproate as second-line due to issues of cost and side effects. Valproate is recommended first-line for generalized seizures with lamotrigine being second-line. In those with absence seizures, ethosuximide or valproate are recommended; valproate is particularly effective in myoclonic seizures and tonic or atonic seizures. If seizures are well-controlled on a particular treatment, it is not usually necessary to routinely check the medication levels in the blood.
The least expensive anticonvulsant is phenobarbital at around $5 USD a year. The World Health Organization gives it a first-line recommendation in the developing world and it is commonly used there. Access however may be difficult as some countries label it as a controlled drug.
Adverse effects from medications are reported in 10 to 90% of people, depending on how and from whom the data is collected. Most adverse effects are dose-related and mild. Some examples include mood changes, sleepiness, or an unsteadiness in gait. Some medications have side effects that are not related to dose such as rashes, liver toxicity, or suppression of the bone marrow. Up to a quarter of people stop treatment due to adverse effects. Some medications are associated with birth defects when used in pregnancy. Valproate is of particular concern, especially during the first trimester. Despite this, treatment is often continued once effective, because the risk of untreated epilepsy is believed to be greater than the risk of the medications.
Slowly stopping medications may be reasonable in some people who do not have a seizure for two to four years; however, around a third of people have a recurrence, most often during the first six months. Stopping is possible in about 70% of children and 60% of adults.
Surgery
Epilepsy surgery may be an option for people with focal seizures that remain a problem despite other treatments. These other treatments include at least a trial of two or three medications. The goal of surgery is total control of seizures and this may be achieved in 60–70% of cases. Common procedures include cutting out the hippocampus via an anterior temporal lobe resection, removal of tumors, and removing parts of the neocortex. Some procedures such as a corpus callosotomy are attempted in an effort to decrease the number of seizures rather than cure the condition. Following surgery, medications may be slowly withdrawn in many cases.
Neurostimulation may be another option in those who are not candidates for surgery. Three types have been shown to be effective in those who do not respond to medications: vagus nerve stimulation, anterior thalamic stimulation, and closed-loop responsive stimulation.
Other
A ketogenic diet (high-fat, low-carbohydrate, adequate-protein) appears to decrease the number of seizures by half in about 30–40% of children. About 10% manage to stay on the diet for a few years, 30% had constipation, and other adverse effects were common. Less radical diets were easier to tolerate and may be effective. It is unclear why this diet works. Exercise has been proposed as possibly useful for preventing seizures with some data to support this claim.
Avoidance therapy consists of minimizing or eliminating triggers. For example, in those who are sensitive to light, using a small television, avoiding video-games or wearing dark glasses may be useful. Some claim that seizure response dogs, a form of service dog, can predict seizures. Evidence for this, however, is poor. Operant-based biofeedback based on the EEG waves has some support in those who do not respond to medications. Psychological methods should not, however, be used to replace medications.
Alternative medicine
Alternative medicine, including acupuncture, psychological interventions, routine vitamins, and yoga, have no reliable evidence to support their use in epilepsy. The use of cannabis is not supported by the evidence. Melatonin is insufficiently supported by evidence.
Prognosis

Epilepsy cannot usually be cured, but medication can control seizures effectively in about 70% of cases. Of those with generalized seizure more than 80% can be well controlled with medications while this is true in only 50% of people with focal seizures. One predictor of long-term outcome is the number of seizures that occur in the first six months. Other factors increasing the risk of a poor outcome include little response to the initial treatment, generalized seizures, a family history of epilepsy, psychiatric problems, and waves on the EEG representing generalized epileptiform activity. In the developing world 75% of people are either untreated or not appropriately treated. In Africa 90% do not get treatment. This is partly related to appropriate medications not being available or being too expensive.
Mortality
People with epilepsy are at an increased risk of death. This increase is between 1.6 and 4.1 fold greater than that of the general population and is often related to: the underlying cause of the seizures, status epilepticus, suicide, trauma, and sudden unexpected death in epilepsy (SUDEP). Death from status epilepticus is primarily due to an underlying problem rather than missing doses of medications. The risk of suicide is increased between two and six times in those with epilepsy. The cause of this is unclear. SUDEP appears to be partly related to the frequency of generalized tonic-clonic seizures and accounts for about 15% of epilepsy related deaths. It is unclear how to decrease its risk. The greatest increase in mortality from epilepsy is among the elderly. Those with epilepsy due to an unknown cause have little increased risk. In the United Kingdom it is estimated that 40–60% of deaths are possibly preventable. In the developing world many deaths are due to untreated epilepsy leading to falls or status epilepticus.
Epidemiology
Epilepsy is one of the most common serious neurological disorders affecting about 65 million people globally. It affects 1% of the population by age 20 and 3% of the population by age 75. It is more common in males than females with the overall difference being small. Most of those with the disease (80%) are in the developing world.
The number of people who currently have active epilepsy is in the range 5–10 per 1,000, with active epilepsy defined as someone with epilepsy who has had a least one seizure in the last five years. Epilepsy begins each year in 40–70 per 100,000 in developed countries and 80–140 per 100,000 in developing countries. Poverty is a risk and includes both being from a poor country and being poor relative to others within one's country. In the developed world epilepsy most commonly starts either in the young or in the old. In the developing world its onset is more common in older children and young adults due to the higher rates of trauma and infectious diseases. In developed countries the number of cases a year has decreased in children and increased among the elderly between the 1970s and 2003. This has been attributed partly to better survival following strokes in the elderly.
History
The oldest medical records show that epilepsy has been affecting people since the beginning of recorded history. Throughout ancient history, the disorder was thought to be a spiritual condition. The world's oldest description of an epileptic seizure comes from a text in Akkadian (a language used in ancient Mesopotamia) and was written around 2000 BCE. The person described in the text was diagnosed as being under the influence of a Moon god, and underwent an exorcism. Epileptic seizures are listed in the Code of Hammurabi (c. 1790 BCE) as reason for which a purchased slave may be returned for a refund, and the Edwin Smith Papyrus (c. 1700 BCE) describes cases of individuals with epileptic convulsions.
The oldest known detailed record of the disorder itself is in the Sakikkū, a Babylonian cuneiform medical text from 1067–1046 BCE. This text gives signs and symptoms, details treatment and likely outcomes, and describes many features of the different seizure types. As the Babylonians had no biomedical understanding of the nature of disease, they attributed the seizures to possession by evil spirits and called for treating the condition through spiritual means. Around 900 BCE, Punarvasu Ātreya described epilepsy as loss of consciousness; this definition was carried forward into the Ayurvedic text of Charaka Samhita (about 400 BCE).

The ancient Greeks had contradictory views of the disease. They thought of epilepsy as a form of spiritual possession, but also associated the condition with genius and the divine. One of the names they gave to it was the sacred disease. Epilepsy appears within Greek mythology: it is associated with the Moon goddesses Selene and Artemis, who afflicted those who upset them. The Greeks thought that important figures such as Julius Caesar and Hercules had the disease. The notable exception to this divine and spiritual view was that of the school of Hippocrates. In the fifth century BCE, Hippocrates rejected the idea that the disease was caused by spirits. In his landmark work On the Sacred Disease, he proposed that epilepsy was not divine in origin and instead was a medically treatable problem originating in the brain. He accused those of attributing a sacred cause to the disease of spreading ignorance through a belief in superstitious magic. Hippocrates proposed that heredity was important as a cause, described worse outcomes if the disease presents at an early age, and made note of the physical characteristics as well as the social shame associated with it. Instead of referring to it as the sacred disease, he used the term great disease, giving rise to the modern term grand mal, used for generalized seizures. Despite his work detailing the physical origins of the disease, his view was not accepted at the time. Evil spirits continued to be blamed until at least the 17th century.
In most cultures, persons with epilepsy have been stigmatized, shunned, or even imprisoned; in the Salpêtrière, the birthplace of modern neurology, Jean-Martin Charcot found people with epilepsy side-by-side with the mentally ill, those with chronic syphilis, and the criminally insane. In ancient Rome, epilepsy was known as the Morbus Comitialis ('disease of the assembly hall') and was seen as a curse from the gods. In northern Italy, epilepsy was once traditionally known as Saint Valentine's malady.
In the mid-1800s the first effective anti-seizure medication, bromide, was introduced. The first modern treatment, phenobarbital, was developed in 1912, with phenytoin coming into use in 1938.
Society and culture
See also: List of people with epilepsyStigma
Stigma is commonly experienced, around the world, by those with epilepsy. It can affect people economically, socially and culturally. In India and China epilepsy may be used as justification to deny marriage. People in some areas still believe those with epilepsy to be cursed. In Tanzania, as in other parts of Africa, epilepsy is associated with possession by evil spirits, witchcraft, or poisoning and is believed by many to be contagious, for which there is no evidence. Before 1970 the United Kingdom had laws which prevented people with epilepsy from marrying. The stigma may result in some people with epilepsy denying that they have ever had seizures.
Economics
Seizures result in direct economic costs of about one billion dollars in the United States. Epilepsy resulted in economic costs in Europe of around 15.5 billion Euros in 2004. In India epilepsy is estimated to result in costs of 1.7 billion USD or 0.5% of the GDP. It is the cause of about 1% of emergency department visits (2% for emergency departments for children) in the United States.
Vehicles
See also: Epilepsy and drivingThose with epilepsy are at about twice the risk of being involved in a motor vehicular collision and thus in many areas of the world are not allowed to drive or only able to drive if certain conditions are met. In some places physicians are required by law to report if a person has had a seizure to the licensing body while in others the requirement is only that they encourage the person in question to report it themselves. Countries that require physician reporting include Sweden, Austria, Denmark and Spain. Countries that require the individual to report include the UK, and New Zealand and the physician may report if they believe the individual has not already. In Canada, the United States and Australia the requirements around reporting vary by province or state. If seizures are well controlled most feel allowing driving is reasonable. The amount of time a person must be free from seizures before they can drive varies by country. Many countries require one to three years without seizures. In the United States the time needed without a seizure is determined by each state and is between three months and one year.
Those with epilepsy or seizures are typically denied a pilot license. In Canada if an individual has had no more than one seizure, they may be considered after five years for a limited license if all other testing is normal. Those with febrile seizures and drug related seizures may also be considered. In the United States, the Federal Aviation Administration does not allow those with epilepsy to get a commercial pilot license. Rarely, exceptions can be made for persons who have had an isolated seizure or febrile seizures and have remained free of seizures into adulthood without medication. In the United Kingdom, a full national private pilot license requires the same standards as a professional driver's license. This requires a period of ten years without seizures while off medications. Those who do not meet this requirement may acquire a restricted license if free from seizures for five years.
Support organizations
There are organizations that provide support for people and families affected by epilepsy. The Out of the Shadows campaign, a joint effort by the World Health Organization, the International League Against Epilepsy and the International Bureau for Epilepsy, provides help internationally. The Joint Epilepsy Council serves the UK and Ireland. In the United States, the Epilepsy Foundation is a national organization that works to increase the acceptance of those with the disease, their ability to function in society and to promote research for a cure. The Epilepsy Foundation, some hospitals, and some individuals also run support groups in the United States.
Research
Seizure prediction refers to attempts to forecast epileptic seizures based on the EEG before they occur. As of 2011, no effective mechanism to predict seizures has been developed. Kindling, where repeated exposures to events that could cause seizures eventually causes seizures more easily, has been used to create animal models of epilepsy.
Gene therapy is being studied in some types of epilepsy. Medications that alter immune function, such as intravenous immunoglobulins, are poorly supported by evidence. Noninvasive stereotactic radiosurgery is, as of 2012, being compared to standard surgery for certain types of epilepsy.
Other animals
Main article: Epilepsy in animalsEpilepsy occurs in a number of other animals including dogs and cats and is the most common brain disorder in dogs. It is typically treated with anticonvulsants such as phenobarbital or bromide in dogs and phenobarbital in cats. Imepitoin is also being used in dogs. While generalized seizures in horses are fairly easy to diagnose, it may be more difficult in non-generalized seizures and EEGs may be useful.
References
- ^ Magiorkinis E, Kalliopi S, Diamantis A (January 2010). "Hallmarks in the history of epilepsy: epilepsy in antiquity". Epilepsy & behavior : E&B. 17 (1): 103–108. doi:10.1016/j.yebeh.2009.10.023. PMID 19963440.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Chang BS, Lowenstein DH (2003). "Epilepsy". N. Engl. J. Med. 349 (13): 1257–66. doi:10.1056/NEJMra022308. PMID 14507951.
- ^ "Epilepsy". Fact Sheets. World Health Organization. October 2012. Retrieved January 24, 2013.
- ^ Fisher R, van Emde Boas W, Blume W, Elger C, Genton P, Lee P, Engel J (2005). "Epileptic seizures and epilepsy: definitions proposed by the International League Against Epilepsy (ILAE) and the International Bureau for Epilepsy (IBE)". Epilepsia. 46 (4): 470–2. doi:10.1111/j.0013-9580.2005.66104.x. PMID 15816939.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Eadie, MJ (December 2012). "Shortcomings in the current treatment of epilepsy". Expert Review of Neurotherapeutics. 12 (12): 1419–27. doi:10.1586/ern.12.129. PMID 23237349.
- ^ Thurman, DJ (September 2011). "Standards for epidemiologic studies and surveillance of epilepsy". Epilepsia. 52 Suppl 7: 2–26. doi:10.1111/j.1528-1167.2011.03121.x. PMID 21899536.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - Brodie, MJ (November 2009). "Epilepsy in later life". Lancet neurology. 8 (11): 1019–30. doi:10.1016/S1474-4422(09)70240-6. PMID 19800848.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Holmes, Thomas R. Browne, Gregory L. (2008). Handbook of epilepsy (4th ed.). Philadelphia: Lippincott Williams & Wilkins. p. 7. ISBN 978-0-7817-7397-3.
{{cite book}}: CS1 maint: multiple names: authors list (link) - Wyllie's treatment of epilepsy : principles and practice (5th ed.). Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins. 2010. ISBN 978-1-58255-937-7.
- ^ Newton, CR (29 September 2012). "Epilepsy in poor regions of the world". Lancet. 380 (9848): 1193–201. doi:10.1016/S0140-6736(12)61381-6. PMID 23021288.
- ^ Wilden, JA; Cohen-Gadol, AA (15 August 2012). "Evaluation of first nonfebrile seizures". American family physician. 86 (4): 334–40. PMID 22963022.
- Berg, AT (2008). "Risk of recurrence after a first unprovoked seizure". Epilepsia. 49 Suppl 1: 13–8. doi:10.1111/j.1528-1167.2008.01444.x. PMID 18184149.
- ^ L Devlin, A (December 2012). "Epilepsy and driving: current status of research". Epilepsy research. 102 (3): 135–52. doi:10.1016/j.eplepsyres.2012.08.003. PMID 22981339.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Duncan, JS (1 April 2006). "Adult epilepsy" (PDF). Lancet. 367 (9516): 1087–100. doi:10.1016/S0140-6736(06)68477-8. PMID 16581409.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ National Institute for Health and Clinical Excellence (January 2012). "Chapter 1: Introduction". The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care (PDF). National Clinical Guideline Centre. pp. 21–28.
- ^ Hammer, edited by Stephen J. McPhee, Gary D. (2010). "7". Pathophysiology of disease : an introduction to clinical medicine (6th ed. ed.). New York: McGraw-Hill Medical. ISBN 978-0-07-162167-0.
{{cite book}}:|edition=has extra text (help);|first=has generic name (help)CS1 maint: multiple names: authors list (link) - Hughes, JR (August 2009). "Absence seizures: a review of recent reports with new concepts". Epilepsy & behavior : E&B. 15 (4): 404–12. doi:10.1016/j.yebeh.2009.06.007. PMID 19632158.
- ^ Shearer, Peter. "Seizures and Status Epilepticus: Diagnosis and Management in the Emergency Department". Emergency Medicine Practice.
- ^ Bradley, Walter G. (2012). "67". Bradley's neurology in clinical practice (6th ed. ed.). Philadelphia, PA: Elsevier/Saunders. ISBN 978-1-4377-0434-1.
{{cite book}}:|edition=has extra text (help) - ^ National Institute for Health and Clinical Excellence (January 2012). "Chapter 9: Classification of seizures and epilepsy syndromes". The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care (PDF). National Clinical Guideline Centre. pp. 119–129.
- ^ Engel, Jerome (2008). Epilepsy : a comprehensive textbook (2nd ed. ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 2797. ISBN 978-0-7817-5777-5.
{{cite book}}:|edition=has extra text (help) - ^ Simon, David A. Greenberg, Michael J. Aminoff, Roger P. (2012). "12". Clinical neurology (8th ed. ed.). New York: McGraw-Hill Medical. ISBN 978-0-07-175905-2.
{{cite book}}:|edition=has extra text (help)CS1 maint: multiple names: authors list (link) - ^ Steven C. Schachter, ed. (2008). Behavioral aspects of epilepsy : principles and practice (. ed.). New York: Demos. p. 125. ISBN 978-1-933864-04-4.
- Xue, LY; Ritaccio, AL (March 2006). "Reflex seizures and reflex epilepsy". American journal of electroneurodiagnostic technology. 46 (1): 39–48. PMID 16605171.
- Malow, BA (November 2005). "Sleep and epilepsy". Neurologic Clinics. 23 (4): 1127–47. doi:10.1016/j.ncl.2005.07.002. PMID 16243619.
- Tinuper, P; Provini, F; Bisulli, F; Vignatelli, L; Plazzi, G; Vetrugno, R; Montagna, P; Lugaresi, E (August 2007). "Movement disorders in sleep: guidelines for differentiating epileptic from non-epileptic motor phenomena arising from sleep". Sleep medicine reviews. 11 (4): 255–67. doi:10.1016/j.smrv.2007.01.001. PMID 17379548.
- Holmes, Thomas R. (2008). Handbook of epilepsy (4th ed. ed.). Philadelphia: Lippincott Williams & Wilkins. p. 34. ISBN 978-0-7817-7397-3.
{{cite book}}:|edition=has extra text (help) - ^ Panayiotopoulos, CP (2010). A clinical guide to epileptic syndromes and their treatment based on the ILAE classifications and practice parameter guidelines (Rev. 2nd ed. ed.). : Springer. p. 445. ISBN 978-1-84628-644-5.
{{cite book}}:|edition=has extra text (help) - James W. Wheless, ed. (2009). Advanced therapy in epilepsy. Shelton, Conn.: People's Medical Pub. House. p. 443. ISBN 978-1-60795-004-2.
- Larner, Andrew J. (2010). A dictionary of neurological signs (3rd ed. ed.). New York: Springer. p. 348. ISBN 978-1-4419-7095-4.
{{cite book}}:|edition=has extra text (help) - Stefan, Hermann (2012). Epilepsy Part I: Basic Principles and Diagnosis E-Book: Handbook of Clinical Neurology (Volume 107 of Handbook of Clinical Neurology ed.). Newnes. p. 471. ISBN 978-0-444-53505-4.
- Plioplys S, Dunn DW, Caplan R (2007). "10-year research update review: psychiatric problems in children with epilepsy". J Am Acad Child Adolesc Psychiatry. 46 (11): 1389–402. doi:10.1097/chi.0b013e31815597fc. PMID 18049289.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Reilly CJ (May–June 2011). "Attention Deficit Hyperactivity Disorder (ADHD) in Childhood Epilepsy". Research in Developmental Disabilities: A Multidisciplinary Journal. 32 (3): 883–93. doi:10.1016/j.ridd.2011.01.019. PMID 21310586.
- Levisohn PM (2007). "The autism-epilepsy connection". Epilepsia. 48 (Suppl 9): 33–5. doi:10.1111/j.1528-1167.2007.01399.x. PMID 18047599.
- Berg, AT (April 2010). "Revised terminology and concepts for organization of seizures and epilepsies: report of the ILAE Commission on Classification and Terminology, 2005–2009". Epilepsia. 51 (4): 676–85. doi:10.1111/j.1528-1167.2010.02522.x. PMID 20196795.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Neligan, A; Hauser, WA; Sander, JW (2012). "The epidemiology of the epilepsies". Handbook of clinical neurology. 107: 113–33. doi:10.1016/B978-0-444-52898-8.00006-9. PMID 22938966.
- ^ Pandolfo, M. (Nov 2011). "Genetics of epilepsy". Semin Neurol. 31 (5): 506–18. doi:10.1055/s-0031-1299789. PMID 22266888.
- Dhavendra Kumar, ed. (2008). Genomics and clinical medicine. Oxford: Oxford University Press. p. 279. ISBN 978-0-19-972005-7.
- ^ Bhalla, D.; Godet, B.; Druet-Cabanac, M.; Preux, PM. (Jun 2011). "Etiologies of epilepsy: a comprehensive review". Expert Rev Neurother. 11 (6): 861–76. doi:10.1586/ern.11.51. PMID 21651333.
- Simon D. Shorvon (2011). The Causes of Epilepsy: Common and Uncommon Causes in Adults and Children. Cambridge University Press. p. 467. ISBN 978-1-139-49578-3.
- Sellner, J; Trinka, E (Oct 2012). "Seizures and epilepsy in herpes simplex virus encephalitis: current concepts and future directions of pathogenesis and management". Journal of neurology. 259 (10): 2019–30. doi:10.1007/s00415-012-6494-6. PMID 22527234.
- Somjen, George G. (2004). Ions in the Brain Normal Function, Seizures, and Stroke. New York: Oxford University Press. p. 167. ISBN 978-0-19-803459-9.
- ^ Goldberg, EM; Coulter, DA (May 2013). "Mechanisms of epileptogenesis: a convergence on neural circuit dysfunction". Nature reviews. Neuroscience. 14 (5): 337–49. doi:10.1038/nrn3482. PMID 23595016.
- Oby, E; Janigro, D (November 2006). "The blood-brain barrier and epilepsy". Epilepsia. 47 (11): 1761–74. doi:10.1111/j.1528-1167.2006.00817.x. PMID 17116015.
- ^ Jerome Engel, Jr., Timothy A. Pedley, ed. (2008). Epilepsy : a comprehensive textbook (2nd ed. ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 483. ISBN 978-0-7817-5777-5.
{{cite book}}:|edition=has extra text (help)CS1 maint: multiple names: editors list (link) - ^ National Institute for Health and Clinical Excellence (January 2012). "Chapter 4: Guidance". The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care (PDF). National Clinical Guideline Centre. pp. 57–83.
- ^ Fisher, RS (Apr 2014). "ILAE Official Report: A practical clinical definition of epilepsy". Epilepsia. 55 (4): 475–82. doi:10.1111/epi.12550. PMID 24730690.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - Robert S. Fisher, Walter van Emde Boas, Warren Blume, Christian Elger, Pierre Genton, Phillip Lee & Jerome Jr Engel (April 2005). "Epileptic seizures and epilepsy: definitions proposed by the International League Against Epilepsy (ILAE) and the International Bureau for Epilepsy (IBE)". Epilepsia. 46 (4): 470–472. doi:10.1111/j.0013-9580.2005.66104.x. PMID 15816939.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Panayiotopoulos, CP (December 2011). "The new ILAE report on terminology and concepts for organization of epileptic seizures: a clinician's critical view and contribution". Epilepsia. 52 (12): 2155–60. doi:10.1111/j.1528-1167.2011.03288.x. PMID 22004554.
- Simon D. Shorvon (2004). The treatment of epilepsy (2nd ed.). Malden, Mass.: Blackwell Pub. ISBN 978-0-632-06046-7.
- Wallace, ed. by Sheila J.; Farrell, Kevin (2004). Epilepsy in children (2nd ed ed.). London: Arnold. p. 354. ISBN 978-0-340-80814-6.
{{cite book}}:|edition=has extra text (help);|first=has generic name (help) - Luef, G (October 2010). "Hormonal alterations following seizures". Epilepsy & behavior : E&B. 19 (2): 131–3. doi:10.1016/j.yebeh.2010.06.026. PMID 20696621.
- ^ Ahmad S, Beckett MW (2004). "Value of serum prolactin in the management of syncope". Emergency medicine journal : EMJ. 21 (2): e3. doi:10.1136/emj.2003.008870. PMC 1726305. PMID 14988379.
- Shukla G, Bhatia M, Vivekanandhan S; et al. (2004). "Serum prolactin levels for differentiation of nonepileptic versus true seizures: limited utility". Epilepsy & behavior : E&B. 5 (4): 517–21. doi:10.1016/j.yebeh.2004.03.004. PMID 15256189.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - Chen DK, So YT, Fisher RS (2005). "Use of serum prolactin in diagnosing epileptic seizures: report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology". Neurology. 65 (5): 668–75. doi:10.1212/01.wnl.0000178391.96957.d0. PMID 16157897.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Brodtkorb, E (2013). "Common imitators of epilepsy". Acta neurologica Scandinavica. Supplementum (196): 5–10. doi:10.1111/ane.12043. PMID 23190285.
- ^ John A. Marx, ed. (2010). Rosen's emergency medicine : concepts and clinical practice (7th ed. ed.). Philadelphia: Mosby/Elsevier. p. 2228. ISBN 978-0-323-05472-0.
{{cite book}}:|edition=has extra text (help) - ^ Jerome, Engel (2013). Seizures and epilepsy (2nd ed. ed.). New York: Oxford University Press. p. 462. ISBN 9780195328547.
{{cite book}}:|edition=has extra text (help) - ^ Michael, GE.; O'Connor, RE. (Feb 2011). "The diagnosis and management of seizures and status epilepticus in the prehospital setting". Emerg Med Clin North Am. 29 (1): 29–39. doi:10.1016/j.emc.2010.08.003. PMID 21109100.
- James W. Wheless, James Willmore, Roger A. Brumback (2009). Advanced therapy in epilepsy. Shelton, Conn.: People's Medical Pub. House. p. 144. ISBN 9781607950042.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ National Institute for Health and Clinical Excellence (January 2012). "Chapter 3: Key priorities for implementation". The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care (PDF). National Clinical Guideline Centre. pp. 55–56.
- Elaine Wyllie (2012). Wyllie's Treatment of Epilepsy: Principles and Practice. Lippincott Williams & Wilkins. p. 187. ISBN 978-1-4511-5348-4.
- Steven R. Flanagan, Herb Zaretsky, Alex Moroz,, ed. (2010). Medical aspects of disability; a handbook for the rehabilitation professional (4th ed. ed.). New York: Springer. p. 182. ISBN 978-0-8261-2784-6.
{{cite book}}:|edition=has extra text (help)CS1 maint: extra punctuation (link) CS1 maint: multiple names: editors list (link) - Nolan, SJ; Marson, AG; Pulman, J; Tudur Smith, C (23 August 2013). "Phenytoin versus valproate monotherapy for partial onset seizures and generalised onset tonic-clonic seizures". The Cochrane database of systematic reviews. 8: CD001769. doi:10.1002/14651858.CD001769.pub2. PMID 23970302.
- Tudur Smith, C; Marson, AG; Clough, HE; Williamson, PR (2002). "Carbamazepine versus phenytoin monotherapy for epilepsy". The Cochrane database of systematic reviews (2): CD001911. doi:10.1002/14651858.CD001911. PMID 12076427.
- Powell, G; Saunders, M; Marson, AG (20 January 2010). "Immediate-release versus controlled-release carbamazepine in the treatment of epilepsy". The Cochrane database of systematic reviews (1): CD007124. doi:10.1002/14651858.CD007124.pub2. PMID 20091617.
- Ilangaratne, NB; Mannakkara, NN; Bell, GS; Sander, JW (Dec 1, 2012). "Phenobarbital: missing in action". Bulletin of the World Health Organization. 90 (12): 871-871A. doi:10.2471/BLT.12.113183. PMID 23284189.
- Moshé, edited by Simon Shorvon, Emilio Perucca, Jerome Engel Jr. ; foreword by Solomon (2009). The treatment of epilepsy (3rd ed. ed.). Chichester, UK: Wiley-Blackwell. p. 587. ISBN 9781444316674.
{{cite book}}:|edition=has extra text (help);|first=has generic name (help)CS1 maint: multiple names: authors list (link) - ^ Perucca, P; Gilliam, FG (September 2012). "Adverse effects of antiepileptic drugs". Lancet neurology. 11 (9): 792–802. doi:10.1016/S1474-4422(12)70153-9. PMID 22832500.
- ^ Kamyar, M.; Varner, M. (Jun 2013). "Epilepsy in pregnancy". Clin Obstet Gynecol. 56 (2): 330–41. doi:10.1097/GRF.0b013e31828f2436. PMID 23563876.
- Lawrence S. Neinstein, ed. (2008). Adolescent health care : a practical guide (5th ed. ed.). Philadelphia: Lippincott Williams & Wilkins. p. 335. ISBN 978-0-7817-9256-1.
{{cite book}}:|edition=has extra text (help) - Duncan, JS (1 April 2006). "Adult epilepsy". Lancet. 367 (9516): 1087–100. doi:10.1016/S0140-6736(06)68477-8. PMID 16581409.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Duncan, JS (April 2007). "Epilepsy surgery". Clinical medicine (London, England). 7 (2): 137–42. doi:10.7861/clinmedicine.7-2-137. PMID 17491501.
- Birbeck GL, Hays RD, Cui X, Vickrey BG. (2002). "Seizure reduction and quality of life improvements in people with epilepsy". Epilepsia. 43 (5): 535–538. doi:10.1046/j.1528-1157.2002.32201.x. PMID 12027916.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Bergey, GK (June 2013). "Neurostimulation in the treatment of epilepsy". Experimental neurology. 244: 87–95. doi:10.1016/j.expneurol.2013.04.004. PMID 23583414.
- ^ Levy, RG; Cooper, PN; Giri, P (14 March 2012). "Ketogenic diet and other dietary treatments for epilepsy". The Cochrane database of systematic reviews. 3: CD001903. doi:10.1002/14651858.CD001903.pub2. PMID 22419282.
- , Bernard L. Maria (2009). Current management in child neurology (4th ed. ed.). Hamilton, Ont.: BC Decker. p. 180. ISBN 978-1-60795-000-4.
{{cite book}}:|edition=has extra text (help);|last=has generic name (help) - Arida, RM; Scorza, FA; Scorza, CA; Cavalheiro, EA (March 2009). "Is physical activity beneficial for recovery in temporal lobe epilepsy? Evidences from animal studies". Neuroscience and biobehavioral reviews. 33 (3): 422–31. doi:10.1016/j.neubiorev.2008.11.002. PMID 19059282.
- Arida, RM (2008). "Physical activity and epilepsy: proven and predicted benefits". Sports medicine (Auckland, N.Z.). 38 (7): 607–15. doi:10.2165/00007256-200838070-00006. PMID 18557661.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - Verrotti, A; Tocco, AM; Salladini, C; Latini, G; Chiarelli, F (November 2005). "Human photosensitivity: from pathophysiology to treatment". European journal of neurology : the official journal of the European Federation of Neurological Societies. 12 (11): 828–41. doi:10.1111/j.1468-1331.2005.01085.x. PMID 16241971.
- Doherty, MJ; Haltiner, AM (23 January 2007). "Wag the dog: skepticism on seizure alert canines". Neurology. 68 (4): 309. doi:10.1212/01.wnl.0000252369.82956.a3. PMID 17242343.
- Tan, G; Thornby, J; Hammond, DC; Strehl, U; Canady, B; Arnemann, K; Kaiser, DA (July 2009). "Meta-analysis of EEG biofeedback in treating epilepsy". Clinical EEG and neuroscience : official journal of the EEG and Clinical Neuroscience Society (ENCS). 40 (3): 173–9. doi:10.1177/155005940904000310. PMID 19715180.
- Cheuk, DK; Wong, V (8 October 2008). "Acupuncture for epilepsy". The Cochrane database of systematic reviews (4): CD005062. doi:10.1002/14651858.CD005062.pub3. PMID 18843676.
- Ramaratnam, S; Baker, GA; Goldstein, LH (16 July 2008). "Psychological treatments for epilepsy". The Cochrane database of systematic reviews (3): CD002029. doi:10.1002/14651858.CD002029.pub3. PMID 18646083.
- Ranganathan, LN; Ramaratnam, S (18 April 2005). "Vitamins for epilepsy". The Cochrane database of systematic reviews (2): CD004304. doi:10.1002/14651858.CD004304.pub2. PMID 15846704.
- Ramaratnam, S; Sridharan, K (2000). "Yoga for epilepsy". The Cochrane database of systematic reviews (3): CD001524. doi:10.1002/14651858.CD001524. PMID 10908505.
- Gloss, D; Vickrey, B (13 June 2012). "Cannabinoids for epilepsy". The Cochrane database of systematic reviews. 6: CD009270. doi:10.1002/14651858.CD009270.pub2. PMID 22696383.
- Brigo, F (13 June 2012). "Melatonin as add-on treatment for epilepsy". The Cochrane database of systematic reviews. 6: CD006967. doi:10.1002/14651858.CD006967.pub2. PMID 22696363.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Kwan, Patrick (2012). Fast facts : epilepsy (5th ed. ed.). Abingdon, Oxford, UK: Health Press. p. 10. ISBN 1-908541-12-1.
{{cite book}}:|edition=has extra text (help) - ^ Hitiris N, Mohanraj R, Norrie J, Brodie MJ (2007). "Mortality in epilepsy". Epilepsy Behavior. 10 (3): 363–376. doi:10.1016/j.yebeh.2007.01.005. PMID 17337248.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Moshé, edited by Simon Shorvon, Emilio Perucca, Jerome Engel Jr. ; foreword by Solomon (2009). The treatment of epilepsy (3rd ed. ed.). Chichester, UK: Wiley-Blackwell. p. 28. ISBN 978-1-4443-1667-4.
{{cite book}}:|edition=has extra text (help);|first=has generic name (help)CS1 maint: multiple names: authors list (link) - ^ Bagary, M (April 2011). "Epilepsy, antiepileptic drugs and suicidality". Current opinion in neurology. 24 (2): 177–82. doi:10.1097/WCO.0b013e328344533e. PMID 21293270.
- Mula, M; Sander, JW (August 2013). "Suicide risk in people with epilepsy taking antiepileptic drugs". Bipolar disorders. 15 (5): 622–7. doi:10.1111/bdi.12091. PMID 23755740.
- ^ Ryvlin, P; Nashef, L; Tomson, T (May 2013). "Prevention of sudden unexpected death in epilepsy: a realistic goal?". Epilepsia. 54 Suppl 2: 23–8. doi:10.1111/epi.12180. PMID 23646967.
- Hirtz D, Thurman DJ, Gwinn-Hardy K, Mohamed M, Chaudhuri AR, Zalutsky R (2007-01-30). "How common are the 'common' neurologic disorders?". Neurology. 68 (5): 326–37. doi:10.1212/01.wnl.0000252807.38124.a3. PMID 17261678.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Sander JW (2003). "The epidemiology of epilepsy revisited". Current Opinion in Neurology. 16 (2): 165–70. doi:10.1097/00019052-200304000-00008. PMID 12644744.
- ^ Saraceno, B; Avanzini, G; Lee, P, eds. (2005). Atlas: Epilepsy Care in the World (PDF). World Health Organization. ISBN 92-4-156303-6. Retrieved 20 December 2013.
- Mervyn J. Eadie; Peter F. Bladin (2001). A Disease Once Sacred: A History of the Medical Understanding of Epilepsy. John Libbey Eurotext. ISBN 978-0-86196-607-3.
- "Epilepsy: An historical overview". World Health Organization. Feb 2001. Retrieved 27 December 2013.
- "Epilepsy: historical overview". World Health Organization. Retrieved 2011-03-20.
- ^ Jilek-Aall, L (1999). "Morbus sacer in Africa: some religious aspects of epilepsy in traditional cultures". Epilepsia. 40 (3): 382–6. doi:10.1111/j.1528-1157.1999.tb00723.x. PMID 10080524.
- Illes, Judika (2011-10-11). Encyclopedia of Mystics, Saints & Sages. HarperCollins. p. 1238. ISBN 978-0-06-209854-2. Retrieved 26 February 2013.
Saint Valentine is invoked for healing as well as love. He protects against fainting and is requested to heal epilepsy and other seizure disorders. In northern Italy, epilepsy was once traditionally known as Saint Valentine's Malady.
- E. Martin Caravati (2004). Medical toxicology (3. ed. ed.). Philadelphia : Lippincott Williams & Wilkins. p. 789. ISBN 978-0-7817-2845-4.
{{cite book}}:|edition=has extra text (help) - ^ de Boer, HM (Dec 2010). "Epilepsy stigma: moving from a global problem to global solutions". Seizure : the journal of the British Epilepsy Association. 19 (10): 630–6. doi:10.1016/j.seizure.2010.10.017. PMID 21075013.
- Martindale, JL; Goldstein, JN; Pallin, DJ (February 2011). "Emergency department seizure epidemiology". Emergency medicine clinics of North America. 29 (1): 15–27. doi:10.1016/j.emc.2010.08.002. PMID 21109099.
- ^ Jerome Engel, Jr., Timothy A. Pedley, ed. (2008). Epilepsy : a comprehensive textbook (2nd ed. ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 2279. ISBN 978-0-7817-5777-5.
{{cite book}}:|edition=has extra text (help)CS1 maint: multiple names: editors list (link) - Bor, Robert (2012). Aviation Mental Health: Psychological Implications for Air Transportation. Ashgate Publishing. p. 148. ISBN 978-1-4094-8491-2.
- ^ "Seizure Disorders". Transport Canada. Government of Canada. Retrieved 29 December 2013.
- Wilner, Andrew N. (2008). Epilepsy 199 answers : a doctor responds to his patients' questions (3rd ed. ed.). New York: Demos Health. p. 52. ISBN 978-1-934559-96-3.
{{cite book}}:|edition=has extra text (help) - "Guide for Aviation Medical Examiners". Federal Aviation Administration. Retrieved 29 December 2013.
- ^ "National PPL (NPPL) Medical Requirements". Civil Aviation Authority. Retrieved 29 December 2013.
- Drivers Medical Group (2013). "For Medical Practitioners: At a glance Guide to the current Medical Standards of Fitness to Drive" (PDF). p. 8. Retrieved 29 December 2013.
- "Epilepsy Foundation of America - EFA". Healthfinder.gov. US Department of Health and Human Services. April 28, 2011. Retrieved July 28, 2014.
- al.], editors, Jerome Engel, Jr., Timothy A. Pedley ; associate editors, Jean Aicardi ... [et (2008). Epilepsy : a comprehensive textbook (2nd ed. ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 2245. ISBN 9780781757775.
{{cite book}}:|edition=has extra text (help);|first1=has generic name (help)CS1 maint: multiple names: authors list (link) - ^ Carney, PR.; Myers, S.; Geyer, JD. (Dec 2011). "Seizure prediction: methods". Epilepsy Behav. 22 Suppl 1: S94-101. doi:10.1016/j.yebeh.2011.09.001. PMID 22078526.
- Jerome Engel, ed. (2008). Epilepsy : a comprehensive textbook (2nd ed. ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 426. ISBN 9780781757775.
{{cite book}}:|edition=has extra text (help) - Walker, MC.; Schorge, S.; Kullmann, DM.; Wykes, RC.; Heeroma, JH.; Mantoan, L. (Sep 2013). "Gene therapy in status epilepticus". Epilepsia. 54 Suppl 6: 43–5. doi:10.1111/epi.12275. PMID 24001071.
- Walker, L; Pirmohamed, M; Marson, AG (27 June 2013). "Immunomodulatory interventions for focal epilepsy syndromes". The Cochrane database of systematic reviews. 6: CD009945. doi:10.1002/14651858.CD009945.pub2. PMID 23803963.
- Quigg, M; Rolston, J; Barbaro, NM (Jan 2012). "Radiosurgery for epilepsy: clinical experience and potential antiepileptic mechanisms". Epilepsia. 53 (1): 7–15. doi:10.1111/j.1528-1167.2011.03339.x. PMID 22191545.
- Thomas, WB (January 2010). "Idiopathic epilepsy in dogs and cats". Veterinary Clinics of North America, Small Animal Practice. 40 (1): 161–79. doi:10.1016/j.cvsm.2009.09.004. PMID 19942062.
- Thomas, WB (Jan 2010). "Idiopathic epilepsy in dogs and cats". The Veterinary clinics of North America. Small animal practice. 40 (1): 161–79. doi:10.1016/j.cvsm.2009.09.004. PMID 19942062.
- Rundfeldt, C; Loescher, W (January 2014). "The pharmacology of imepitoin: The first partial benzodiazepine receptor agonist developed for the treatment of epilepsy". CNS Drugs. 28 (1): 29–43. doi:10.1007/s40263-013-0129-z. PMID 24357084.
- van der Ree, M; Wijnberg, I (2012). "A review on epilepsy in the horse and the potential of Ambulatory EEG as a diagnostic tool". The Veterinary quarterly. 32 (3–4): 159–67. doi:10.1080/01652176.2012.744496. PMID 23163553.
Further reading
- National Institute for Health and Clinical Excellence (January 2012). The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care (PDF). National Clinical Guideline Centre.
- World health organization, Department of mental health and substance abuse, Programme for neurological diseases and neuroscience ; Global campaign against epilepsy ; International league against epilepsy (2005). Atlas, epilepsy care in the world, 2005 (pdf). Geneva: Programme for Neurological Diseases and Neuroscience, Department of Mental Health and Substance Abuse, World Health Organization. ISBN 92-4-156303-6.
{{cite book}}: CS1 maint: multiple names: authors list (link)
External links
| Diseases of the nervous system, primarily CNS | |||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Inflammation |
| ||||||||||||||||||||||||
| Brain/ encephalopathy |
| ||||||||||||||||||||||||
| Both/either |
| ||||||||||||||||||||||||
| Seizures and epilepsy | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Basics | |||||||||
| Management |
| ||||||||
| Personal issues | |||||||||
| Seizure types |
| ||||||||
| Related disorders | |||||||||
| Organizations | |||||||||